Does A “Dead Tooth” Mean That I Need A Root Canal Treatment?
If you’ve been told your tooth is “dead,” it can feel alarming—and confusing—especially when you hear different treatment options. One of the most common questions patients ask is: does a dead tooth need a root canal? The answer depends on what’s happening inside the tooth, whether infection is present, and whether the tooth can be restored to function long-term.
Quick Answer: Does a Dead Tooth Need a Root Canal?
A “dead tooth” usually means the pulp inside the tooth is no longer vital (not receiving healthy blood supply). In many cases, dental professionals recommend root canal treatment to remove infected or non-vital pulp tissue, disinfect the root canals, and seal the tooth to prevent reinfection.
That said, not every dying tooth automatically requires a root canal. Your dentist’s diagnosis—based on symptoms, exam findings, and X-rays—drives the recommendation.
When the answer is “often yes”
When the pulp becomes necrotic (fully non-vital) and bacteria are present, infection can develop around the root tip. This inflammatory condition is commonly called apical periodontitis, and it can persist even if the tooth stops hurting for a while.
In these situations, a root canal is often recommended because it gives the tooth the best chance to be saved. Root canal therapy removes the dead pulp tissue, cleans and disinfects the canal system, and seals the space so bacteria can’t continue to thrive.
- Root canal is commonly recommended when a tooth is symptomatic (pain, tenderness) and/or when infection is suspected or confirmed.
- It’s also frequently advised when X-rays show signs of bone inflammation near the root tip.
- When the tooth can be restored with a filling and often a crown, root canal treatment can preserve natural tooth structure.
When the answer may be “no”
Sometimes a tooth is “dying” but not fully necrotic. For example, a tooth may have irreversible pulpitis or other changes where the pulp is inflamed but not completely dead, and your dentist may recommend monitoring, a different type of treatment, or a staged approach depending on the findings.
In other cases, the tooth may be too structurally compromised to be predictably restored. Even if root canal treatment could address the pulp issue, the tooth might fracture easily afterward due to extensive decay, cracks, or insufficient remaining tooth structure.
- Not always root canal: early or partial pulp changes may be managed differently, depending on test results.
- Extraction may be more predictable: when the tooth has severe fracture, poor restorability, or a prognosis that is unlikely to support long-term function.
- Your dentist may discuss options such as a crown, onlay, or other restoration plan if the tooth is salvageable.
What to do next (so you don’t delay)
If swelling, pus, severe pain, or a persistent bad taste is present, an urgent dental evaluation is important. These signs can indicate active infection that may worsen if treatment is delayed.
Even when symptoms seem mild, diagnosis matters. A dead tooth can be painless for periods, yet infection can still be developing around the root tip—so the safest next step is a timely exam and imaging.
- Schedule an appointment as soon as possible if a tooth is changing color, hurts when biting, or feels tender to tapping.
- Seek urgent care if there is facial swelling, fever, or trouble swallowing.
- Expect your dentist to explain whether the pulp is truly non-vital and whether infection is present—this determines whether root canal is needed.
What Is a Dead Tooth (Non-Vital Tooth)?
“Dead tooth” is a common phrase patients use, but it helps to translate it into what dental professionals mean clinically. In most cases, it refers to a tooth whose pulp is non-vital, meaning the nerve and blood supply inside the tooth are no longer viable.
Importantly, a non-vital tooth is not automatically beyond saving. Many teeth can be preserved with appropriate endodontic treatment and a strong restoration plan.
Definition of “dead” vs “dying” pulp
A dead tooth typically means the pulp tissue and its blood supply are no longer viable. This condition is called pulp necrosis, and the tooth may be described as depulped or non-vital.
A dying tooth is a broader term that can include stages where the pulp is inflamed and struggling but not yet fully necrotic. The difference matters because treatment recommendations can change depending on whether the pulp is still salvageable or whether it has already died.
- Necrosis (dead pulp): bacteria may invade the canal system and infection can form at the root tip.
- Dying/inflamed pulp: symptoms may be present, but the pulp may not be fully non-vital.
