Dental Implants vs. Bridges: Cost, recovery, and which option is best for your smile
Dental Implants vs. Bridges: Cost, recovery, and which option is best for your smile
When a missing tooth needs replacing, choosing between dental implants vs bridges is a decision that affects your smile, budget, and long term oral health. This article explains how each option works, realistic upfront and lifetime costs, typical recovery timelines, and the clinical factors that should guide your choice. It also includes practical examples and next steps for patients in the Houston metro area considering treatment at a local practice.
Head to head at a glance
Quick take: Implants replace the tooth at the root level and anchor a crown to bone; bridges replace only the visible tooth and rely on adjacent teeth for support. When you weigh dental implants vs bridges, think about mechanics first — that difference drives everything from bone health to long term stability.
Side-by-side snapshot
- Mechanics: Implant = fixture in bone + abutment + crown. Bridge = pontic suspended between prepared abutment crowns.
- Effect on neighbors: Implants spare adjacent teeth. Bridges require reshaping healthy teeth and can accelerate future work on those teeth.
- Bone preservation: Implants transmit functional load to the jaw and reduce resorption. Bridges leave the underlying ridge unsupported.
- Timeline and recovery: Implant workflows require surgical healing and often months before final crown; bridges can be completed in fewer appointments and days of soft-tissue recovery.
- Maintenance and failure modes: Implants need peri-implant care and monitoring for peri-implantitis; bridges need vigilant hygiene under the pontic to prevent decay and failure of abutments.
