Can Tooth Pain Nerve Be Permanently Killed in a Short Time?
If you’re searching for a way to kill tooth pain nerve in 3 seconds permanently, it’s usually because the pain feels unbearable and time feels irrelevant. Unfortunately, the “instant permanent cure” idea is not real—and relying on it can delay the treatment needed to stop the underlying cause. The good news: fast, safe symptom relief is possible while a dentist provides definitive care.
The Truth: Can You “Kill Tooth Pain Nerve in 3 Seconds Permanently”?
Why the “3 seconds” claim is a myth
Tooth nerves sit deep inside the tooth in the pulp chamber, protected by layers of enamel and dentin. At home, it isn’t possible to reach that space or permanently destroy the nerve instantly—especially not in “3 seconds.” Dental professionals can access the pulp only after removing decay, opening the tooth, and using sterile techniques.
Most “instant cures” online work by numbing the area temporarily or masking pain signals. That can feel like the nerve is “dead,” but the infection, inflammation, or crack that triggered the pain may still be progressing underneath. In many cases, pain returns worse once the temporary numbness wears off.
Even if a nerve becomes less responsive over time, that does not mean the problem is solved. Studies and clinical experience consistently show that dental infections can continue silently, sometimes leading to abscess formation and bone involvement.
What “permanent relief” actually means for tooth nerve pain
In dentistry, “permanent relief” usually means the source of pain is removed and the tooth is sealed or restored so bacteria can’t keep irritating the pulp. For example, if the pain comes from deep decay or an infected pulp, treatment focuses on eliminating the diseased tissue and preventing reinfection.
It’s also important to understand that pain can temporarily stop even while the underlying condition worsens. When inflammation decreases or the nerve’s ability to transmit signals changes, pain may lessen. However, the infection process can still continue, which is why a dental exam and imaging matter.
Your dentist may describe “lasting relief” as pain that does not return after definitive treatment such as a root canal, a restoration (filling/crown), or—when necessary—extraction. The goal is not just symptom control; it’s stopping the cause.
What to do right now when you’re searching this exact phrase
If the search phrase is happening because the toothache is urgent, the safest next step is to arrange prompt dental evaluation. Many dental offices can offer same-day or next-day appointments for severe pain, and imaging can quickly identify whether the issue is pulp inflammation, a crack, or an abscess.
While waiting, interim care can reduce discomfort without damaging tissues. Cold compresses, gentle rinses, and appropriate over-the-counter pain relievers can help you get through the day or night—without attempting dangerous “nerve killing” hacks.
Set expectations clearly: fast relief is realistic, but an instant permanent cure at home is not. When pain is severe, delaying definitive treatment can increase the chance of needing more extensive care later.
What Tooth Nerve Pain Really Is (Pulp, Nerves, and Pain Signals)
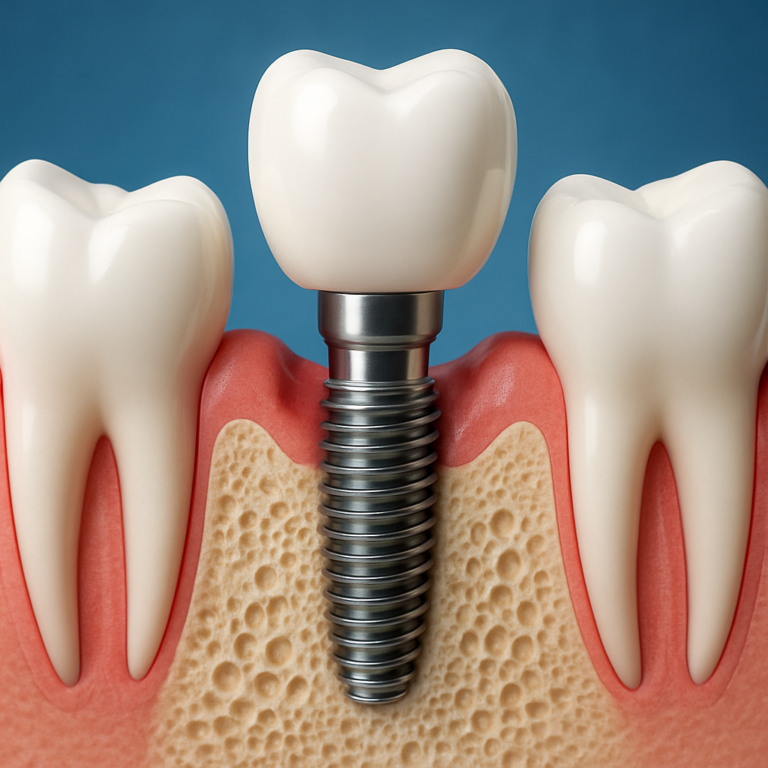
Anatomy basics: what’s inside the tooth pulp
The center of a tooth contains pulp, a soft tissue that houses nerves and blood vessels. The pulp helps the tooth sense pressure and temperature and supports the tooth’s internal health. When the pulp becomes irritated, the nerves send pain signals that can feel sharp, throbbing, or “electric.”
