Dental Implants in Cypress, TX: Procedure, Recovery, Cost Breakdown, and How to Know If Implants Are Right for You
If you are weighing tooth replacement options, dental implants cypress tx offer the most durable, natural-feeling solution for anything from a single tooth to a full-arch restoration. This practical guide explains how the procedure works, who is a good candidate, realistic recovery expectations, and local cost ranges so you can compare implants with bridges or dentures. You will also get a checklist for choosing a local provider and clear next steps to schedule an evaluation in Cypress, Bridgeland, Towne Lake, and northwest Houston.
How Dental Implants Work and Common Types of Implant Restorations
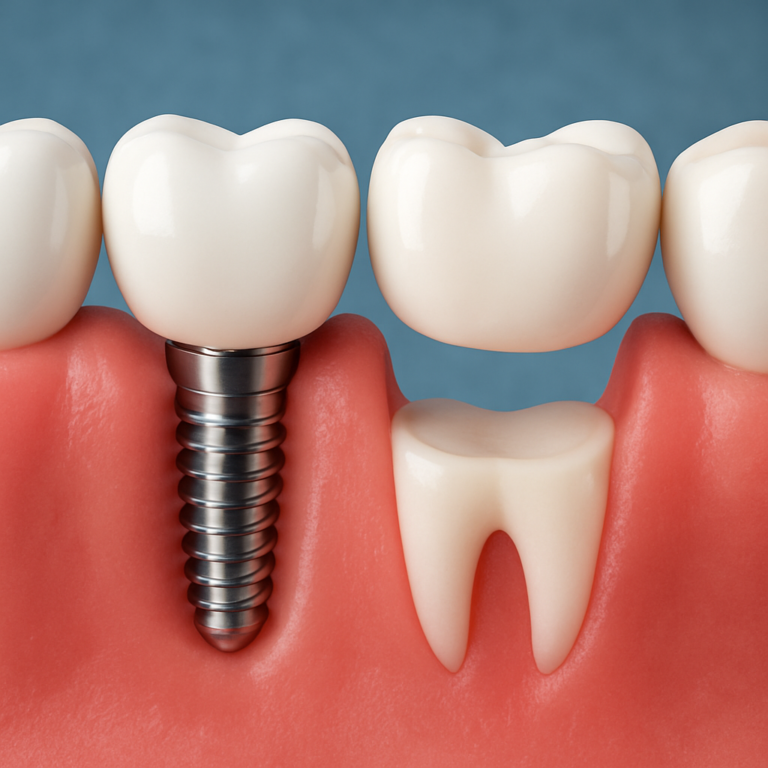
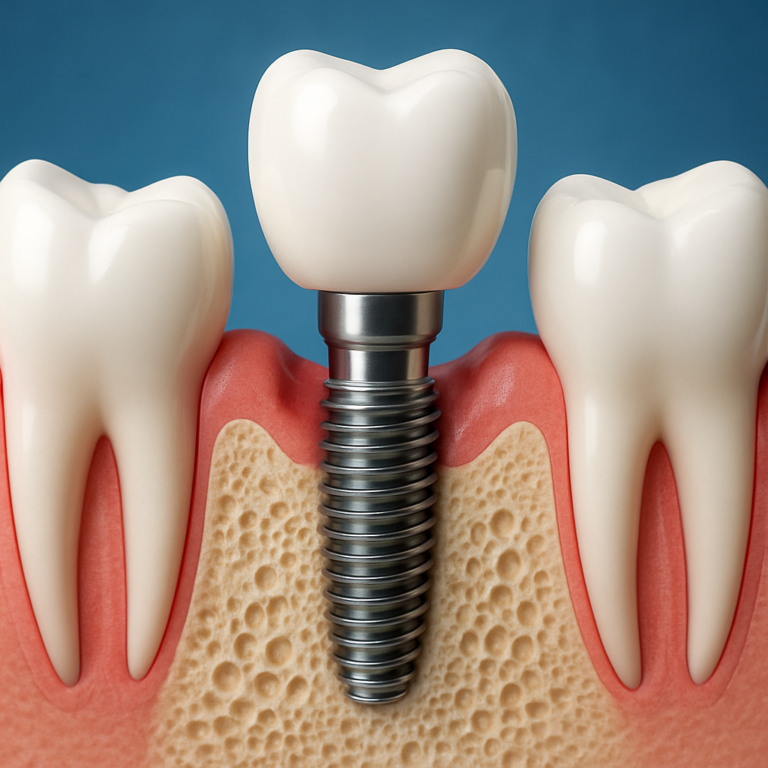
Basic mechanics: A modern dental implant is a three-part system: the fixture (the implant body placed in bone), the abutment (the connector), and the crown or prosthesis sitting above the gum. Osseointegration is the biological bond between bone and the implant surface; in routine cases clinicians plan for a healing window that lets that bond mature before final loading. Diagram suggestion: a simple vertical stack labeled fixture in bone – abutment at gum level – crown above the gum to show spatial relationships.