- Dental professionals use tests to determine which stage is most consistent with your symptoms and imaging.
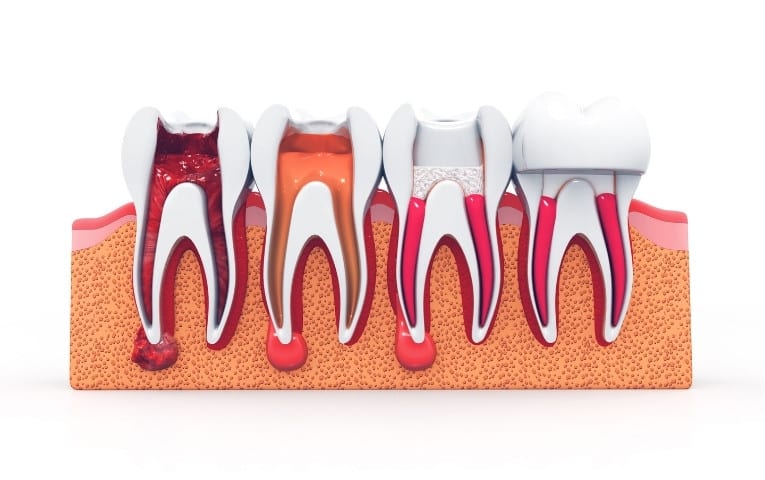
What’s happening inside the tooth
Inside each tooth is a pulp chamber and a network of root canals that contain nerves and blood vessels. When the pulp is healthy, it helps the tooth sense temperature and pain and supports tooth vitality.
When pulp blood flow is compromised—often from deep decay, trauma, or extensive dental work—the pulp can become infected and break down. Over time, the body may respond with inflammation around the root apex, which is where the root canal meets the surrounding bone.
Why “dead tooth” doesn’t always mean extraction
Even if the pulp has died, the tooth’s outer structure may still be strong enough to keep. Root canal therapy is designed to remove the non-vital pulp, disinfect the canal system, and seal it so bacteria cannot re-enter.
After treatment, the tooth often needs a core build-up and frequently a crown to restore strength. When a tooth can be properly restored, saving it can be more conservative than extraction and replacement.
- Many teeth remain restorable with root canal treatment plus a filling or crown.
- When the tooth is too brittle or structurally compromised, extraction may be safer.
- Your dentist weighs both infection control and long-term function when recommending the best option.
Common Causes of Tooth Death
Tooth death usually results from a disruption of the pulp’s blood supply or from bacteria reaching the pulp. While cavities are a common cause, trauma and certain dental procedures can also contribute.
Understanding the cause can help explain symptoms and guide prevention for future teeth.
Tooth decay (cavities reaching the pulp)
Tooth decay begins when bacteria produce acids that weaken enamel and dentin. If cavities are left untreated, they can progress deeper until bacteria reach the pulp chamber.
Once bacteria invade the pulp, inflammation can escalate and eventually the pulp may lose its blood supply. This progression often moves from reversible irritation to irreversible pulpitis, and then to pulp necrosis if the damage is severe.
- Early decay may cause sensitivity, while deeper decay can lead to persistent or spontaneous pain.
- As infection develops, pain may sometimes lessen—yet infection around the root tip may still be present.
- Regular dental visits help catch cavities before they reach the pulp.
Trauma and injuries
Sports injuries, falls, and even minor impacts can damage the blood vessels inside a tooth. Sometimes the tooth looks fine at first, but internal damage can progress over weeks or months.
Cracks and fractures can also expose or injure the pulp. In trauma-related cases, the tooth may develop a pinkish discoloration early on and later shift to grey or darker shades as the pulp deteriorates.
- Any significant dental injury should be evaluated promptly.
- Delayed discoloration can be a clue that pulp damage occurred at the time of injury.
- Early assessment can improve the chances of preserving the tooth.
Large fillings and dental work complications
Extensive restorations can sometimes contribute to pulp problems. Microleakage or micro-caries under a filling may allow bacteria to reach deeper tooth structures over time.