Because the pulp sits in a confined space, inflammation can create pressure inside the tooth. That pressure can intensify pain, especially when biting or when temperature changes trigger fluid movement within the tooth.
In most cases, tooth nerve pain is not just “the nerve itself hurting”—it’s the body’s response to irritation and inflammation inside the pulp chamber. That’s why the most effective treatment targets the underlying cause.
How irritation becomes sharp/throbbing pain
When bacteria invade through decay, cracks, or leaking restorations, they can inflame the pulp. Inflammation increases sensitivity, so even minor stimuli—like cold air or sweet foods—may trigger a painful response.
As inflammation worsens, pain often changes character. Some people experience brief, sharp jolts; others feel constant throbbing that can worsen at night. Both patterns can indicate pulp involvement, but the cause and severity may differ.
Dental professionals often describe tooth pain as a “signal” that something inside the tooth needs attention. The intensity of pain does not always match the exact severity of infection, which is another reason imaging and an exam are important.
Why pain patterns can mislead you
Pain can fluctuate because inflammation can temporarily rise and fall. A tooth may feel better for a few hours or even a couple of days, especially after pain medication. That improvement can be misleading if the underlying infection continues.
Some people assume that “if it stopped hurting, it must be healed.” In reality, reduced pain can occur when the nerve’s ability to transmit signals changes, or when swelling temporarily decreases. Unfortunately, infection can still spread beyond the pulp into the tissues around the root.
Because pain patterns can be confusing, dentists rely on clinical tests and X-rays to determine whether the pulp is reversibly inflamed, irreversibly inflamed, or infected. This is also why follow-up care matters even after pain improves.
Causes of Tooth Nerve Pain (What Triggers the Pulp)
Deep cavities and untreated decay
Deep cavities can progress from the outer enamel into deeper dentin and eventually reach the pulp. As the cavity gets closer to the nerve, bacteria and their byproducts can irritate the pulp and trigger pain.
Decay is often gradual, but once it reaches the pulp, symptoms can become sudden and severe. In many cases, untreated decay leads to irreversible pulpitis (pulp inflammation that cannot heal on its own) and may progress to infection.
Because decay can be hidden under old fillings or between teeth, regular checkups and bitewing X-rays are important for catching problems before they reach the nerve.
Cracks, broken teeth, and dental trauma
Cracks can be tiny—sometimes invisible to the naked eye—but still allow bacteria to enter or irritate the pulp. Micro-cracks may cause sharp pain when biting, especially if the crack allows movement of the tooth structure.
Trauma from sports, falls, or accidents can also injure the pulp even if the tooth looks mostly intact. Over time, the pulp may become inflamed and pain can appear days, weeks, or even months later.
Grinding and clenching can worsen these issues by increasing pressure on already weakened teeth. If a crack is present, your dentist may recommend stabilization with a filling, crown, or other protective restoration.
Infection and gum-related causes
Not all tooth nerve pain starts with a cavity. Gum disease, abscesses, and exposed root surfaces from recession can expose sensitive areas and inflame tissues near the root. In some cases, infection spreads from the gums toward the tooth’s internal structures.