- Aesthetics and function: Both can look excellent; implants usually win on long-term stability and chewing force, bridges are faster when immediate results matter.
Practical tradeoff: Choosing implants buys long-term biological benefits but accepts surgery, longer treatment time, and upfront commitments like CBCT planning or possible grafting. Choosing a bridge reduces surgical risk and shortens the path to a finished tooth, but you trade away some future options and add risk to the teeth you rely on as anchors.
Concrete example: A 52-year-old with a single missing lower molar and good bone on CBCT can often receive a Straumann or comparable implant at Smile Avenue, wait through osseointegration, then get a final crown — the result restores bite force without touching adjacent teeth. By contrast, an 80-year-old with cardiac comorbidity who needs a quick, non-surgical fix may receive a three-unit bridge using zirconia crowns to avoid any oral surgery.
Judgment that matters: Patients frequently assume bridges are always cheaper long term. In practice, repeated bridge replacements and downstream work on abutment teeth can erase that short-term saving. If preserving bone and minimizing future restorative cascade matter to you, implants are often the more conservative clinical choice — assuming you are a suitable surgical candidate.
How dental implants restore missing teeth
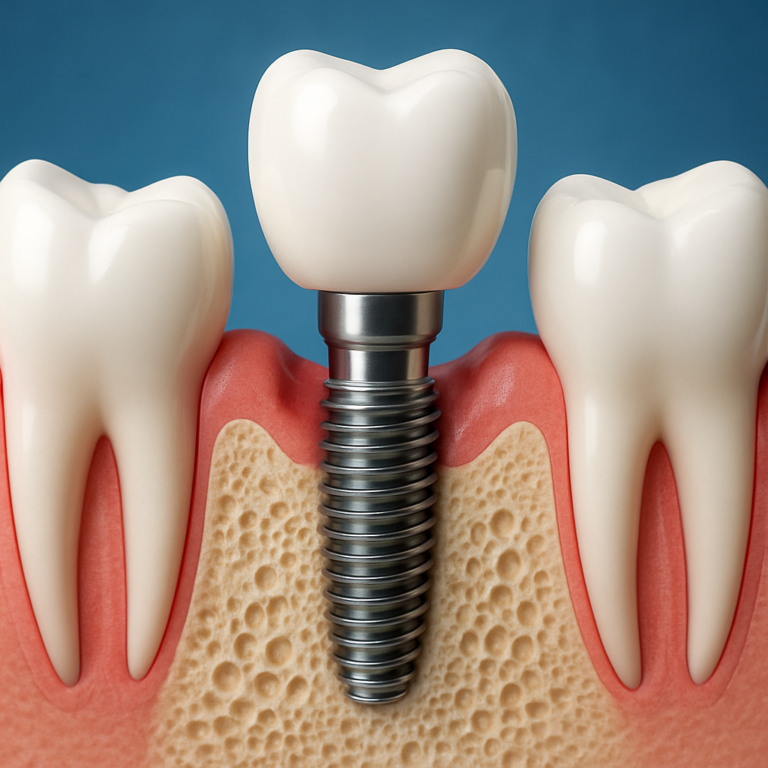
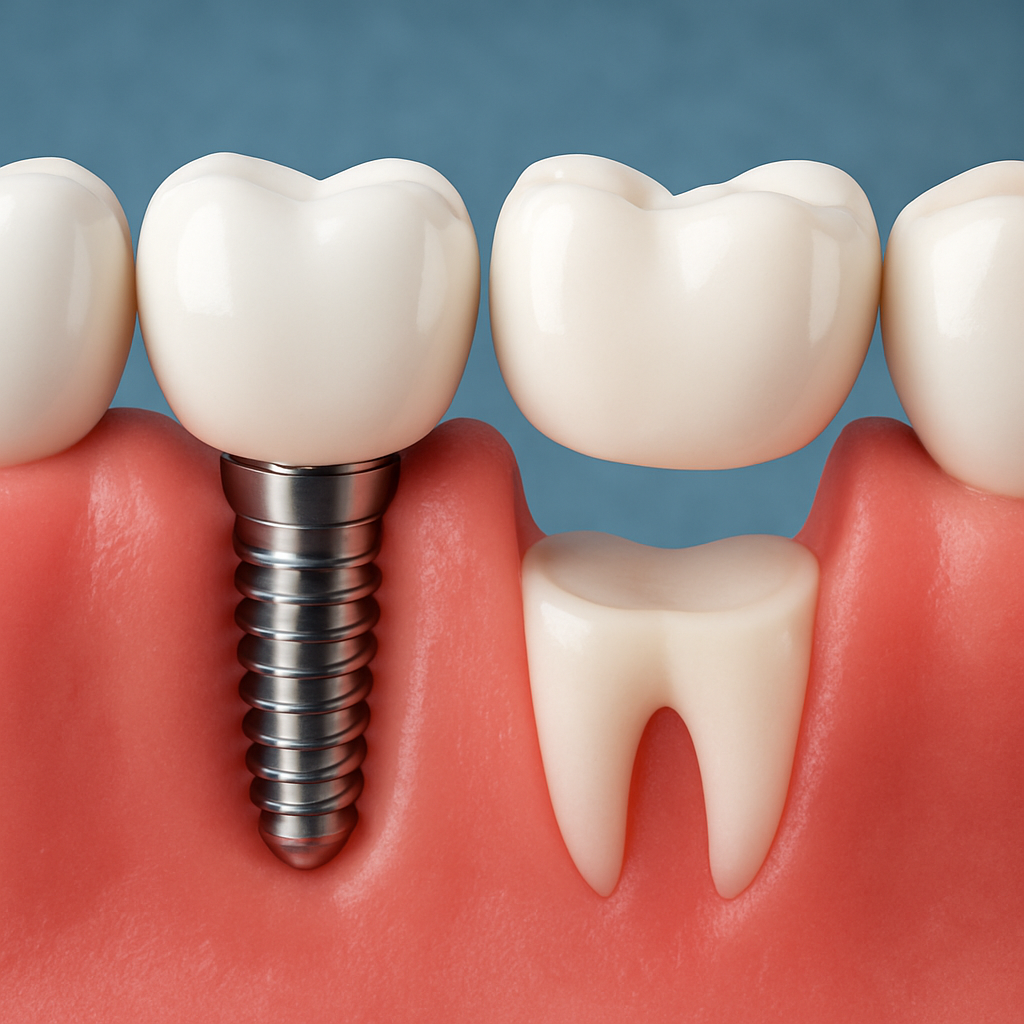
Direct replacement of the root changes the biology. A dental implant is a biocompatible fixture (usually titanium or zirconia) placed into the jawbone, then restored with an abutment and crown. That root-level support is the practical reason implants behave differently than any prosthetic that simply spans a gap.
