What Are The Five Principles Of Oral Health?
Healthy teeth and gums don’t happen by chance—daily habits do the heavy lifting. Understanding the principles of oral hygiene helps turn “brush and floss” into a clear, repeatable routine that controls plaque, prevents cavities, and supports gum health for years to come.
Principles of Oral Hygiene: What They Are and Why They Matter
Define “principles of oral hygiene” in plain language
The principles of oral hygiene are the core, evidence-based habits that keep the mouth clean and protected day after day. They focus on reducing dental plaque, supporting healthy gums, and strengthening teeth so problems are less likely to start.
- Oral hygiene is daily, practical care—brushing, cleaning between teeth, and smart choices—that helps control bacteria and inflammation.
- These habits support long-term outcomes like fewer cavities, less gum disease, and better overall oral comfort.
- Even when teeth already have fillings or have been chipped, plaque can still contribute to new decay—so consistent principles still matter.
The “why” behind oral hygiene (mouth → whole body)
The mouth is more than a place to chew—it’s an entry point for germs and a starting line for inflammation. When plaque builds up, bacteria produce acids and irritants that can affect both teeth and gums.
- Oral germs can contribute to tooth decay and gum disease, and the inflammation from gum disease may influence the body’s overall response to infection.
- Research suggests links between gum health and conditions such as diabetes, pregnancy complications, and respiratory infections—often through inflammation and infection risk.
- Good oral hygiene helps keep the mouth’s microbial balance under control, which is one reason dental care is often described as part of whole-body wellness.
The goal: keep teeth for a lifetime
The goal of oral hygiene is not just “clean teeth today,” but prevention and early detection over time. Many dental problems begin quietly—so the best results come from consistent routines and timely professional check-ups.
- Prevention reduces the chance of needing more complex treatment later, including fillings, root canals, and periodontal therapy.
- Early detection helps dental professionals address small issues before they become painful or expensive.
- Even teeth with fillings or minor damage can develop new decay when plaque stays in place long enough to attack enamel and dentin.
The Main Cause: Dental Plaque and How It Leads to Problems
What plaque is and why it’s hard to see
Plaque is a sticky, colorless film of bacteria that forms on teeth every day. It’s hard to see with the naked eye, but it can be present even when the mouth looks “clean.”
When plaque remains on teeth, it can cause two major problems: tooth decay and gum disease. Plaque bacteria produce acids that can weaken enamel, and they also irritate gum tissue, which may lead to bleeding and swelling.
- Plaque buildup can be especially noticeable at the gumline, between teeth, and around dental work.
- Because plaque is sticky, it can cling to tooth surfaces and resist removal unless the right technique is used.
- Disclosing tablets or disclosing toothpaste can help reveal plaque areas so brushing can be targeted more effectively.
Plaque → gingivitis → periodontitis (progression)
When plaque irritates the gums, the earliest stage of gum disease is often gingivitis. Gingivitis may show up as red, swollen gums and bleeding when brushing or flossing.
Without consistent plaque control, gingivitis can progress to periodontitis, a more advanced condition where gum tissue and supporting bone can be affected. In periodontitis, symptoms may include persistent bad breath, gum recession, and in some cases looseness of teeth.
- Gingivitis is often reversible with daily brushing and interdental cleaning, but it requires consistency.
- Over time, plaque can harden into tartar (also called calculus), which is much harder to remove at home.
- Professional cleaning is important because tartar can sit below the gumline and keep inflammation going.
