How Long Do Dental Implants Last? What to Expect and Tips to Make Them Last a Lifetime
How Long Do Dental Implants Last? What to Expect and Tips to Make Them Last a Lifetime
If you are asking how long do dental implants last, the straightforward answer is that the titanium implant fixture can last for decades, while the crown or prosthetic component commonly needs replacement every 10 to 15 years. This piece gives evidence-based survival ranges, a clear distinction between the implant body and the visible restoration, the main medical and mechanical risks that shorten lifespan, and practical maintenance steps you can use to maximize durability.
How long the implant fixture lasts versus the crown or restoration
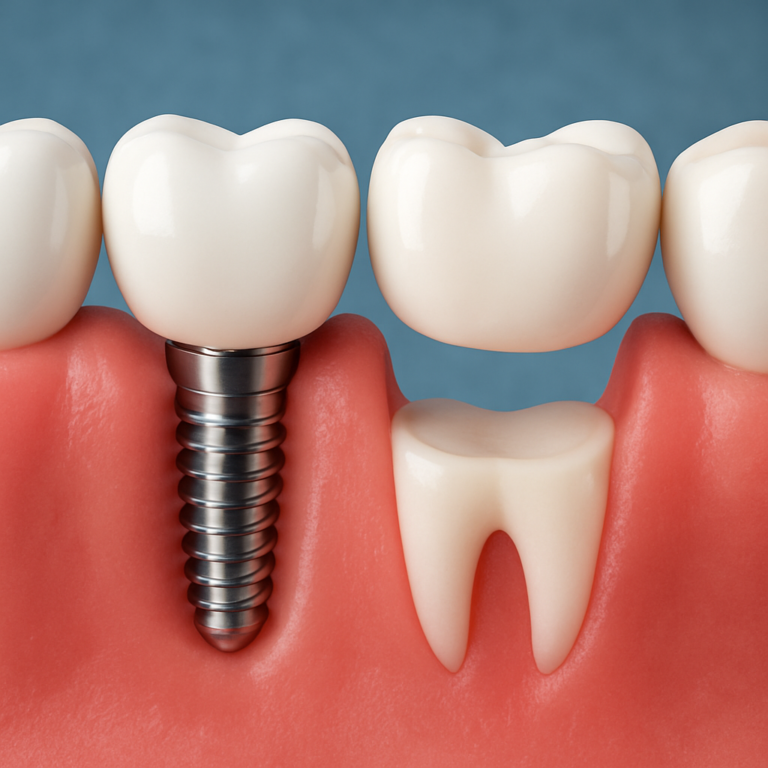
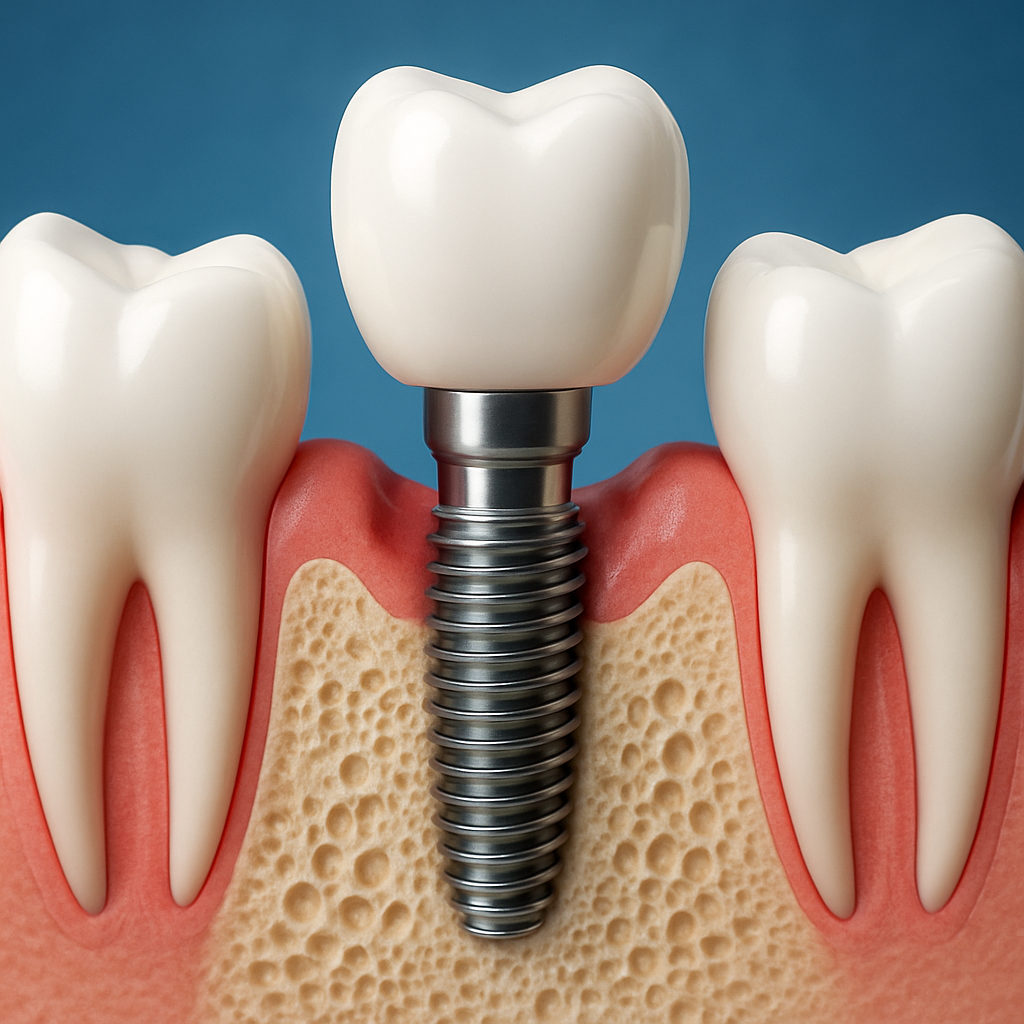
Two different lifespans. The metal or ceramic body placed into the jawbone and the visible tooth replacement above it behave like two different devices: one is integrated into biology, the other is a mechanical prosthesis subject to wear.
Why they age differently
Implant body: Osseointegration makes the fixture stable over long periods, but its survival depends on bone health and infection control. A successful implant becomes part of the jaw, so biological failure pathways such as bone loss from peri implant disease are the main threat.
Restoration: Crowns, abutments, and retention components fail for mechanical reasons: fracture, wear, screw loosening, or esthetic breakdown. These parts are replaceable without disturbing the implant in many cases, which matters for cost and treatment planning.
- Practical tradeoff: Choosing a highly aesthetic layered porcelain crown improves looks but increases risk of chipping compared with a solid zirconia crown.
- Clinical consequence: Replacing a worn crown is a straightforward restorative appointment; replacing a failing fixture requires more complex surgery and longer recovery.