Surgical and restorative workflow in practice
Planning and placement: Modern implant workflows start with a CBCT scan and intraoral digital scan to map bone volume, sinus position, and the restorative envelope. Guided placement or freehand can both work; the clinical decision is driven by anatomy, prosthetic demands, and whether immediate provisionalization is desirable. Smile Avenue uses CBCT during planning to decide if a staged graft, sinus lift, or immediate load is appropriate — see Dental implants for our process.
Osseointegration versus immediate load: Traditional sequencing leaves the implant unloaded for weeks to months to secure osseointegration. Immediate loading (a crown or temporary attached at placement) is attractive but only predictable when primary stability and bone quality meet specific thresholds. In my experience, immediate provisionalization works well in the anterior when it preserves soft tissue contours, but I avoid it on wide molar sites with poor bone density.
Biologic, functional, and esthetic consequences
Bone preservation is the steady advantage. Implants transmit chewing forces into bone and reduce the degree of alveolar resorption beneath the replaced tooth. That matters clinically: less ridge collapse simplifies future prosthetic work and preserves facial contours. The tradeoff is surgical complexity — where bone is thin you will often need grafting, which adds time and cost and slightly raises the risk of complications.
Soft tissue and esthetics matter more than people expect. For front teeth, getting the gingival margin and papilla right requires planning the emergence profile and often a provisional crown to shape tissue. A poorly planned implant in the esthetic zone can look worse than a well-executed bridge because the gum architecture is more challenging to reconstruct than to mimic with a pontic.
Maintenance and failure modes to weigh: Implants eliminate decay risk on an extracted site but introduce risks like peri-implant mucositis and peri-implantitis. Mechanically, screw loosening and prosthetic fractures are the common issues. Good hygiene, regular professional maintenance, and risk-factor control (smoking cessation, diabetes management) are not optional if you want longevity.
Concrete example: A 37-year-old patient lost an upper central incisor in a sports accident. CBCT showed a thin buccal plate; the team performed a ridge augmentation and placed an implant with a provisional crown to preserve the papilla. The staged approach cost more and took longer, but it avoided a visible gingival recession that would have required secondary soft-tissue grafting had a faster protocol been chosen.
Practical judgment: Implants are a restorative strategy — not just a piece of hardware. The best outcomes come from integrating surgical planning, provisionalization strategy, and prosthetic design up front. Cheap shortcuts on grafting, implant position, or provisional shaping often cost more later.
How dental implants restore missing teeth
Root-level replacement changes predictable outcomes. When you replace the missing tooth root with an implant fixture, how chewing forces travel through the jaw changes — and that single fact explains the majority of clinical differences between implants and any tooth-spanning prosthesis.
Prosthetic decisions that determine function and longevity
Screw-retained versus cement-retained matters. Screw-retained crowns and bridges are retrievable for repairs and make managing biological complications easier; cement-retained restorations can hide excess cement and raise the risk of peri-implant inflammation. Choosing a custom titanium or zirconia abutment influences esthetics in the anterior and soft-tissue support around the emergence profile.
Platform switching and implant surface choices affect crestal bone. Modern implant designs that use platform switching and roughened surfaces promote more stable bone levels than older straight-abutment systems. Those engineering differences are small at placement but compound over years and matter when you compare dental implants vs bridges longevity in the real world.