Failed restorations—such as old fillings or crowns with leaks—can allow bacteria to seep underneath. This can irritate the pulp and lead to persistent pain that may worsen with chewing or temperature changes.
When infection forms, it may create pressure and swelling. If swelling occurs, urgent evaluation is often needed to prevent spread to surrounding tissues.
Symptoms That Suggest Nerve Inflammation or Infection
Sensitivity clues (hot/cold/sweet/air)
Tooth sensitivity can be a sign of pulp irritation, especially when it is intense or lingering. Cold sensitivity that causes sharp pain may indicate pulp involvement, while sweet sensitivity can suggest exposed dentin or deeper irritation.
Air sensitivity—pain when breathing in cold air—often points to exposed dentin or gum recession. However, if sensitivity escalates into lingering throbbing, it may be more than simple enamel wear.
Some people also notice pain with biting or pressure, which can indicate inflammation deeper in the tooth. Your dentist can differentiate between surface sensitivity and pulpitis using tests and imaging.
Pain behavior clues (sharp jolt vs constant throbbing)
Sharp, sudden pain—sometimes described as a “jolt”—can occur when a crack or deep cavity irritates the pulp during biting. This type of pain may come and go, often triggered by chewing or temperature changes.
Constant throbbing pain that persists for hours is more suggestive of significant pulp inflammation or infection. Night pain is also common because lying down can increase blood flow and pressure in inflamed tissues.
Intermittent pain does not necessarily mean the problem is minor. Because pain can fluctuate, the safest approach is to treat persistent symptoms as a reason for dental evaluation.
Red-flag symptoms that may indicate emergency
Some symptoms suggest infection may be spreading or causing systemic involvement. Facial swelling, fever, and feeling generally unwell are red flags that warrant urgent care.
Other urgent signs include difficulty swallowing, trouble breathing, swelling under the jaw, or pain that rapidly worsens over hours. These can indicate that infection is moving beyond the tooth.
If any red flags are present, do not wait for a “3-second” fix to work. Contact emergency dental services or urgent medical care immediately.
Can You Kill Tooth Nerve Pain at Home in Seconds? (Safe vs Dangerous)
What home remedies can and can’t do
Home care can help reduce discomfort, but it cannot remove infected pulp or reverse irreversible pulpitis. Temporary methods may numb the area, reduce inflammation, or keep the mouth clean, which can make pain more manageable until a dentist can treat the source.
For example, cold compresses can reduce swelling and numb the cheek area. Saltwater rinses can gently cleanse the area and may reduce irritation in the gums. Over-the-counter pain relievers can reduce inflammation and pain signaling.
These approaches are symptom management. They do not “kill the nerve” in a permanent way, and they do not eliminate bacteria inside the tooth.
Common “viral” methods to avoid
Some viral methods are dangerous because they can burn soft tissues, worsen damage, or increase infection risk. Avoid using bleach, alcohol, or other harsh chemicals directly on the tooth or gums.
Also avoid placing sharp objects against the tooth, attempting to “drill” or puncture the area, or using super glue/wax to seal over pain. These can trap bacteria, cause burns, and delay proper care.
Crushing pills directly on the tooth can also irritate tissues and create chemical burns. If medication is needed, it should be taken as directed on the label or prescribed by a clinician.
Why DIY attempts can backfire
DIY attempts can cause tissue damage because the pulp and surrounding tissues are delicate. Burns to the gums or inner tissues can add new pain and complicate treatment.
Masking symptoms can also delay diagnosis. If pain improves after a risky home method, it may create a false sense of security while infection continues deeper into the tooth or surrounding bone.
In severe cases, untreated infection can lead to abscess formation and bone loss. That can increase the likelihood of needing a root canal, surgery, or extraction later.
Fast, Safe Temporary Relief While You Wait for a Dentist
Cold compress and swelling control
A cold compress can help reduce pain and swelling by numbing the area and limiting inflammation. Apply it to the cheek on the affected side for about 10–15 minutes at a time, then rest for at least 10 minutes before repeating.
Cold therapy is most helpful when pain is accompanied by swelling or when the tooth feels very sensitive to temperature. It is not a cure, but it can make the next few hours more tolerable.