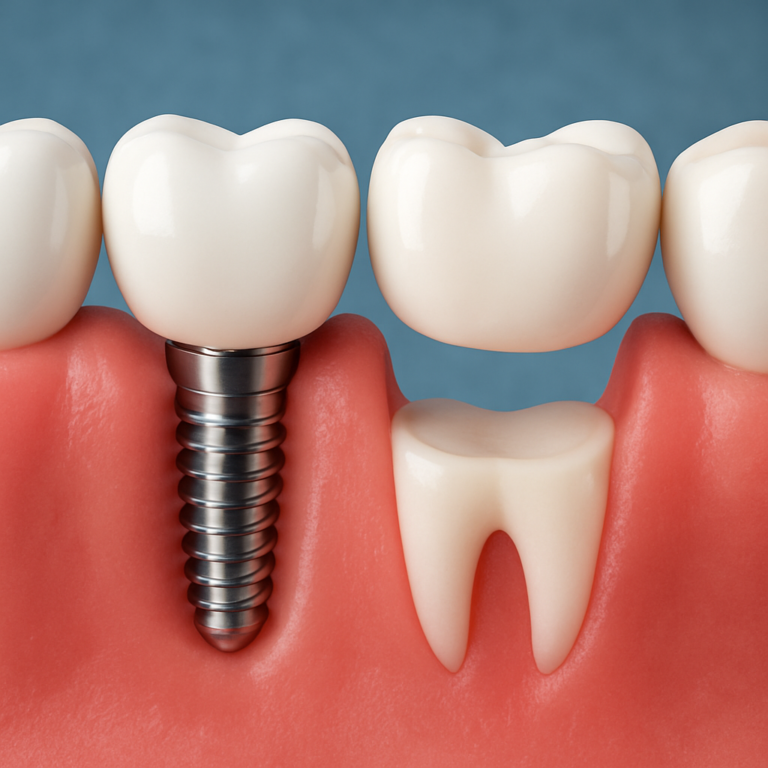
Special risk areas: gum recession, under fillings, and exposed roots
Not all tooth surfaces are equally easy to clean. Plaque often accumulates in “hidden” zones—like along the gumline, around crowns, and under edges of chipped or worn fillings.
When gums recede, the tooth’s root surface may become exposed. Root surfaces are covered by a different type of tissue than enamel, and they can be more vulnerable to decay when plaque and acids are present.
- Hard-to-reach areas can trap plaque even with good brushing, which is why interdental cleaning is a key principle.
- Under fillings and around chipped areas, plaque can contribute to new decay if the margins are not kept clean.
- Exposed roots can develop cavities, so gum recession should be treated as a reason to refine home care and schedule regular exams.
Brushing Principles of Oral Hygiene (Technique, Frequency, and Timing)
Brush twice daily with fluoride toothpaste—how and how long
Brushing is the foundation of daily plaque control. A core principle of oral hygiene is brushing twice a day with fluoride toothpaste, which helps protect enamel from acid attacks.
Most people do best with about 2 minutes per brushing session. Using a timer, a favorite song, or a phone app can make it easier to reach the full time without rushing.
- Brush once in the morning and once at night—night brushing is especially important because saliva flow can decrease during sleep.
- Spit out toothpaste after brushing, but avoid rinsing aggressively with water so fluoride can stay on the teeth longer.
- If nausea or sensitivity makes brushing difficult, your dental professional may suggest a different toothpaste or technique to improve comfort.
Best brushing technique details (angle, motion, coverage)
Technique matters because plaque forms where bristles can reach. For effective cleaning, the toothbrush should be angled toward the gumline so it can disrupt plaque between the gums and teeth.
Gentle, small circular motions are usually more effective than forceful scrubbing. Brushing too hard can irritate gums and wear down tooth surfaces over time.
- Use gentle pressure and focus on coverage: outer surfaces, inner surfaces, and chewing surfaces.
- Brush the tongue to help reduce odor-causing bacteria.
- Consider a soft-bristled brush; it’s typically easier on gums and enamel while still removing plaque.
Common brushing mistakes to avoid
Even well-intentioned brushing can fall short if the technique is rushed or too aggressive. Common mistakes include scrubbing back and forth, skipping hard-to-reach areas, or brushing for less than the recommended time.
Another frequent issue is using an old toothbrush. Worn bristles don’t clean as effectively, which can reduce plaque removal and increase the risk of gum irritation.
- Avoid hard, back-and-forth scrubbing—gentle motions protect gums and enamel.
- Replace the toothbrush (or brush head) about every 3–4 months, or sooner if bristles splay.
- If braces, implants, or gum recession are present, your dentist may recommend a specific brush type or additional tools.
Clean Between Teeth: Flossing and Interdental Cleaning Principles
Why “between teeth” matters
Toothbrush bristles can’t reach every surface. Plaque between teeth can irritate gums and may harden below the gumline if it isn’t removed regularly.
When interdental plaque stays in place, gums may become red, swollen, and more likely to bleed—often a sign of gingivitis. Over time, persistent inflammation can contribute to more advanced gum disease.
- Cleaning between teeth helps remove plaque and food particles that brushing alone can miss.
- Interdental cleaning supports healthier gum margins and can reduce tartar buildup.
- Daily cleaning is often recommended, even if bleeding or sensitivity occurs—technique adjustments may be needed.