Clinical limits and tradeoffs to weigh
Medical and anatomic constraints change the plan, not the principle. Heavy smokers, patients on certain antiresorptive medications, or those with uncontrolled systemic disease have higher complication rates; sometimes the right choice is a bridge because surgery carries unacceptable risk. When bone is narrow or close to the sinus or inferior alveolar nerve, narrow-diameter implants, staged grafting, or angled abutments are practical workarounds — but they add cost and clinical steps.
- Common prosthetic routes: single implant crown, implant-supported fixed bridge, and implant-retained overdenture
- When to prefer implant-supported bridge: when multiple adjacent teeth are missing and placing individual fixtures is anatomically or financially impractical
- When a single implant is better: when neighboring teeth are healthy and you want to avoid preparing them
Biomechanics create hidden costs. A three-unit implant-supported bridge transfers load differently than two single crowns; span length, cantilever presence, and opposing dentition determine whether you need extra fixtures. Economizing by using fewer implants can raise mechanical risk and long-term maintenance needs.
Concrete example: A 40-year-old patient missing the two lower right molars on the same side had adequate bone but limited budget. We discussed two paths: place two single implants to preserve individual root mechanics, or place an implant-supported two-unit bridge on two fixtures. The team chose two single implants because the occlusal forces in the posterior and the patient's bruxism history made separate fixtures more durable over a decade.
Maintenance is procedural, not optional. Expect periodic torque checks, occasional screw retightening, and focussed hygiene under prostheses with a proxabrush or water flosser. Retrievability built into the prosthetic design reduces the need to remove a crown to regain access for repair — that design choice often saves more money over time than the marginal cost of a custom abutment.
Next consideration: Before you choose between an implant or a bridge, confirm the prosthetic plan: which abutment material, whether restorations will be screw-retained, and how many fixtures the bite mechanics actually require — those specifics change cost, recovery, and long-term durability more than the headline label dental implant vs bridge.
Cost comparison and what drives price differences
Upfront price is only one axis. When you compare dental implants vs bridges, the real cost picture combines immediate fees, predictable add-ons, and the probability of future repairs or replacements. Focus on what you are paying for, not just the bottom line: imaging and surgical complexity, prosthetic design choices, and the expected service life of the restoration all shift value.
What moves the needle on price
| Cost driver | How it affects implants | How it affects bridges |
|---|---|---|
| Advanced imaging and planning | CBCT and guided surgical planning increase planning fees but reduce surgical risk and complications. | Often limited to 2D or digital scans; less planning cost but also fewer predictive safeguards. |
| Bone grafting / sinus lift | Can add significant expense and months to treatment when bone volume is insufficient. | Generally not required for bridge placement; saving here may be offset by future work on abutment teeth. |
| Implant system and abutment type | Premium systems and custom zirconia or titanium abutments raise costs; screw-retained options add lab work but simplify maintenance. | Crown material (zirconia, lithium disilicate, PFM) and pontic design drive lab costs. |
| Surgery vs prosthetic work | Operating time, sedation option, and surgical skill factor into cost. | Tooth preparation time and lab fabrication are the main cost centers. |
| Long-term maintenance | Periodic maintenance, potential peri-implantitis treatment, and occasional prosthetic repairs create predictable visits. | Replacements, endodontic treatment on abutments, or crowns on failing supporting teeth create downstream expense. |
Practical tradeoff: implants often shift cost from recurring restorative cycles to initial surgical and prosthetic investment. Bridges concentrate expense in smaller, earlier payments but increase the chance of future procedures on adjacent teeth. That tradeoff matters if you plan to keep the tooth replacement for decades or if your budget is short-term.
Concrete example: A 55-year-old patient missing an upper first molar had borderline sinus height on CBCT. Choosing an implant required a sinus lift and staged healing, which lengthened the timeline and added surgical fees. The alternative — a three-unit bridge — avoided surgery but meant reducing two otherwise healthy premolars; within seven years one of those premolars required a root canal and crown, increasing total treatment expense and complexity.