Do not apply ice directly to the skin. Wrap it in a cloth to prevent frostbite or skin irritation.
Saltwater rinse and gentle cleaning
Warm saltwater rinses can soothe irritated tissues and help keep the area clean. Mix about 1/2 teaspoon of salt in 8 ounces (240 mL) of warm water, then gently swish for 30 seconds and spit. Repeat 2–4 times per day.
Saltwater may reduce inflammation and help remove debris around the tooth and gums. It can be especially useful if food is trapped near the painful area.
Do not rinse aggressively or use very hot water, which can worsen irritation. Gentle rinsing is enough.
Clove oil and OTC pain relievers (what’s reasonable)
Clove oil contains eugenol, which can provide short-term numbing and comfort. If used, apply a very small amount to a cotton swab and dab it carefully on the painful area—avoid soaking the gums or using large quantities.
Over-the-counter pain relievers often provide more reliable relief. Many adults can use ibuprofen or acetaminophen according to label directions, unless contraindicated due to medical conditions, allergies, or medication interactions.
If you have kidney disease, stomach ulcers, are on blood thinners, are pregnant, or have other health concerns, ask a pharmacist or clinician before taking NSAIDs like ibuprofen. Pain control should be safe, not experimental.
Home Remedies Mentioned Online (What to Use Carefully, What to Skip)
Clove oil, garlic paste, peppermint tea bag, vanilla extract (temporary comfort)
Many online remedies are popular because they may temporarily reduce discomfort. Clove oil can numb due to eugenol, while garlic paste, peppermint tea bag, and vanilla extract may provide mild soothing effects for some people.
However, none of these approaches can remove infected pulp or “kill tooth pain nerve in 3 seconds permanently.” They are comfort measures at best, and they should not replace dental treatment.
If any remedy causes burning, increased redness, or worsening pain, stop immediately and rinse with water. Irritation from DIY substances can make the situation harder to treat.
Hydrogen peroxide rinses and other antiseptic claims
Hydrogen peroxide is sometimes suggested as an antiseptic rinse. While diluted peroxide may reduce bacteria in the mouth, it is not a cure for pulp infection and does not reach the pulp chamber where the nerve pain originates.
Overuse or incorrect dilution can irritate tissues and delay healing. If peroxide is used at all, it should be diluted and used briefly, following product instructions or clinician guidance.
For most people, saltwater rinses are a safer first option for temporary comfort. If peroxide is used, it should be occasional—not a substitute for definitive dental care.
“Hydrogen peroxide/garlic/other hacks” vs evidence-based care
Symptom management is not the same as definitive treatment. Evidence-based dental care focuses on removing the source of irritation—such as infected pulp, decay, or a crack—and then sealing or restoring the tooth.
Online “hacks” can sometimes reduce pain for minutes to hours, but they do not eliminate bacteria inside the tooth. That means the underlying problem can continue, leading to worsening symptoms or complications.
When tooth pain is severe, persistent, or associated with swelling, the safest path is prompt dental diagnosis. Your dentist can determine whether the tooth needs a root canal, a restoration, gum treatment, or—rarely—extraction.
How Long Until a Tooth Nerve “Dies”? (Timeline and Misconceptions)
Typical timelines by cause severity
There is no single timeline for when a tooth nerve “dies,” because it depends on the cause, depth of damage, and whether infection is present. Some cases of mild inflammation may improve within days if the source is removed early.
More severe decay or trauma can lead to irreversible pulpitis that does not heal on its own. In those cases, pain may persist or fluctuate over weeks, and infection may develop even if symptoms temporarily lessen.
Clinically, people sometimes report that pain changes after a few days, but “less pain” does not mean the nerve is permanently solved. The infection process can continue, and imaging is often needed to confirm what is happening.
Why pain may lessen as the nerve deteriorates
As pulp tissue becomes more damaged, the nerve’s ability to transmit pain signals can decrease. That can make the tooth feel better temporarily, leading some people to believe the problem has resolved.
However, reduced pain can coincide with worsening infection. A tooth may be less painful while bacteria spread toward the root tip, potentially forming an abscess.