Flossing tips and alternatives when floss is difficult
Some people find flossing challenging due to dexterity issues, arthritis, braces, or simply discomfort. The goal is not to force a single method—it’s to choose an interdental tool that you can use consistently.
When standard floss is difficult, dental professionals often recommend alternatives that match your needs and anatomy. Consistency matters more than perfection with any one tool.
- Options include floss picks, floss holders, threaders, interdental brushes, wooden/plastic picks, and water flossers.
- For arthritis or limited hand strength, a floss holder or pre-threaded tool can reduce strain.
- For spaces that are larger or have gum recession, interdental brushes may clean more comfortably than tight flossing.
If bleeding occurs, it can be a sign of gum inflammation rather than a reason to stop. Gentle technique and a dental visit can help determine the safest, most effective approach.
Signs you’re not cleaning effectively
When interdental cleaning isn’t reaching plaque, gums may show early warning signs. Bleeding during flossing or brushing can be a common indicator of gingivitis.
Other signs include persistent bad breath, gum swelling, or a rough feeling along the gumline. These symptoms don’t always mean severe disease, but they do mean it’s time to refine technique and consider professional guidance.
- Bleeding gums can improve with consistent cleaning, but they should be evaluated if they persist for more than 1–2 weeks.
- Sensitivity or discomfort may indicate the need for a softer tool, gentler motion, or a different interdental option.
- Dental professionals can also check for tartar buildup that home care can’t remove.
Diet Principles of Oral Hygiene: Sugar, Acids, and Nutrients
Limit added sugar and frequent snacking
Diet influences oral health because bacteria use sugars to produce acids. Those acids attack enamel, increasing the risk of cavities—especially when sugary foods or drinks are consumed frequently.
It’s not only about total sugar in a day; frequency matters. Frequent snacking keeps the mouth in a more acidic state for longer periods, which can be harder on enamel.
- Reduce added sugar in drinks like soda, sweet tea, energy drinks, and sweetened coffee.
- Choose fewer “between-meal” sugary snacks, and aim to keep sweet exposures to mealtimes when possible.
- When sweets are unavoidable, pairing them with meals and rinsing with water afterward can help reduce acid exposure.
Balance for enamel and gum health
Enamel and gum tissue benefit from nutrients that support repair and resilience. A balanced diet can help maintain stronger teeth and healthier gums, especially when combined with good brushing and interdental cleaning.
Foods rich in vitamins and minerals—such as fruits and vegetables, lean proteins, and dairy products—provide building blocks for tissue health. Some nutrients also support saliva production and the body’s ability to manage inflammation.
- Include nutrient-rich foods like leafy greens, crunchy vegetables, and dairy or calcium-fortified alternatives.
- Lean proteins support tissue repair, which is important for gum health.
- Limit frequent acidic drinks (like soda or citrus beverages) and consider using a straw for occasional intake.
Hydration and saliva support
Saliva is a natural protective system. It helps wash away food particles, buffers acids, and supports the mouth’s ability to maintain a healthier balance of germs.
Dry mouth can increase cavity risk because there’s less saliva to neutralize acids and less natural cleansing. Dry mouth may be caused by medications, dehydration, mouth breathing, or certain medical conditions.
- Drink water regularly, especially during the day and with meals.
- Consider sugarless gum or lozenges to stimulate saliva (if appropriate for your health needs).
- Avoid tobacco and limit alcohol, both of which can worsen dryness and irritation.
Fluoride, Water, and Preventive Add-Ons
Why fluoride protects teeth
Fluoride is one of the most effective tools for preventing tooth decay. It helps strengthen enamel and makes teeth more resistant to acid attacks from plaque bacteria.
Fluoride toothpaste is a core principle of oral hygiene because it delivers fluoride directly to the tooth surface during brushing. Over time, this can reduce the likelihood of cavities, particularly in people who are at higher risk.
- Fluoride supports enamel repair after early acid damage.
- Using fluoride toothpaste twice daily is typically more protective than relying on occasional rinses.
- Your dentist may recommend additional fluoride products if cavity risk is elevated.
Fluoridated water and community-level protection
Drinking fluoridated tap water can provide ongoing, low-level fluoride exposure that supports cavity prevention. Community water fluoridation is designed to benefit public health broadly.