Common mistake patients make: people fixate on sticker price and ignore failure cascade risk. A cheaper bridge can become more expensive when abutment teeth deteriorate or when repeated bridge replacements are needed. Conversely, obsessing over brand names for implants beyond documented performance rarely improves outcomes; ask how the choice affects warranties, component compatibility, and retrievability instead.
If you want specifics for the Houston metro area, bring prior records and insurance info to a consult so your provider can run a CBCT-based plan and show alternatives with firm, itemized pricing. For more on implant planning see Dental implants and for independent guidance consult the American Dental Association.
Recovery, healing timeline, and aftercare for implants and bridges
Direct point: choosing between dental implants vs bridges is as much about the recovery and daily upkeep as it is about cost or appearance. The two treatments demand very different short-term behaviors and long-term maintenance habits; those differences often determine whether a restoration lasts or becomes another bill.
Implant recovery: staged healing and what to expect
Early phase (first week): expect localized swelling, bruising, and soreness for 48–72 hours. Cold packs, short course analgesics, and a soft diet reduce complications. If sutures were placed, they are usually removed or dissolve between 7 and 14 days.
Bone integration (weeks to months): the implant must osseointegrate to the jaw. Typical clinical windows run from approximately 8 to 16 weeks in mandibular sites to 12 to 24 weeks in maxillary sites, depending on bone quality. Immediate loading—attaching a provisional crown at placement—works but should be reserved for cases with measured primary stability (often >30–35 Ncm) and favorable bone.
Bridge recovery: fast finish, different responsibilities
Single-visit impact: tooth preparation and temporization usually create only days of sensitivity and soft-tissue settling. Most patients return to normal eating within a few days, and the final crown is delivered in one to two weeks.
Hidden demands: a bridge spares you surgery but places long-term responsibility on the abutment teeth. Aftercare focuses on cleaning under the pontic and monitoring margins; failure here is often biologic (decay or endodontic failure) rather than surgical.
Practical aftercare checklist (what actually changes day-to-day)
- First two weeks after implant placement: soft diet, avoid heavy lifting and smoking, take prescribed antibiotics or analgesics as directed, and keep the site gently clean with saline or a chlorhexidine rinse if recommended.
- Daily hygiene for implants: brush twice, use an interdental brush or floss around the implant-abutment junction, and consider a water flosser to manage biofilm; avoid abrasive pastes on healing tissue.
- Daily hygiene for bridges: floss using a floss threader or specialized tape under the pontic every day, inspect margins for staining or odor, and report any increased sensitivity or bad taste promptly.
- Professional care: expect hygiene visits every 3–6 months for implants (risk-based) and similar or slightly more frequent checks for bridges to catch margin problems early.
- Para-functional protection: wear a night guard if you grind; both implants and bridges fail faster under unmanaged bruxism.
Tradeoff to understand: implants shift risk from tooth decay to biological and mechanical complications (peri-implantitis, screw loosening). Bridges shift risk onto natural teeth—so your oral hygiene skill and periodontal status matter more with a bridge than people usually appreciate.
Real-world case: a 58-year-old patient received a single posterior implant. They used a strict soft-food protocol and stopped smoking for six weeks; sutures were removed at 10 days and the final crown placed at four months with stable bone levels on follow-up radiographs. The avoidance of prepping adjacent premolars preserved their long-term integrity and saved the patient a later root-canal procedure.
Next consideration: before committing, ask your clinician for a site-specific recovery plan with measurable checkpoints (suture removal date, radiographic review, provisional-to-final timeline) and an itemized aftercare protocol — that plan predicts outcomes more reliably than sticker price.
Clinical candidacy and decision criteria
Core assertion: candidacy for an implant is a clinical judgement that balances local anatomy, medical risk, and what the patient values most. When you compare dental implants vs bridges, the right answer often follows from those three factors—not from price alone.