This is why dental professionals emphasize evaluation even when pain improves. The goal is to treat the cause, not just the symptom.
The danger of waiting for “it to stop”
Waiting for pain to stop can be risky because infection can progress without obvious symptoms. Abscesses can develop and expand, sometimes causing swelling, drainage, or systemic symptoms.
Infection can also contribute to bone loss around the tooth root. Once bone involvement occurs, treatment may become more complex and recovery time can increase.
If the toothache is persistent, worsening, or associated with swelling or fever, delaying care is not recommended. Prompt treatment reduces the chance of complications and improves the likelihood of saving the tooth.
Professional Treatments That Permanently Stop Tooth Nerve Pain
Root canal therapy (the main “permanent relief” procedure)
Root canal therapy is often the definitive treatment for irreversible pulpitis or infected pulp. The procedure removes the inflamed or infected pulp tissue, cleans and disinfects the inside of the tooth, and then seals it to prevent reinfection.
Once the source of irritation is removed and the tooth is sealed, pain typically improves significantly. Many patients feel relief within 24–72 hours, though some soreness can occur for a few days after treatment.
Your dentist may recommend a crown afterward, especially for molars, to protect the tooth structure and reduce the risk of fracture. Root canal therapy aims for long-term function, not just short-term numbness.
Fillings, crowns, and restorative protection
If the pain is caused by decay that has not fully progressed to the pulp, a filling may be enough to remove the damaged tissue and restore the tooth. When cracks or structural weakness are involved, a crown may be recommended to protect the tooth.
Restorations can also address leaking margins from older fillings or crowns. By sealing gaps, dentists reduce bacterial entry and stop ongoing irritation that can trigger nerve pain.
In many cases, the right restoration prevents future nerve flare-ups by removing the pathways bacteria use to reach deeper layers.
Extraction and when it’s the right option
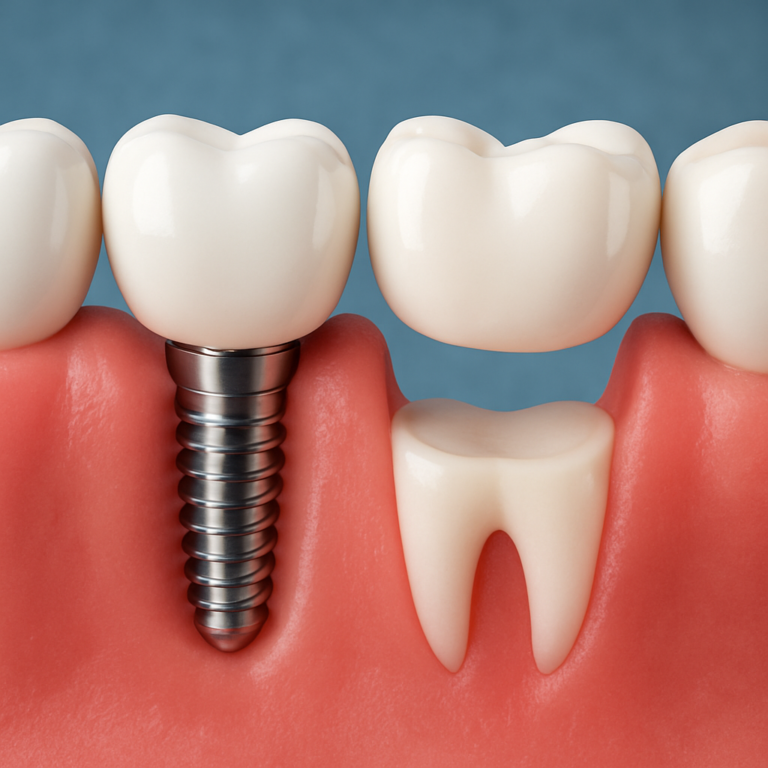
Extraction may be the best option when a tooth is too damaged to restore safely. This can occur with extensive decay, severe cracks, or when the tooth cannot be stabilized after infection.
Even when extraction is recommended, the goal is to eliminate the source of infection and pain. Your dentist may discuss replacement options such as implants or bridges depending on the situation.