Concrete example: A patient with a single lower molar implant presented after 7 years with a fractured veneered crown and new sensitivity when chewing. The implant body remained stable on exam and radiographs, so we replaced the crown with a monolithic zirconia restoration and fitted a nightguard to manage heavy clenching. That avoided surgical rework while addressing the underlying mechanical cause.
What the evidence shows. Systematic reviews report high midterm fixture survival, and clinicians usually see most failures early or years later due to biological complications. For readers who want deeper reading, see the Mayo Clinic overview and a relevant PubMed review.
Common misunderstanding. Patients often assume implants are maintenance free. That is wrong in practice. The implant body is resilient, but it is not immune to disease. Regular checks and hygiene stop small inflammation from becoming a failure that requires removing the fixture.
Key point: expect restorations to need periodic repair or replacement; protect the implant body by preventing gum disease and controlling mechanical overload.
Clinical timeline and what to expect after surgery and restoration
Short answer up front: healing follows a predictable set of clinic visits and checks — immediate wound care, a months-long bone integration window, then prosthetic adjustments and lifetime maintenance. Expect the first year to be the most hands-on period from your dental team; after that, surveillance and preventive care become the priority.
Typical clinic timeline (what your appointments will look like)
- Day 0 to 7: wound check and pain control. Stitches removed if needed, and we confirm the soft tissue is closing without unusual swelling or persistent bleeding.
- 2 to 4 weeks: soft tissue healing and oral hygiene coaching. We clean the area and show you targeted cleaning techniques for the implant site.
- 6 to 12 weeks: early radiographic check for initial bone response when indicated; we assess primary stability if considering early loading.