Not all areas have the same water fluoride content, so it can help to check local information. If fluoridated water isn’t available, your dental professional may suggest other fluoride strategies.
- When available, choosing fluoridated tap water is a simple daily support for enamel protection.
- Check local water reports or ask your dentist about fluoride recommendations for your area.
- Even with fluoridated water, brushing with fluoride toothpaste remains essential.
Professional fluoride treatments for higher-risk patients
Some people are more prone to cavities due to factors like dry mouth, frequent snacking, braces, or a history of recurrent decay. For these patients, dental professionals may recommend in-office fluoride treatments.
Professional fluoride options can include varnish or foam applied during visits. Depending on risk, your dentist may also recommend fluoride gels or rinses for home use.
- Fluoride varnish or foam can provide a concentrated protective layer on teeth.
- Home fluoride gels or rinses may be recommended for specific risk profiles.
- These add-ons work best when combined with daily brushing, interdental cleaning, and diet adjustments.
Dental Check-ups and Cleanings: Treatment That Prevention Requires
How often to see the dentist (and why)
Even with excellent home care, professional exams catch issues that aren’t obvious. Dental check-ups help identify early cavities, gum inflammation, and other concerns before they progress.
Many adults benefit from at least once yearly visits for routine exams and cleanings. People at higher risk—such as those with dry mouth, diabetes, or a history of gum disease—may need more frequent care.
- Exams can detect cavities between teeth, gum changes, and signs of oral cancer.
- Professional monitoring supports better long-term outcomes and fewer emergency visits.
- Dental professionals can also review technique and recommend tools tailored to your mouth.
What professional cleaning removes (tartar/calculus)
Professional cleanings remove tartar (hardened plaque), which can’t be fully removed by brushing and flossing alone. Tartar forms when plaque mineralizes, often near the gumline.
Because tartar can maintain gum irritation, removing it can reduce gingivitis and help prevent progression. Cleanings also help reduce the buildup that makes plaque harder to manage at home.
- Tartar is hardened plaque and often requires specialized instruments to remove safely.
- Removing tartar can improve gum health and reduce bleeding for many patients.
- Cleanings also allow the dental team to check for early signs of decay or gum disease.
Personalized care plans based on risk factors
Oral health needs vary from person to person. A personalized care plan considers risk factors like medication-related dry mouth, diabetes, orthodontic appliances, or previous gum disease.
Dental professionals may adjust visit frequency, recommend specific fluoride products, or suggest targeted interdental tools. The aim is to match prevention strategies to real-world needs.
- Dry mouth from medications can increase cavity risk, so your dentist may recommend additional preventive steps.
- Diabetes can affect gum health, and managing blood sugar may support better oral outcomes.
- Ask about a tailored home-care routine and how often check-ups should occur for your situation.
Lifestyle Principles: Tobacco, Alcohol, and Risk Reduction
Don’t smoke or use tobacco
Tobacco use is one of the most significant lifestyle risk factors for oral health problems. It increases the risk of gum disease and can slow healing after dental procedures.
Smoking and other tobacco products are also associated with a higher risk of oral cancer. Quitting can improve gum health over time and supports better long-term outcomes.
- Quitting resources may include counseling, nicotine replacement options, or prescription supports.
- Even reducing tobacco exposure can be a step forward, but complete cessation is best for oral health.
- Dental professionals can help connect patients with evidence-based quitting support.
Drink less alcohol (and why moderation matters)
Alcohol can contribute to oral health risks, including dry mouth and irritation. Higher alcohol intake has been associated with increased risk of head and neck cancers.
Moderation is the practical approach for most people. If alcohol is part of a routine, reducing frequency and amount can support oral comfort and reduce risk.
- Alcohol’s effects on dryness can make plaque control harder and increase discomfort.
- Moderation helps lower risk without requiring extreme changes that are hard to maintain.
- If there are concerns about alcohol use, discussing options with a clinician can help create a safer plan.
Vaccines and systemic health habits that support oral hygiene
Some preventive health steps can indirectly support oral health. For example, vaccination can reduce the risk of infections that may affect the mouth and throat.
Managing chronic conditions also matters. When the body’s immune response is compromised or inflammation is higher, gum tissues can be more vulnerable.
- HPV vaccination may help prevent certain cancers; ask a healthcare provider whether it’s appropriate.
- Managing conditions like diabetes can support gum health and reduce complications.
- Preventing and treating dry mouth—often by reviewing medications with a clinician—can protect teeth and gums.