Local anatomy matters first. Adequate bone volume, the thickness of the buccal plate, soft tissue quality, and the condition of neighboring teeth drive whether an implant is predictable. Small defects are routinely corrected with ridge grafts, but proximity to the sinus or the inferior alveolar nerve forces different surgical choices and sometimes staged treatment. At Smile Avenue we require a CBCT and intraoral scan before recommending either route; the imaging changes the plan more often than patient preference does. See Dental implants for our diagnostic workflow.
Medical and behavioral factors change probability, not possibilities. Controlled chronic disease, including well-managed diabetes, is not an automatic implant exclusion. Heavy smoking, uncontrolled systemic conditions, recent intravenous bisphosphonate therapy, and poor oral hygiene raise failure risk and push the recommendation toward less invasive options. Coordinate with your physician; many conditions can be optimized so an implant becomes a reasonable long-term choice.
Patient goals and timing are decisive. If preserving neighboring tooth structure and avoiding future restorative cascades is your priority, implants usually win. If you need a non-surgical, faster solution because of medical constraints, budget, or immediate aesthetic need, a bridge can be the right choice—provided the bridge is designed to preserve future options. A poorly planned, overcontoured bridge will make a later implant much harder.
Concrete example: A 58 year old patient with controlled type 2 diabetes and a missing upper lateral tooth presented to our Cypress office. CBCT showed a thin buccal ridge; after risk review we recommended staged grafting and an implant to secure papilla and long term esthetics. The patient accepted a conservative resin bonded bridge as a temporary while scheduling the graft, which preserved adjacent tooth structure and kept the implant option intact.
A quick decision framework you can use in consultation
- Score each item yes=1/no=0: Adequate bone on CBCT; healthy periodontal support; controlled systemic health; willing to accept surgery and longer timeline; priority on long-term stability. Tally the score.
- Interpretation: 4–5 = implant favored; 2–3 = shared decision with emphasis on patient priorities and possible staged plan; 0–1 = bridge or removable option recommended with management of risk factors first.
- Practical tweak: If you score 2–3 but plan to upgrade to an implant later, insist on a bridge design that minimizes preparation depth and avoids subgingival margins to preserve the ridge for future implant placement.
Practical tradeoff worth stating plainly: implants buy preservation of bone and independence from neighboring teeth; they require surgery, time, and ongoing peri-implant maintenance. Bridges avoid surgery and provide a faster finish but increase the chance of future work on abutment teeth and can complicate later implant therapy if executed without foresight.
Longevity, complications, and maintenance expectations
Straight to the point: an implant changes the biology of the site; a bridge leaves the biology as-is and borrows support from neighbor teeth. That mechanical difference is why implants tend to remain serviceable for many more years than bridges, but it does not mean implants are carefree or risk-free.
What typically goes wrong — and how we catch it early
Implant complications are biological and mechanical. On the biological side the main threat is peri-implant inflammation that, if ignored, progresses to bone loss around the fixture. Mechanically you will see loose screws, fractured prosthetic components, or wear of the crown. The fix is different for each: early mucosal inflammation responds to hygiene and local debridement; progressive bone loss sometimes needs surgical revision and antimicrobial therapy; mechanical problems usually require a clinic visit for tightening, repair, or replacement.
Bridge complications are mostly on the abutment teeth. Recurrent decay at margins, loss of retention, or secondary fracture of a supporting tooth are the failure cascade you want to avoid. When an abutment tooth fails, treatment typically becomes more complex and expensive — often converting a previously simple bridge case into an implant or a removable solution that demands additional surgery or prosthetic redesign.
- Signals you should bring to your dentist now: bleeding around the restoration, a persistent bad taste or odor under a pontic, any mobility of an implant crown or abutment tooth, and exposure of implant threads or visible bone.
- Monitoring that matters: baseline radiographs at delivery, targeted radiographic checks thereafter, and risk-adjusted hygiene recalls that keep biofilm and marginal disease under control.