- 3 to 6 months: definitive osseointegration assessment and scheduling of the restorative phase unless immediate loading was performed.
- Restoration delivery: bite adjustments and soft tissue shaping. Plan for a one-week check and a short adjustment window afterward.
- 6 to 12 months post-restoration then ongoing: formal peri-implant review with charting, probing when indicated, and radiographs on a risk-based schedule (usually every 1–2 years).
Practical tradeoff to understand: choosing immediate or early loading speeds treatment but requires strong primary stability and excellent oral hygiene. If those conditions are marginal, delayed loading is less convenient but safer long term. In practice, pushing for speed when bone quality is poor is a common cause of early complications.
Concrete example: A 58-year-old patient received an upper premolar implant with adequate torque and had a provisional crown same day. At the two-week check we found mild mucosal inflammation from missed food around the provisional; targeted hygiene instruction and a short antiseptic rinse prevented progression and the final crown was placed at three months without further issues. That early clinic visit saved the implant from evolving into a more serious soft tissue problem.
Clinical judgment: many practices underuse radiographs after the first year unless symptoms appear. That saves time short term but misses gradual bone loss that is reversible if caught early. For patients with risk factors — smoking, prior periodontitis, diabetes, or bruxism — schedule more frequent imaging and three-to-six-month hygiene recalls.
Plan for a front-loaded schedule: expect several visits in year one, then risk-based reviews thereafter. Early detection of changes is the single most practical way to extend the lifespan of your implant.
Primary biological and mechanical factors that affect implant longevity
Straight to the point: the implant itself fails most often because of biological breakdown around the bone, while prosthetic or connection failures are driven by mechanical overload and poor restorative design. Understanding which side of the fence a problem sits on tells you whether the fix is medical, surgical, or simply a parts replacement.
Biological drivers
- Peri-implant infection: bacterial inflammation eats away bone. Mitigation: treat active periodontal disease before surgery, maintain strict plaque control, and schedule risk-based recalls.
- Systemic health influences: uncontrolled diabetes and immune suppression reduce healing capacity. Mitigation: stable medical control and communication with your physician before implant placement.
- Smoking and poor circulation: nicotine impairs bone remodeling and soft tissue health. Mitigation: quitting before surgery significantly lowers risk — discuss cessation resources with your dentist.
- History of aggressive periodontitis: past bone loss predicts future problems around implants. Mitigation: longer-term maintenance and more frequent imaging are warranted for these patients.
Mechanical drivers
- Excessive bite forces and bruxism: repeated overload causes screw loosening, component fracture, and marginal bone loss. Mitigation: prescribe a custom nightguard and consider stronger restorative materials.
- Poor prosthetic design: long cantilevers, inadequate implant number, or unfavorable implant angulation concentrate stress. Mitigation: plan restorations with the surgical team and use digital planning or CBCT when anatomy is tight.
- Small-diameter or short implants in weak bone: these solve immediate gaps without grafting but accept a mechanical tradeoff. Mitigation: weigh the short-term convenience against increased risk of mechanical failure and discuss alternatives like staged grafting.
Clinical tradeoff to know: choosing fewer implants for cost or to avoid grafting is common, but that shifts load to each implant and raises the chance of mechanical complications later. In many cases the cheaper upfront route creates more frequent repairs and higher long-term costs.
Concrete example: a 65-year-old patient received an upper full-arch overdenture on four implants without grafting because of limited budget. After three years of heavy clenching the prosthetic screws loosened repeatedly and the attachment inserts wore out fast. We revised the plan: added one additional implant in a strategic position, converted to stronger abutment screws, and supplied a nightguard — the episodes stopped and maintenance visits dropped in frequency.
Key judgment: biological problems progress silently; mechanical problems announce themselves early. Prioritize infection control first, then design restorations to survive the bite they will face.
Practical maintenance plan to make implants last a lifetime
Start with a plan, not hope. Maintenance that actually extends the life of an implant combines disciplined home care, scheduled professional checks, mechanical protection, and a small set of agreed monitoring triggers so problems are caught when they are fixable.
A step-by-step maintenance routine you can follow
- Baseline documentation: take a radiograph and peri-implant chart at restoration delivery and keep a dated photo. This baseline is what you and your dentist compare against later to detect slow bone loss.