Common restoration types and when each is practical
- Single-tooth implant: replaces one missing tooth without altering adjacent teeth; best when surrounding bone is adequate.
- Implant-supported bridge: replaces two or more teeth when adjacent implants can support a multi-unit prosthesis; avoids preparing healthy teeth like a traditional bridge.
- Implant-retained denture / overdenture: uses two to four implants to stabilize a removable denture; practical when cost or bone limitations make full fixed workups impractical.
- Full-arch fixed solutions (for example All-on-4): uses strategically angled implants to support a fixed arch, often with immediate provisional teeth; useful for people with extensive tooth loss or poor dentures but requires strict hygiene and maintenance.
Practical tradeoff: Immediate-load or same-day restorations reduce time without teeth, but they trade speed for stricter candidacy requirements. If bone quality is marginal, clinicians who promise immediate teeth are increasing risk. In practice, predictable long-term outcomes depend more on bone volume and digital planning than on whether the crown is placed the same day.
Concrete example: A patient with one failing front tooth in Cypress often gets a single-tooth titanium implant with a provisional crown while the bone integrates; final ceramic crown follows once stability is confirmed. Conversely, a patient moving from unstable full dentures to fixed teeth may be treated with an All-on-4 protocol to regain immediate function, then return for refined prosthetics after healing.
Materials and reality check: Titanium implants have the longest clinical track record and the widest restorative options. Zirconia implants are attractive for metal-free restorations and certain aesthetic situations, but they have fewer connection options and less long-term data. Choose materials for the clinical need, not marketing claims.
Brand versus planning: Brand names like Straumann, Nobel Biocare, and Zimmer Biomet are common examples of reliable systems, but the limiting factor in outcomes is usually surgical planning and case selection. Ask about CBCT-based planning and guided placement rather than fixating on implant brand. For a general overview of implant therapy and patient resources see AAID patient resources. You can learn about local options at Smile Avenue services.
Step-by-Step What to Expect During the Implant Process at a Typical Dental Practice
Straight answer: expect a sequence of discrete appointments — evaluation, planning, surgery, and prosthetic follow-ups — not a single one-and-done visit unless you specifically qualify for immediate-load protocols. Each stage contains decisions that change cost, timeline, and risk.
Typical appointment schedule and durations
Common cadence: most practices schedule 4 to 6 visits from first consult to finished crown. That looks like: initial consult (30 to 60 minutes), CBCT and records (30 minutes, sometimes same day), implant surgery (45 to 120 minutes depending on complexity), short follow-ups in the first two weeks (10 to 20 minutes each), and one or two prosthetic visits for abutment and crown placement (30 to 90 minutes).
- Initial consult and imaging: medical/dental history, oral exam, and usually a CBCT when bone quality must be checked.
- Treatment planning visit (may be combined with consult): review digital plan, discuss immediate vs staged placement, review costs and financing.
- Surgery appointment: local anesthesia with optional sedation; surgeon places implant(s) and may place grafts or membranes if needed.
- Early healing checks: quick visits at 1 week and 2 weeks to monitor soft tissue and remove sutures if present.
- Prosthetic phase: uncovering or abutment placement, impressions or intraoral scan, then final crown or prosthesis delivery.