Special Situations: Pregnancy, Dry Mouth, Older Adults, and Sports
Pregnancy oral hygiene principles
Pregnancy can change hormone levels, which may increase the risk of gum inflammation and cavities. Many people notice gum bleeding or swelling during pregnancy, especially if plaque control isn’t consistent.
Good oral hygiene during pregnancy is usually the same routine—just with extra attention. Brushing twice daily, flossing daily, and maintaining dental visits can help protect both comfort and oral health.
- Brush twice daily with fluoride toothpaste and clean between teeth once a day.
- Schedule a dental visit before delivery, especially if there is pain, sensitivity, or bleeding.
- If morning nausea affects brushing, your dental professional may suggest strategies to protect enamel.
Dry mouth and medication-related oral hygiene
Dry mouth reduces saliva’s protective effects, which can increase cavity risk and make gums more vulnerable. Some medications—such as certain antihistamines, antidepressants, and decongestants—can contribute to reduced saliva flow.
Practical steps can help: staying hydrated, using sugarless gum, and avoiding tobacco and alcohol. It’s also important to ask a clinician whether medication adjustments are possible.
- Drink water frequently and consider sugarless gum to stimulate saliva.
- Avoid tobacco and limit alcohol to reduce dryness and irritation.
- Ask about saliva-supporting options or medication alternatives if dryness is persistent.
Older adults and people with mobility/dexterity challenges
Oral health challenges can increase with age due to changes in saliva, gum recession, and difficulty brushing or flossing. Vision, cognitive changes, and physical limitations can make daily care harder.
Caregiver support and adaptive tools can make a significant difference. Dental professionals can also recommend supplies designed for easier cleaning.
- For limited dexterity, consider electric toothbrushes, floss holders, or interdental brushes that require less hand strength.
- Caregivers can help with brushing and interdental cleaning when needed, focusing on consistency and comfort.
- Denture wearers should follow denture cleaning principles and remove dentures at night when possible to reduce infection risk.
Mouthguards for injury prevention
Sports and high-risk activities can lead to dental trauma. A mouthguard helps protect teeth and soft tissues from impact injuries.
Injury prevention is an often-overlooked principle of oral hygiene because it reduces the chance of chipped teeth, fractures, and emergency dental visits.
- Use a mouthguard for contact sports or activities with higher risk of falls or collisions.
- Custom or properly fitted mouthguards often provide better protection and comfort.
- Ask your dentist about the best type for your sport and dental needs.
Comparison Table: “Principles” Checklist by Goal (Cavities vs. Gum Disease vs. Fresh Breath)
At-a-glance routine mapping
The principles of oral hygiene work together. Some steps mainly target cavities, others focus on gum health, and several also help reduce plaque-related odor.
| Routine Principle | Primary Benefit | Frequency | Notes / Alternatives |
|---|---|---|---|
| Brush with fluoride toothpaste (about 2 minutes) | Cavities + plaque control | Twice daily | Angle toward gumline; gentle small circles; consider timer/music/app |
| Floss or interdental cleaning | Gum health + plaque/tartar control | Daily | Floss picks, holders/threaders, interdental brushes, water flossers |
| Diet: limit added sugar + frequent snacking | Cavities prevention | Ongoing | Reduce sugary drinks/foods; limit acid frequency; rinse with water after sweets |
| Fluoridated water | Enamel protection | Daily | Choose tap water when available; check local fluoride content |
| Dentist visits + professional cleanings | Early detection + tartar removal | At least yearly | More often if higher risk (dry mouth, diabetes, gum disease history) |
| Avoid tobacco + limit alcohol | Gum health + cancer risk reduction | Ongoing | Quitting support available; moderation for alcohol |
| Mouthguard (sports/high-risk activities) | Injury prevention | As needed | Custom or properly fitted mouthguards provide better protection |
What to do if you’re bleeding or have sensitivity
Bleeding gums and tooth sensitivity can be early signs that plaque control needs refinement or that gum inflammation is present. In many cases, gentle technique and consistent interdental cleaning help, but persistent symptoms should be assessed.
- Call your dentist if bleeding continues for more than 1–2 weeks, if there is swelling, or if pain is present.
- For sensitivity, consider whether brushing pressure is too strong or whether gum recession is exposing root surfaces.
- Adjust home care and schedule an evaluation to check for tartar buildup, cavities, or gum disease progression.