Additionally, the process of placing a large filling can involve heat, pressure, or trauma to the tooth. Temperature changes (hot/cold) and repeated stress on a weakened tooth can also increase the risk of pulp injury.
- Large fillings may require careful monitoring and timely replacement if they fail.
- Symptoms such as lingering sensitivity after dental work should be evaluated.
- Your dentist may recommend a crown if the tooth becomes brittle after treatment.
Dead Tooth Symptoms and Signs to Watch For
Symptoms vary widely. Some non-vital teeth cause obvious discomfort, while others are surprisingly painless until infection becomes more established.
Recognizing patterns—color changes, biting tenderness, swelling, and taste or breath changes—can help you seek care before the problem becomes more complex.
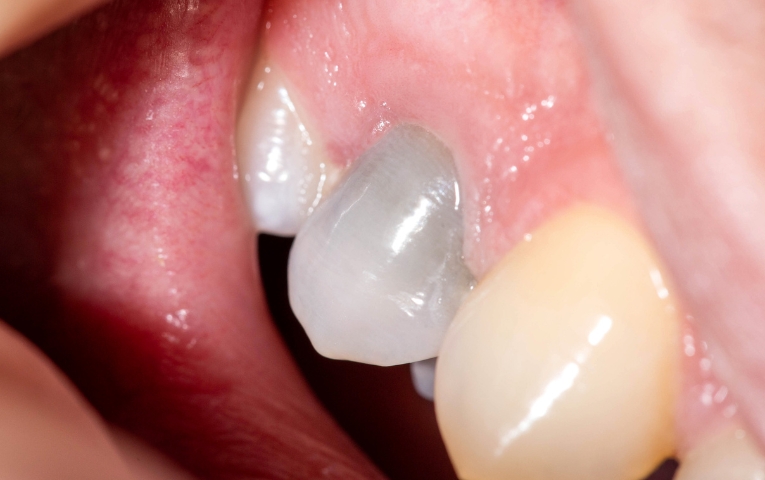
Color changes and appearance
A common sign is a change in tooth color compared with neighboring teeth. Many patients notice a greyish or darker appearance, especially in teeth that have experienced trauma or deep decay.
In trauma-related cases, discoloration may evolve over time. A tooth can shift from a slightly pinkish hue to grey or black as the pulp degenerates.
- Grey/darker tooth: may suggest non-vital pulp.
- Progressive discoloration: can occur over weeks to months after injury.
- Color change alone doesn’t confirm necrosis, but it’s an important clue for evaluation.
Pain, sensitivity, and “why it can stop”
Some dying or dead teeth cause sensitivity to hot or cold. Pain can range from mild discomfort to sharp, lingering pain depending on the stage of pulp inflammation and the presence of infection.
Interestingly, pain may sometimes decrease or disappear. This can happen because the pulp tissue has died and can no longer transmit nerve signals, but infection around the root tip may still be active.
- Sensitivity to temperature: may indicate pulp irritation.
- Intermittent pain: can occur as pressure and inflammation fluctuate.
- No pain: does not necessarily mean the tooth is healthy.
Infection-related signs
When bacteria are involved, infection-related symptoms may appear. Patients often report bad breath or a persistent bad taste, which can be linked to bacterial activity and drainage.
Swelling near the gumline, pus, tenderness to biting, and pain when tapping the tooth are also common signs. In some cases, tooth mobility may be present, though it can be subtle early on.
- Bad taste/bad breath: can be a sign of infection.
- Swelling or gumline pus: suggests active drainage.
- Pain on chewing/percussion: often points toward apical inflammation.
- Mobility: may occur if the supporting bone is affected.
How Dentists Diagnose a Dead Tooth (Not Guesswork)
Diagnosing a non-vital tooth is more than looking at color or asking about symptoms. Dental professionals combine clinical tests with imaging to determine pulp status and whether infection is present.
This is why two patients with “dead tooth” concerns can receive different recommendations.
Clinical tests
Clinical testing helps determine whether the pulp responds to stimuli. A percussion test (gently tapping the tooth) assesses tenderness that may correlate with inflammation around the root tip.