While extraction can be emotionally difficult, it can prevent ongoing infection and reduce the risk of complications when the tooth cannot be saved.
When Antibiotics Are Needed (and When They Aren’t)
Infection vs inflammation: what antibiotics treat
Antibiotics treat bacterial infections, but they do not remove the source of infection inside a tooth. For tooth nerve pain, definitive care typically involves removing infected pulp, draining an abscess if present, and sealing the tooth.
In many dental cases, antibiotics are not required if the infection is localized and can be treated with dental procedures. Dental professionals often reserve antibiotics for situations where infection is spreading or systemic symptoms are present.
Your dentist may still prescribe antibiotics in select cases, but they are usually an adjunct—not the main solution.
Signs that suggest bacterial spread
Antibiotics may be more urgent when infection appears to be spreading beyond the tooth. Signs can include facial swelling, fever, chills, swollen lymph nodes, or feeling weak and unwell.
Difficulty swallowing, trouble breathing, or rapidly increasing swelling are emergency-level symptoms. In these situations, prompt medical or emergency dental care is essential.
Because systemic spread can become dangerous quickly, do not rely on home remedies to “wait out” these symptoms.
Why definitive dental treatment still matters
Even if antibiotics reduce symptoms, they may not fully eliminate the infection source inside the tooth. Without removing infected tissue and sealing the tooth, bacteria can persist and symptoms can return.
Definitive treatment addresses the root cause—decay, crack, infected pulp, or a failing restoration. This is what provides the most reliable long-term relief.
Antibiotics can help the body manage spread, but they cannot replace procedures like root canal therapy, drainage, restoration, or extraction when indicated.
Prevention: How to Avoid Future Tooth Nerve Pain
Daily habits that reduce decay and nerve irritation
Preventing decay is one of the best ways to avoid pulp inflammation. Brush at least twice daily with fluoride toothpaste, using gentle technique along the gumline and tooth surfaces.
Floss daily or use interdental brushes to remove plaque between teeth where cavities often start. Plaque buildup can lead to enamel breakdown and eventually deeper decay.
Regular dental cleanings and fluoride treatments can further reduce risk, especially for people with a history of cavities.
Protect teeth from trauma and grinding
Grinding and clenching can overload teeth and contribute to cracks. If morning jaw soreness or worn tooth surfaces are present, a dentist may recommend a night guard.
Sports injuries can also damage teeth. Using a properly fitted mouthguard during contact sports can reduce the risk of trauma to the pulp.
Protective habits don’t just prevent pain—they help preserve tooth structure so nerves are less likely to become exposed or inflamed.
Catch problems early with exams and imaging
Many dental problems start silently. Routine exams and digital X-rays can detect hidden decay, cracks, or failing restorations before they reach the pulp.
For people with higher cavity risk, dentists may recommend more frequent checkups. Early intervention often means simpler treatment like a filling rather than root canal therapy.
Imaging also helps explain symptoms that seem confusing—like pain that comes and goes—by showing what’s happening inside the tooth.