Practical tradeoff: choosing same-day provisional teeth reduces the time you go without a tooth, but it narrows who is eligible and raises the chance of adjustments later. If your bone is marginal, staged loading is slower but more predictable.
Questions to ask at each stage
- At the consult:How will you assess my bone volume (ask for CBCT)? Who will perform the surgery and how many implant cases do they do annually?
- Before surgery:What level of sedation do you offer, how long will I be numb, and what will I need at home the first 48 hours?
- Post-op visits:What are the check points and how quickly do you expect me back for the prosthetic phase?
- Prosthetic phase:Which abutment and crown materials do you recommend and what is the expected warranty or follow-up for adjustments?
Concrete example: a routine single front-tooth case in Cypress often follows this flow: consult with CBCT on day one, surgery the following week (about 60 minutes) with a provisional crown when esthetics matter, then a final crown appointment 3 to 4 months later after the implant has bonded. If a small graft is needed at surgery, the provisional timeline may stay the same; large grafts typically extend the wait by several months.
- What to bring to your first implant consult: a list of medications and medical conditions, any recent dental X-rays if available, dental insurance information, and a note of what bothers you most about the missing tooth/teeth.
Reality check: clinics that advertise two-visit implant completion are either selecting only ideal immediate-load candidates or using protocols that trade long-term predictability for speed. Ask for their long-term success data for cases like yours.
Next consideration: when you call to schedule, mention that you want a CBCT-based implant plan and ask whether they provide digital scanning and in-house lab work — those capabilities materially reduce surprises and extra appointments. To book at Smile Avenue, use Schedule a consult.
Who Is a Good Candidate and How to Improve Candidacy
Bottom line: many people who believe they are not candidates for dental implants in Cypress, TX are actually treatable after a few deliberate steps; the real question is whether those steps fit your timeline, budget, and overall health priorities.
Core candidacy factors: clinicians look for a stable oral environment, adequate jawbone where the implant will sit, and controlled systemic conditions. Active gum infection, poorly controlled diabetes, high tobacco use, and certain medications raise the risk of failure. None of these are always absolute disqualifiers, but each changes planning, cost, or healing time.
Practical improvements you can make before a consult
- Treat active gum disease: Complete periodontal therapy and maintain consistent cleanings; implants fail more often into infected sites.
- Optimize medical conditions: Bring recent lab values such as an HbA1c if you have diabetes and obtain clearance from your physician when advised.
- Reduce or quit smoking: Stopping tobacco improves blood flow and bone healing; even temporary cessation around surgery reduces complications.
- Plan for grafting if needed: If CBCT shows low bone, accept that grafting or sinus augmentation can create a predictable foundation but will lengthen the timeline and increase cost.
- Inventory medications and supplements: Tell your dentist about bisphosphonates, anticoagulants, or immune-suppressing drugs so your team can coordinate care with your physician.
Tradeoff to understand: rebuilding bone or treating periodontitis increases chances of long-term success, but it also means a longer process and more out-of-pocket expense. In practice, choosing a cheaper, faster path that skips disease control is the most common route to mid-term failure.
Concrete Example: A 58-year-old patient from Bridgeland presented with a missing lower molar and 30 percent bone loss at the site. The team recommended a short course of nonsurgical periodontal therapy, smoking cessation support, and a localized bone graft. That added two to four months and a predictable implant foundation; without grafting the alternative would have been a removable partial denture with lower long-term comfort and function.
What clinicians often get wrong about candidacy: many patients assume implant denial means permanent exclusion. The more useful question is which barrier needs fixing and whether the patient accepts the extra steps. Practices that promise same-day implants without addressing bone, infection, or systemic risk are taking a clinical shortcut that increases failure risk.
For technical background on candidacy criteria see the AAID patient resources at AAID patient resources. When you schedule a local evaluation, ask whether the practice uses CBCT planning and in-house restorative coordination; those capabilities materially reduce surprises. To book a consultation with Smile Avenue Family Dentistry – Cypress, visit Smile Avenue services.