Thermal testing with hot and cold stimuli evaluates nerve response. If the tooth does not respond appropriately compared with adjacent teeth, it may support the diagnosis of non-vital pulp.
- Percussion test: tenderness can suggest apical inflammation.
- Thermal testing: absent or abnormal response may indicate necrosis.
- Additional exam: bite test and gum assessment help refine the diagnosis.
Imaging and advanced diagnostics
X-rays are essential for evaluating the tooth and surrounding bone. They can show signs of bone loss near the root tip, which may indicate apical periodontitis or other infection-related changes.
In complex cases—such as unclear anatomy, persistent symptoms, or suspected hidden lesions—your dentist may recommend CBCT (3D imaging). CBCT can provide more detailed views of root canals and bone involvement.
- 2D X-rays: often sufficient for many cases.
- CBCT/3D scans: may be used when the extent of disease or anatomy is unclear.
- Imaging helps confirm whether symptoms match a non-vital tooth diagnosis.
Interpreting results (what “non-vital” means clinically)
“Non-vital” is a clinical description, not just a feeling. Your dentist interprets test responses, symptom patterns, and radiographic findings together to determine whether the pulp is necrotic, whether inflammation is irreversible, or whether another issue is causing symptoms.
For example, a tooth may be tender to biting without being fully necrotic, or a tooth may be non-vital but not actively infected at the moment. The treatment plan changes based on the full picture.
- Necrotic pulp: often associated with infection risk and apical inflammation.
- Irreversible pulpitis: may require different treatment depending on severity and restorability.
- Radiographs: help distinguish symptoms from infection-related bone changes.
Treatment Options for a Dead Tooth (Root Canal vs Alternatives)
Once a tooth is identified as non-vital, the main decision is whether to treat the tooth from the inside (root canal) or remove it. Your dentist will consider infection control, tooth structure, and your long-term restoration plan.
In many cases, root canal therapy is the most conservative way to preserve a natural tooth.
Root canal therapy (endodontic treatment) — when it’s recommended
Root canal therapy is designed to address the source of infection and stop inflammation from progressing. The process removes dead pulp tissue, cleans and disinfects the root canal system, and seals it to prevent bacteria from re-entering.
After the canals are sealed, the tooth typically needs a restoration to protect it. Many treated teeth become more brittle over time, so a core build-up and often a crown are recommended for strength, especially for molars.
- Goal: eliminate infection and prevent reinfection.
- Typical outcome: reduced pain and healing of apical inflammation.
- Restoration plan: filling or crown based on how much tooth structure remains.
Extraction and replacement options
Extraction may be recommended when a tooth cannot be predictably restored. This can happen if the tooth is fractured below the gumline, has extensive structural loss, or has a poor prognosis due to repeated failure of restorations.
When extraction is chosen, replacement options may include dental implants, bridges, or dentures. Your dentist can discuss timing and the best pathway based on bone health, adjacent teeth, and your bite.
- Implants: often provide a long-term replacement option.
- Bridges: can restore function when implant placement isn’t ideal.
- Dentures: may be considered depending on overall dental needs.
Potential complications and risks (set expectations)
Root canal treatment is highly standardized, but no procedure is risk-free. Potential issues include persistent infection if bacteria remain in complex canal anatomy, or reinfection if the tooth is not sealed properly afterward.
Some teeth require retreatment if symptoms persist or if the initial seal fails. Complex cases may also need additional procedures, such as surgical endodontics, depending on the location and extent of infection.
- Persistent infection: can occur if disinfection is incomplete or anatomy is complex.
- Reinfection risk: increases if the final restoration leaks or breaks down.
- Follow-up matters: healing is monitored with symptoms and repeat imaging when needed.
Does a Dead Tooth Need a Root Canal? Decision Factors That Matter
Whether root canal treatment is recommended depends on multiple factors, not just the label “dead tooth.” Your dentist’s goal is to control infection, preserve function, and choose the most predictable long-term option.
These decision factors help explain why two patients with similar symptoms may receive different plans.