Frequently Asked Questions
What are the five principles of oral hygiene?
The five principles of oral hygiene can be summarized as: brush with fluoride, clean between teeth, eat for oral health (limit sugar/acid and support nutrients), visit the dentist for check-ups and cleanings, and avoid tobacco and limit alcohol. Each principle targets a different part of the problem—plaque, acids, inflammation, or risk factors that make disease more likely.
How long should I brush my teeth each time?
Brush for about 2 minutes per session to give enough time for thorough coverage. Using a timer, a song, or an app can help make the routine consistent and reduce the tendency to rush.
Is flossing necessary if I brush twice a day?
Yes—brushing twice a day is important, but it can’t remove plaque between teeth where toothbrush bristles don’t reach. Daily interdental cleaning helps prevent gingivitis and reduces tartar buildup that can lead to more advanced gum disease.
What if my gums bleed when I floss?
Bleeding during flossing can be a sign of gingivitis, meaning the gums are inflamed from plaque irritation. Gentle technique, consistent daily cleaning, and a dental visit can help address the cause rather than ignoring it.
How often should adults get dental check-ups and cleanings?
Many adults should have dental check-ups and cleanings at least once a year. People with higher risk—such as dry mouth, diabetes, or a history of gum disease—may need more frequent visits based on their dental professional’s recommendations.
Does fluoride toothpaste really prevent cavities?
Fluoride toothpaste helps prevent cavities by strengthening enamel and making teeth more resistant to acid attacks from plaque bacteria. It also supports early enamel repair, which is why fluoride is considered a core principle of oral hygiene.
What’s the best way to handle dry mouth for oral hygiene?
Dry mouth support usually includes hydration, sugarless gum to stimulate saliva, and avoiding tobacco and alcohol. If dryness is medication-related, asking a clinician about alternatives can be an important step.
Can oral hygiene affect overall health?
Oral health can influence overall health because the mouth contains germs and inflammation can spread beyond the gums. Studies suggest possible links between gum disease and conditions like diabetes and respiratory infections, which is why consistent daily care and professional check-ups matter.
Edge Topics (Competitors Don’t Cover Enough): How to Build a Personal Oral Hygiene Plan
Choose tools based on your mouth and barriers (not one-size-fits-all)
Personalizing oral hygiene makes it more likely that the routine will actually be followed. Different mouths need different tools, especially when braces, implants, gum recession, or limited dexterity are involved.
Dental professionals can help match tools to the real barriers that get in the way. The best plan is the one that can be done consistently with good technique.
- Select brush type based on comfort and effectiveness: soft manual brushes or powered brushes for easier plaque removal.
- Choose interdental tools that fit your spaces and comfort level: floss holders/threaders, interdental brushes, or water flossers.
- For arthritis or limited hand strength, adaptive handles and pre-threaded options can reduce friction and improve consistency.
Track progress and plaque control using simple feedback
Sometimes the hardest part of oral hygiene is knowing whether the technique is working. Simple feedback tools can reveal plaque areas and help refine brushing and interdental cleaning.
Disclosing tablets or disclosing toothpaste can show where plaque remains after brushing. This can be especially helpful when gums bleed or when certain tooth areas seem consistently harder to clean.
- Use disclosing products for “spot check” days to identify missed areas.
- Adjust technique for 1–2 weeks, then reassess to see if plaque coverage improves.
- Bring questions to your dental appointment—your dental team can observe technique and recommend targeted changes.
When to seek urgent dental care
Most oral hygiene issues are preventable or manageable, but some symptoms need prompt attention. Waiting too long can allow problems to worsen, especially infections or rapidly progressing gum disease.
Urgent evaluation is especially important when symptoms are severe or persistent. Dental professionals can determine the cause and recommend appropriate treatment quickly.
- Seek prompt care for red flags such as severe pain, swelling, uncontrolled bleeding, or fever.
- Contact a dentist quickly for persistent mouth sores, sudden taste/smell changes, or symptoms that worsen over 24–48 hours.
- Don’t wait for the next routine visit if there are new or alarming changes in the mouth.
If building a personal plan feels overwhelming, our team at Smile Avenue Family Dentistry can help translate the principles of oral hygiene into a routine that fits your lifestyle, your risk factors, and your comfort level. Schedule a consultation to review brushing technique, interdental tool options, and prevention strategies tailored to your needs.