Recovery Timeline, Aftercare, and Managing Complications
Straight to the point: implant recovery follows a predictable arc — an acute inflammatory phase, a soft-tissue healing window, and a slower bone integration period — each with different care needs and different risks. What you do in the first two weeks directly affects comfort; what you do in months two to six determines whether the implant becomes a reliable long-term anchor.
Week-by-week practical timeline
| When | What to expect | Actionable steps |
|---|---|---|
| Day 0 to 3 | Bleeding tapers, swelling peaks, moderate pain controlled with meds | Rest, apply ice first 24 hours, take ibuprofen 400 to 600 mg every 6 to 8 hours as needed unless contraindicated, check contraindications with your physician |
| Days 4 to 14 | Swelling reduces, sutures may be present, soft diet advised | Switch to warm salt rinses after 24 hours, avoid rinsing aggressively, return for suture removal if not dissolvable |
| Weeks 3 to 12 | Soft tissues mature, bone begins stable attachment | Gradually reintroduce firmer foods, attend scheduled follow-ups, avoid heavy chewing on the implant site until your dentist clears it |
| 3 months and beyond | Osseointegration assessment and prosthetic loading if planned | Maintain daily hygiene, begin long-term recalls, consider night guard for bruxism |
Practical limitation: pain control and swelling reduction are usually straightforward, but return-to-chewing is the compromise patients underestimate. Using a provisional crown for cosmetics is often safe, yet biting into a steak before your clinician confirms bone stability is a common cause of complications. Accept temporary dietary limits if you want predictable long-term results.
- Do: follow prescribed analgesics and anti-inflammatory dosing, keep the head elevated, use cold packs first 24 hours then warm compresses after 48 hours for comfort
- Do: use a 0.12% chlorhexidine rinse briefly if recommended (typical course 1 to 2 weeks), continue meticulous brushing away from the site, and attend all follow-ups
- Don't: smoke or vape during healing – even brief relapse raises failure risk; don't probe the surgical site with your tongue or fingers; avoid tipping a temporary restoration with heavy force
- Don't: take NSAIDs in higher-than-recommended doses without medical approval, and avoid abrupt interruption of blood thinners unless directed by your physician
Red flags that need immediate attention: increasing pain after day 4, fever over 100.4 F, persistent heavy bleeding, swelling that worsens instead of improving, implant mobility, or foul drainage. Contact your dentist right away if any occur.
Concrete example: a 52-year-old patient in Towne Lake had a lower premolar implant with a small bone graft. Swelling peaked on day 3 and was managed with ibuprofen and ice. Sutures were removed on day 7, soft chewing resumed at week 3, and the provisional crown was left light-contact until a 4-month CBCT confirmed stable bone for the final crown.
Managing complications in practice: routine issues are manageable in-office — small wound dehiscence, transient nerve paresthesia, or a loose healing abutment typically require repair or adjustment. Serious problems such as early implant mobility or progressive bone loss suggest failed osseointegration or infection and often require removal and staged retreatment. Antibiotics are not a substitute for good surgical technique and planning; overprescribing creates other risks.
If you notice any of the red-flag signs, contact your dental office immediately. For local support and rapid evaluation in Cypress, use Schedule a consult so the team can triage and, if needed, book an urgent visit.
Cost Breakdown for Dental Implants in Cypress, TX: Line Items and Typical Ranges
Straight numbers matter more than slogans. If you are budgeting for dental implants cypress tx, plan for multiple discrete charges rather than one bundled price: diagnostics, the implant fixture, restorative components, any hard-tissue work, sedation, and lab fees all add up and each line can swing the total by thousands.