Tooth structure and restorability
A key question is whether the tooth can be restored after treatment. If the tooth is mostly intact, root canal therapy plus a filling or crown can often preserve it for years.
If the tooth has extensive decay, large portions missing, or a crack that compromises the remaining structure, the prognosis may be poor. In those cases, extraction can be more predictable than trying to rebuild a tooth that may fracture.
- Mostly intact tooth: often better candidate for root canal and crown.
- Severely compromised tooth: may not be restorable even if the canals can be treated.
- Restoration strength: helps prevent future fracture and leakage.
Presence and severity of infection
Symptoms and imaging help determine whether infection is active. Signs such as swelling, pus, and pain on biting can suggest apical infection, which typically increases the urgency for endodontic treatment.
Your dentist may also evaluate whether there is bone involvement around the root tip. When apical periodontitis is present, root canal therapy is often recommended to remove the source and allow healing.
- Swelling/abscess indicators: push toward prompt root canal or urgent drainage.
- Radiographic bone changes: support the need for endodontic treatment.
- Reversible conditions: may be managed differently if the pulp isn’t fully necrotic.
Symptoms, timeline, and overall prognosis
Waiting can change the course of disease. Untreated necrosis can allow bacteria to multiply and inflammation to expand, potentially increasing the complexity of treatment and the risk of abscess formation.
Early treatment often makes recovery easier and can improve the chances of successful healing. Your dentist will also consider your overall oral health and how well the tooth can be protected afterward.
- Why waiting can worsen outcomes: infection may spread to surrounding tissues and bone.
- Early intervention: often reduces the likelihood of severe flare-ups.
- Prognosis depends on: structure, infection extent, and restoration quality.
What Happens If You Leave a Dead Tooth Untreated?
Choosing to delay treatment can have consequences. Even when a dead tooth seems stable, bacteria and inflammation around the root tip can continue progressing.
Understanding what can happen helps clarify why timely evaluation is strongly recommended.
Infection progression
Necrotic pulp tissue can act as a reservoir for bacteria. Over time, this can lead to persistent inflammation at the root apex, known as apical periodontitis.
In some cases, the infection can form an abscess—a collection of pus that may cause throbbing pain and significant swelling. Studies and clinical experience consistently show that infections rarely “self-resolve” reliably when the source remains inside the tooth.
- Apical inflammation: can persist and gradually worsen.
- Abscess risk: increases as infection advances.
- Pain may fluctuate: but disease can still be active.
Spread beyond the tooth
Infection can extend from the root tip into surrounding gums and jawbone. This can contribute to bone loss and may affect nearby teeth depending on the location and severity.
Once infection spreads, treatment may require more complex approaches, and recovery may take longer. In rare cases, severe infections can become urgent medical concerns.
- Jawbone involvement: can complicate healing.
- Adjacent tooth risk: may increase if infection spreads.
- Longer course: untreated problems often become harder to manage.
When it becomes an emergency
Some symptoms should not wait for a routine appointment. Facial swelling, fever, rapidly worsening pain, and difficulty swallowing or breathing are red flags.
If these occur, urgent dental care or emergency evaluation is necessary. Infections can escalate quickly, and prompt treatment can reduce the risk of complications.
- Emergency signs: swelling spreading to the face/neck, fever, severe weakness.
- Urgency: difficulty swallowing/breathing requires immediate care.
- Action: contact urgent dental services or emergency medical care right away.
Root Canal Process (What Patients Can Expect)
Knowing what happens during root canal treatment can reduce anxiety. While each case differs, the general steps are designed to disinfect the canals and seal them effectively.
Your dentist will tailor the plan based on tooth anatomy, infection status, and how much restoration is needed afterward.
Step-by-step overview
Diagnosis comes first, using an exam and imaging such as X-rays or CBCT when needed. If infection is present, your dentist may plan for drainage and may discuss whether antibiotics are appropriate in specific circumstances.
During the procedure, local anesthetic is used, and a rubber dam may be placed to keep the area clean. The dentist accesses the pulp chamber, removes infected or non-vital tissue, cleans and disinfects the canals with specialized instruments, and irrigates to reduce bacterial load.