- Design choices that reduce future work: retrievable (screw-retained) implant restorations for easier repairs; shallow, cleanable subgingival margins on bridges to limit recurrent decay; controlled occlusion to reduce mechanical overload.
Practical tradeoff: implants move the maintenance burden toward surveillance for infection and mechanical checks; bridges move it toward everyday sub-pontic hygiene and the long-term health of adjacent teeth. If you struggle with daily flossing or have active gum disease, a bridge may fail sooner than anticipated; conversely, if you smoke or have uncontrolled systemic disease, an implant is higher risk and may demand more interventions.
Concrete example: a patient in their late 60s chose a three-unit bridge because they wanted to avoid surgery. Five years later one abutment developed deep decay under the crown and needed extraction; the patient then required an implant in a narrower ridge, which meant a graft and a longer, more expensive course than if an implant had been placed initially with staged augmentation. That sequence is common in practice and explains why short-term savings can convert to greater lifetime cost and morbidity.
Next consideration: before you commit, get a written maintenance and surveillance plan that names follow-up intervals, who performs the maintenance (hygienist versus specialist), and the likely costs of predictable repairs — that document changes the calculus more than the initial price tag.
Decision framework with three patient scenarios and local next steps
Start with the clinical constraint, not the price. For most patients the right path is determined by three things: local anatomy on CBCT, medical and behavioral risk, and the timeline or budget you can accept. Below are three realistic patient profiles you can map to an evidence based recommendation, followed by concrete local actions to move forward at Smile Avenue in Cypress or Katy.
Scenario A — Implant-first: healthy, long-term priority
When this fits: healthy adult, adequate bone or willing to undergo grafting, controlled medical conditions, and a goal of avoiding alteration of adjacent teeth.** The clinical logic is preservation: replacing the root preserves bone and reduces the chance of a restorative cascade on neighbors. The tradeoff is a longer timeline because staged grafts or osseointegration can add weeks to months and require surgical healing.
Real-world case: A 45 year old non smoker with a single posterior tooth missing had sufficient bone on CBCT. We planned a guided implant using a Straumann compatible system, placed a provisional where appropriate, and staged the final crown after stable integration. The patient accepted the longer timeline to avoid prepping healthy molars and to preserve future options.
Scenario B — Bridge-first: medical or timing constraints
When this fits: patients with significant medical contraindications to surgery, those who need a fast finish, or when neighboring teeth already require crowns.** Choosing a fixed bridge reduces surgical risk and shortens the path to a finished tooth, but it transfers future risk to the abutment teeth. That tradeoff is acceptable when surgical risk outweighs long-term preservation goals.
Real-world case: An older patient with cardiac comorbidity and two premolars already restored chose a three unit zirconia bridge at our Katy office. The team prioritized shallow margins and a design that would make eventual implant conversion simpler if needed.
Scenario C — Phased or hybrid plan: constrained budget or modifiable risks
When this fits: younger patients with parafunction, heavy smokers willing to attempt behavior change, or those who need to spread cost over time.** A staged approach can start with a conservative bridge or a resin bonded temporary that preserves bone and adjacent tooth structure while you manage smoking, bruxism, or finances. This keeps the implant option open rather than burning bridges, literally and figuratively.
Real-world case: A 30 year old bruxer on a tight budget elected a minimally invasive Maryland style provisional while committing to a night guard and smoking cessation. Once bruxism was controlled the plan moved to an implant with appropriate augmentation.
- Local next steps at Smile Avenue: Schedule a CBCT based consult at our Cypress or Katy location to map bone and soft tissue.
- Bring this to the appointment: current meds, recent dental records and radiographs, and your insurance information to allow a realistic, itemized estimate.
- Discuss risks and timeline: ask specifically about grafting scenarios, immediate provisional options, and prosthetic retrievability so you can compare lifetime maintenance rather than sticker price.
Practical judgment: if your anatomy and health allow it, prioritize solutions that preserve future options. If not, choose the least destructive short term option and document a clear upgrade path.