- First-year checkpoints: schedule checks at 1 week, 1 month, 3 months and 6 months after restoration — each visit focuses on plaque control, soft tissue shape, and a quick mobility and occlusion check.
- Risk-based recall after year one: low-risk patients: hygiene visits and implant exam every 6 months; higher-risk (smoker, prior periodontitis, diabetes): every 3 to 4 months with yearly radiographs as needed.
- Mechanical protection: wear a custom nightguard if you clench or grind; avoid biting hard objects with implant crowns; choose less brittle restorative materials if you have heavy forces.
- Targeted home tools: use an appropriately sized interdental brush (common starting sizes: 0.6mm, 0.8mm, 1.2mm — your hygienist will fit the correct one), a soft-bristle brush, and either a water flosser or implant-specific floss for subgingival cleaning.
- When to get images: order a periapical radiograph if you notice any change in mobility, persistent inflammation, or a change in chewing; otherwise use risk-based imaging intervals rather than fixed yearly films.
- Record and communicate: bring a short medication and health update to every implant check — changes like new diabetes medications or osteoporosis drugs affect bone and healing.
Trade-off to accept: more frequent professional maintenance costs time and money, but it buys you the ability to fix small bone loss or mucosal inflammation non-surgically. Skipping recalls saves short-term expense and often increases the chance of a major surgical rescue later.
Concrete example: A 62-year-old patient with controlled type 2 diabetes agreed to four-month hygiene visits and a custom nightguard. At a routine three-month check a small pocket and 0.7 mm bone change were noted on radiograph; non-surgical cleaning and local antiseptic therapy halted progression and the implant remained stable for years without replacement of the fixture.
Practical judgment: ultrasonic scalers are fine for teeth but use plastic- or rubber-tipped instruments around implants to avoid roughening the implant surface. Also, aggressive whitening toothpastes and metal picks accelerate crown wear — choose gentle products and implant-safe cleaners.
If you want practical resources for scheduling and financing follow-ups at our Cypress or Katy offices, see our insurance and financing page or review general implant care guidance from the American Dental Association.
Signs of implant problems and when to call your dentist
Immediate red flags: new mobility of the crown or implant, continuous pus or a foul taste, worsening pain that does not respond to simple analgesics, or sudden changes in how your bite fits are not routine — these require prompt dental assessment.
Subtle warning signs to watch for: mild but persistent bleeding when you clean the area, gradual gum recession exposing the abutment, a recurring dull ache under the crown, or altered sensation in the lip or tongue near the implant. These often precede serious bone loss; catching them early lets your dentist treat inflammation rather than perform rescue surgery.
Clear actions vs watchful waiting
Not every symptom means the implant must be removed. Trade-off: acting too slowly risks irreversible bone loss and fixture failure; acting too aggressively can sacrifice a salvageable implant. The useful rule in practice is to call for an assessment if a problem persists longer than 48–72 hours or if you note mobility, drainage, or numbness.
- Call now: any looseness of the crown/abutment or visible movement of the implant body
- Call promptly: persistent pus, bad taste, or swelling that progresses over 24–48 hours
- Call within a day: new numbness, tingling, or sinus congestion after an upper implant
- Schedule soon: bleeding after gentle cleaning that does not stop or a steady increase in gum exposure around the implant
What to do before you get to the office: stop chewing on the side, photograph the area, save any broken pieces of crown, rinse gently with warm saline (no harsh mouthwashes), and avoid taking leftover antibiotics without contacting your dentist. These small steps preserve evidence and reduce the chance of making a later treatment more complex.
Concrete example: A woman had intermittent bad taste and slight mobility around a lower implant for three weeks but delayed calling. When she finally presented, radiographs showed progressive bone loss requiring surgical intervention. In another case a man called on day three of drainage; immediate non-surgical debridement, local antiseptics, and closer recalls controlled the infection and the implant remained in place long-term.
Early contact with your dentist is the single most practical action to protect the longevity of an implant — small problems treated quickly usually avoid major surgery.
Practical judgment from the clinic: insist on a baseline radiograph and a documented peri-implant chart when your restoration is delivered. If your provider cannot or will not produce that baseline, get a second opinion — delayed detection is the common reason otherwise healthy implants fail.