- Access opening: creates entry to the pulp chamber.
- Cleaning/disinfection: removes debris and disinfects canal walls.
- Drainage: may be performed if pus is present.
- Obturation/sealing: canals are filled with biocompatible material (often gutta-percha) and sealed.
Restoring the tooth after treatment
Root canal therapy treats the inside of the tooth, but the outside still needs protection. After the canals are sealed, the tooth is typically restored with a core build-up and then a crown or strong filling.
A crown is often recommended because a treated tooth can become more brittle, especially if it already has a large filling or has lost significant structure. A well-sealed, well-supported restoration helps prevent leakage and reinfection.
- Core build-up: replaces lost tooth structure and supports the final restoration.
- Crown: helps protect against chewing forces and fracture risk.
- Timing: your dentist may recommend completing the restoration promptly after endodontic therapy.
Pain relief and recovery expectations
Many patients experience relief after treatment because the source of infection and pressure is addressed. If swelling or infection was present, improvement can occur over days, though complete healing may take longer.
Follow-up visits help confirm healing. Your dentist may schedule a re-evaluation and, in some cases, repeat imaging to ensure the bone around the root tip is recovering.
- Symptom improvement: often begins within 24–72 hours for many patients.
- Healing timeline: can take weeks to months depending on the extent of infection.
- Follow-up: ensures the tooth is sealed and healing as expected.
Prevention: How to Reduce the Risk of a Dead Tooth
While some causes (like trauma) can’t always be prevented, many tooth deaths are preventable through early care and protective habits. Prevention focuses on stopping decay early, protecting teeth from impact, and monitoring restorations.
These steps can reduce the likelihood of pulp damage and the need for endodontic treatment.
Cavity prevention and early treatment
Regular dental checkups allow cavities to be detected before they reach the pulp. Fluoride, consistent brushing, and flossing help reduce bacterial load and strengthen enamel.
Diet also matters. Frequent sugar exposure can keep the mouth acidic, speeding up decay progression even in people who brush and floss.
- Brush twice daily with fluoride toothpaste and clean between teeth daily.
- Limit sugary snacks and drinks, especially between meals.
- Address cavities early—small fillings are far easier to prevent from reaching the pulp.
Protect teeth from trauma
Sports and high-impact activities increase the risk of dental injuries. Mouthguards can significantly reduce the chance of fractures and pulp damage during impacts.
Also, habits like grinding or chewing hard objects can contribute to cracks. If a tooth is injured, prompt evaluation is important even if pain seems minimal.
- Wear a mouthguard for sports and activities with impact risk.
- Avoid using teeth to open packages or bite hard items.
- Get dental assessment after trauma, especially if discoloration appears later.
Monitor large fillings and restorations
Large fillings can fail over time due to wear, microleakage, or recurrent decay. When restorations break down, bacteria can seep deeper and threaten the pulp.
Monitoring and timely replacement of failing restorations can prevent progression to pulp necrosis. If a tooth becomes sensitive after a filling, it should be evaluated rather than ignored.
- Watch for recurrent sensitivity or changes around old fillings.
- Replace or repair failing restorations early to prevent micro-caries.
- Ask your dentist whether a crown is recommended to protect a weakened tooth.
Frequently Asked Questions
Can a dead tooth be saved without a root canal?
Sometimes, depending on whether the pulp is truly necrotic and whether the tooth can be treated and restored successfully. If the pulp is fully dead and infection is present, root canal treatment is often the most reliable way to eliminate the source. Your dentist can confirm pulp status and infection risk with tests and imaging.
Does a dead tooth always hurt?
No. Some non-vital teeth cause little to no pain, especially early on or when the nerve is no longer transmitting signals. Pain can appear later due to apical inflammation or abscess formation, so lack of pain does not always mean the tooth is healthy.
Why would my tooth hurt if the nerve is dead?
Even when the nerve inside the tooth is non-vital, infection and inflammation can develop around the root tip. This can irritate the periodontal ligament and surrounding tissues, leading to pain with biting or tapping. In dentistry, this is often associated with apical periodontitis.