| Line item | Typical range (USD) | Why the cost varies |
|---|---|---|
| Consultation + basic X-rays | $50 – $300 | Clinic pricing, whether consult includes exam plus treatment planning |
| CBCT 3D scan | $150 – $500 | Higher when image interpretation and surgical guides are included |
| Implant fixture (titanium or zirconia) | $900 – $2,000 | Brand, material, and internal connection type |
| Abutment (custom or stock) | $300 – $800 | Custom CAD/CAM abutments and zirconia abutments cost more |
| Final crown (ceramic/porcelain/zirconia) | $800 – $2,000 | Material, lab quality, and implant-to-crown complexity |
| Bone graft (localized) | $200 – $2,000 | Graft material, membranes, and surgeon time |
| Sinus lift (when required) | $1,000 – $3,000 | Technique complexity and whether grafting is simultaneous |
| Sedation (oral/IV) | $200 – $800+ | Sedation level, monitoring, and anesthesia provider fees |
| Lab fees / provisional prosthesis | $150 – $1,200 | Quality of provisional, digital vs traditional lab work |
Practical insight: paying more for a CBCT-based plan, guided surgery, and a reputable lab often saves money by reducing complications and rework. Cheap shortcuts – a low-cost fixture from an unknown supplier or skipping 3D imaging – create risk that typically becomes an expensive problem later.
Concrete example: A straightforward single-tooth implant in Cypress with no graft usually totals roughly $3,000 to $5,000 (CBCT, fixture, abutment, crown, routine lab work). If the CBCT shows bone loss requiring a localized graft, add $1,500 to $2,500 and expect the realistic total to be about $4,500 to $7,500 — the graft is the single largest common add-on that changes both timeline and price.
- Example: All-on-4 / full-arch: Requires individualized quoting; expect a wide range because surgical complexity, prosthetic design, and number of visits change the cost materially.
- Insurance reality: Most plans cover portions of the crown or removable prosthesis but often exclude the implant fixture. Confirm benefits and preauthorization with your insurer before treatment.
- Financing options: Consider CareCredit or LendingClub Patient Solutions, and review in-house financing or membership plans on the practice financing page at Smile Avenue financing.
When Implants Might Not Be the Best Option and Practical Alternatives
Clear decision point: dental implants are excellent long-term solutions, but they are not the right choice when the medical risk, bone situation, or patient priorities make grafting, extended timelines, or higher up-front cost unacceptable. In those situations, choosing a sensible alternative up front avoids needless procedures and aligns treatment with the patient reality.
When to prefer an alternative
Key considerations that push toward alternatives: uncontrolled systemic disease or recent head and neck radiation, active severe periodontal infection that the patient will not treat first, unwillingness to stop heavy tobacco use, or a budget and timeline that cannot accommodate bone grafting and staged care. Also consider long-term maintenance ability – some alternatives demand more frequent adjustments and follow-up.
- Fixed dental bridge – practical tradeoff: replaces one or several teeth quickly with predictable function and lower immediate cost, but it requires reducing healthy adjacent teeth and does nothing to stop bone loss under the missing tooth.
- Removable partial denture – when speed and low cost matter: inexpensive and fast to deliver; good as an interim solution. Downsides are lower comfort, appliance maintenance, and progressive ridge resorption that can limit future implant options.
- Implant-supported overdenture – middle path: two to four implants stabilize a denture for far better function than a removable partial at a fraction of full-arch fixed cost. Maintenance is higher than a fixed crown but stability and chewing improve substantially.
- Mini dental implants – lower invasion, specific uses: useful to retain dentures in narrow ridges or for patients who refuse grafting; they heal faster and cost less. They are not as robust under heavy chewing loads and have a different longevity profile compared with standard implants.
- Resin-bonded bridge (conservative anterior option): preserves adjacent tooth structure and is minimally invasive for a single front tooth, but the bond can fail over time and is not as strong for back teeth.
Practical insight: think about total cost of ownership, not just the sticker price. A cheap removable denture today can drive accelerated bone loss that makes later implant placement more complex and costly. Conversely, an implant overdenture can be a cost-effective way to regain function without full-arch reconstruction.
Real-world example: a 67-year-old patient in Cypress declined an extensive sinus graft after CBCT showed marginal posterior maxillary bone. The team provided a well-fitting removable partial to restore appearance and chewing immediately, then planned for a 2-implant overdenture once the patient secured financing. That sequence preserved options while respecting the patient's health and budget.
Clinical judgment worth stating: practices that present implants as the universal answer sometimes underplay how patient health, daily hygiene, and long-term follow-up change outcomes. If you prefer a lower-risk, reversible path, choose a solution that can be upgraded later – and make sure your provider documents a future-compatibility plan.