When components need repair or replacement and expected costs
Direct point: most implant problems you will actually pay to fix are prosthetic or attachment failures, not the titanium fixture itself. Crowns chip or wear, abutment screws loosen, and retention parts on overdentures degrade. Fixing those is usually straightforward; replacing the fixture is unusual and substantially more complex.
| Component | Typical failure or wear pattern | Usual fix and downtime | Typical cost band (USD) – ballpark |
|---|---|---|---|
| Crown or veneer | Chipping, wear, staining, esthetic breakdown | Replace the crown; often one appointment for impressions and one for delivery | low hundreds to low thousands |
| Abutment or screw | Screw loosening, abutment fracture, stripped threads | Tighten or replace screw/abutment; may need new lab part; short chair time | low hundreds to mid thousands depending on part and labor |
| Overdenture attachments | Worn inserts, loss of retention, plastic housings degrade | Replace inserts or housings; relining sometimes needed; quick turnaround | tens to a few hundred annually for routine replacements |
| Fixture failure | Progressive bone loss, uncontrolled infection, or catastrophic fracture | Remove fixture, debride, bone grafting as needed, then reimplant later | several thousand to many thousands; highly variable |
Tradeoff to accept: choosing a highly aesthetic, layered porcelain solution improves looks but increases the chance of chipping and earlier replacement. Conversely, monolithic zirconia sacrifices some translucency for durability and fewer repairs. Decide with your dentist which balance of appearance and longevity makes sense for your bite and budget.
Real-world case: A patient with an implant-retained denture began noticing looseness and food trapping after two years. The problem was worn locator inserts and a slightly cupped tissue surface. We replaced the inserts, relined the denture base, and adjusted occlusion; the patient regained function without surgery and returned to normal in a week.
When a fixture replacement becomes necessary
Fixture loss is primarily a biological problem – progressive bone loss from infection or failed integration. When that happens the remedy is surgical and often staged: remove the failed implant, treat infection, graft bone if needed, then reimplant after healing. This is not a routine refund; it is complex, time consuming, and the outcome depends on bone quality and your health status.
Practical judgment: it is far cheaper and simpler to invest in predictable, small repairs and regular maintenance than to gamble on avoiding follow up. Routine replacement of crowns or inserts keeps the whole system stable and usually prevents the rare but expensive need for fixture salvage or replacement.
How Smile Avenue Family Dentistry supports long term implant success
Our clinical focus is longevity over shortcuts. At Smile Avenue Family Dentistry we design implant care around predictable risk reduction: thorough diagnostics, coordinated surgical and restorative planning, and a documented maintenance pathway that follows each patient for years, not just until the crown is placed.
Clinic systems that matter for lasting results
Diagnostic depth: we use clinical charting, intraoral photos, and CBCT imaging when anatomy or bone quality could affect the outcome. Good planning reduces surprises that force compromises during surgery or restoration.
- Coordinated planning: surgical decisions and prosthetic design are made together so implants are placed where the restoration wants them to be, not the reverse.
- Documented baselines: every restoration delivery includes a radiograph and peri-implant chart stored in the record for future comparison.
- Hygiene training and role clarity: our hygienists are trained in implant maintenance, and each patient leaves with a personalized home care plan and specific interdental brush size recommendations.
Tradeoff to understand: we can expedite treatment with immediate loading in suitable cases, but when bone quality or inflammation risk is marginal we will recommend staged healing. That choice slows the process but materially reduces the chance of early biological failure.
Concrete example: a patient with a history of moderate periodontal disease wanted a single tooth replacement quickly. We completed active periodontal therapy first, obtained a CBCT, staged a bone grafted site, and delayed loading until soft tissue and bone were stable. The staged approach added treatment time but avoided reinfection and preserved the implant fixture long term.
Local logistics and follow up: we keep patients in Cypress and Katy on a recall schedule tailored to risk. The office proactively schedules peri-implant hygiene visits, sends reminders through the patient portal, and offers same-day triage for implant concerns so small issues are handled before they escalate.
Practical limitation: no clinic can guarantee an implant will last forever. Outcomes depend on patient health, habits, and adherence to follow up. Our promise is to manage modifiable risks, document the case, and intervene early so repairs remain minor rather than surgical rescues.
If you are comparing providers, prioritize documented planning, a clear maintenance program, and access to coordinated specialist care rather than lowest upfront price.