Can a dead tooth cause bad breath or bad taste?
Yes. Bacteria associated with necrotic pulp and infection can produce odors and tastes that linger. Bad breath or a persistent bad taste, especially when paired with other symptoms like swelling or discoloration, should be evaluated.
How long can I wait before getting a root canal for a dead tooth?
It’s best not to delay once a non-vital tooth and infection risk are suspected. Untreated necrosis can progress to abscess and spread, making treatment more complex. A prompt dental evaluation is recommended so the diagnosis can guide the safest timeline.
Will I need a crown after a root canal on a dead tooth?
Often, yes. Many root canal–treated teeth become more brittle, and a crown helps protect the tooth from chewing forces and fracture. Whether a crown is necessary depends on how much tooth structure remains and the tooth’s location in the mouth.
What are the signs of a dental abscess from a dead tooth?
Common signs include swelling, pus drainage, throbbing pain, and tenderness to bite or percussion. Some people also experience fever or feel generally unwell. If these symptoms occur, urgent dental evaluation is important.
Is a root canal safe and how successful is it?
Root canal treatment is a standard, conservative procedure used for decades. Success depends on accurate diagnosis, thorough cleaning and disinfection, proper sealing, and a durable restoration afterward. Your dentist can discuss expected outcomes based on your specific tooth and imaging findings.
Dead Tooth vs Root Canal: Quick Comparison Table (Decision Support)
The table below summarizes how dentists often weigh root canal therapy versus extraction when a tooth is non-vital. It’s not a substitute for diagnosis, but it can help you understand the decision factors.
Root canal vs extraction at a glance
| Option | When chosen | Goal | Pros | Cons/risks | Typical next step |
|---|---|---|---|---|---|
| Root canal therapy | Tooth is non-vital and restorable; infection/inflammation at root tip is present or likely | Remove dead pulp, disinfect canals, seal to stop reinfection | Preserves natural tooth; conservative vs extraction | May require retreatment; depends on sealing and restoration quality | Crown (often) or strong filling/core build-up |
| Extraction | Tooth is too damaged (fracture, insufficient structure, poor prognosis) | Remove source of infection and non-restorable tooth | Predictable when tooth cannot be saved; eliminates endodontic failure risk | Requires replacement planning; may involve bone preservation depending on case | Implant, bridge, or denture |
Symptom/infection indicators that push toward root canal
Certain signs more strongly suggest non-vital pulp with apical infection risk. When these are present, dental professionals typically recommend endodontic evaluation to determine whether root canal therapy is needed.
Below are common indicators and how they often relate to treatment planning.
- Grey discoloration → may indicate non-vital pulp; often prompts pulp testing and X-ray evaluation.
- Sensitivity to hot/cold → may indicate pulp irritation; persistent or worsening symptoms can suggest irreversible damage.
- Bad taste/bad breath → may indicate bacterial activity associated with necrosis/infection.
- Swelling or gumline pus → suggests active infection; often increases urgency for treatment.
- Pain on chewing/percussion → can indicate apical inflammation consistent with apical periodontitis.
Prognosis factors that change the recommendation
Even when a tooth is non-vital, the recommendation depends on how well it can be treated and restored. Dentists consider tooth structure, radiographic findings, and whether infection has caused significant bone involvement.
These prognosis factors help determine whether root canal therapy is likely to succeed or whether extraction is the safer long-term choice.
- Tooth structure: remaining enamel/dentin and whether a crown can be placed for protection.
- Radiographic bone involvement: size and location of lesions near the root tip.
- Presence of abscess: may require urgent intervention and can affect complexity.
- Restoration feasibility: ability to seal the tooth after endodontic therapy to prevent reinfection.
If you suspect a tooth is “dead” or you’re wondering does a dead tooth need a root canal, scheduling a consultation is the safest next step. A dental professional can perform pulp testing, check for infection with imaging, and recommend the most predictable option for saving your tooth—or choosing extraction when it’s truly the better path. Contact our team at Smile Avenue Family Dentistry to book an evaluation and get clear answers based on your specific findings.