Comparison Table: “3-Second Nerve Killing” vs Real Dental Care
Side-by-side comparison of outcomes and risks
| Claim/Method | What it actually does | Duration of relief | Can it remove infection/decay? | Main risks |
|---|---|---|---|---|
| “Kill tooth pain nerve in 3 seconds permanently” at home | Numbs or masks symptoms; cannot access pulp chamber | Minutes to hours (if any) | No | Delayed treatment, worsening infection, tissue damage |
| Cold compress | Reduces inflammation and numbs cheek area | Short-term (often 15–60 minutes) | No | Minimal if used correctly; avoid direct ice on skin |
| Saltwater rinse | Gently cleanses and soothes irritated tissues | Temporary | No | Low risk; avoid aggressive rinsing |
| Clove oil (eugenol) | Short-term numbing/comfort | Minutes to a few hours | No | Irritation/burn if overused or applied too aggressively |
| Hydrogen peroxide rinse (claimed antiseptic cure) | May reduce bacteria briefly; does not treat pulp | Temporary | No | Tissue irritation if overused or improperly diluted |
| Garlic paste / “viral hacks” | Mild soothing for some; not nerve-killing | Temporary | No | Burns/irritation to gums; delayed care |
| Root canal therapy | Removes infected/inflamed pulp, cleans, disinfects, seals | Often significant relief within 24–72 hours | Yes | Rare complications; requires proper restoration afterward |
| Filling | Removes decay and restores tooth structure | Long-term if decay is the cause | Yes (when decay is limited) | May not help if pulp is already irreversibly inflamed |
| Crown | Protects cracked/weak tooth and seals margins | Long-term | Yes (prevents ongoing irritation) | May be insufficient if pulp is infected without root canal |
| Gum treatment for root exposure | Reduces exposure and inflammation | Improves sensitivity over time | Yes (for gum-related causes) | Requires accurate diagnosis; may not address pulp infection |
| Extraction | Removes the damaged tooth entirely | Immediate source removal | Yes | Surgical risks; replacement planning needed |
Include common home remedies in the table
Cold compress, saltwater rinses, clove oil, and diluted antiseptic rinses may provide temporary comfort. They can help you manage pain while arranging dental care, but they do not remove the pulp problem or eliminate decay.
Because these methods are symptom-focused, they should be used only as interim support. If pain persists beyond a short window or worsens, a dentist should evaluate the tooth promptly.
Include professional options in the table
Root canal therapy, fillings, crowns, gum treatment for root exposure, and extraction are definitive options depending on the cause. The “best” treatment depends on whether the pulp is reversibly inflamed, irreversibly inflamed, or infected.
Professional care aims to stop the pain by removing the source and sealing the tooth. This is what makes relief durable rather than temporary.
Frequently Asked Questions
Is it possible to kill tooth nerve pain in 3 seconds permanently?
No. It isn’t possible to kill tooth pain nerve in 3 seconds permanently at home because the pulp is deep inside the tooth and protected by enamel and dentin. Home methods may numb or mask pain temporarily, but they cannot remove infected pulp or decay.
What will kill a tooth nerve safely?
Safe, definitive “nerve pain elimination” is typically done by a dentist through procedures that remove the source of irritation. In many cases, that means root canal therapy, which cleans and seals the pulp space to stop pain and prevent reinfection.
What’s the fastest way to stop tooth nerve pain at home?
The fastest at-home options usually include a cold compress, a gentle saltwater rinse, and appropriate over-the-counter pain relievers. Clove oil may provide short-term numbing for some people, but it is not a permanent solution.
Will tooth nerve pain go away on its own?
Sometimes pain may lessen temporarily, especially if inflammation fluctuates or if medication masks symptoms. However, pain improvement does not guarantee healing, and infection can continue even when the tooth feels better.
How do I know if I have an exposed nerve vs sensitivity?
Exposed or irritated pulp often causes sharp jabs, lingering throbbing, and sensitivity to hot/cold/sweet that lasts longer than typical enamel sensitivity. If pain is persistent, wakes you at night, or worsens with biting, an exam is strongly recommended.
When should I treat tooth pain as a dental emergency?
Seek urgent care for facial swelling, fever, spreading infection signs, difficulty swallowing, or rapidly worsening pain. These symptoms can indicate infection spread and may require prompt treatment to protect surrounding tissues.
Can I use alcohol/bleach or other DIY chemicals to “kill” the nerve?
No. Alcohol, bleach, and other harsh chemicals can burn soft tissues, worsen damage, and increase infection risk. They also delay proper care by masking symptoms.
What treatments can a dentist offer for permanent relief?
Depending on the diagnosis, dentists may recommend root canal therapy, fillings or crowns, gum treatment for root exposure, antibiotics when indicated, or extraction in severe cases. The lasting solution is removing the source of infection/decay and sealing/protecting the tooth so pain does not return.
If tooth pain is disrupting sleep, eating, or daily life, scheduling a consultation is the safest way to get real, lasting relief. A dental professional can identify the cause quickly and recommend the most appropriate treatment—so the pain stops for the right reasons, not just the short term. Contact Smile Avenue Family Dentistry to book an evaluation and discuss next steps.