How Long Does It Take for a Wisdom Tooth to Emerge?
If you’re wondering how long does it take a wisdom tooth to come in once it starts, the honest answer is: it varies a lot. Some people notice a small nub and then feel gradual improvement over weeks, while others deal with months of soreness—or even a tooth that never fully settles into place. Understanding the stages of eruption and the reasons timelines change can help you know what’s normal, what’s not, and when to call your dentist.
How Long Does It Take a Wisdom Tooth to Come In Once It Starts?
Typical timeline from “first start” to full eruption
Once a wisdom tooth begins breaking through the gum, the process often takes weeks to several months to become fully erupted. In many cases, people first notice discomfort or pressure before any tooth is visible, and that “in-between” period can last a while as the tooth moves through bone and tissue.
For some individuals, it can take up to a year or more for the tooth to reach its final position—especially if the tooth is angled, there is limited space at the back of the jaw, or the gum tissue is thicker. Dental professionals commonly see situations where a tooth partially emerges, then stalls for months, and may only progress again when inflammation settles or space changes.
It’s also important to distinguish between “visible through the gum” and “fully erupted into final position.” A tooth may appear as a small white tip but still be far from aligned with the other molars, which affects both comfort and how easy it is to clean.
- Visible nub: a small portion of the crown may show, but the tooth may still be trapped under gum flap tissue.
- Partial eruption: more of the tooth is visible, yet it may not align properly or may continue to press on surrounding tissue.
- Full eruption: the tooth reaches a stable position in the bite and can be cleaned more effectively.
What “fully come in” really means (and why timelines vary)
“Fully come in” can mean different things depending on the context. In everyday terms, it may mean the tooth is visible above the gum line. In dental terms, it usually means the tooth has completed its eruption path and is positioned in a way that allows normal chewing and easier cleaning.
Wisdom tooth eruption is often described in stages: a pressure stage (movement inside the jaw), eruption through the gum, partial eruption (tooth breaks through but doesn’t finish), and full positioning (alignment and stabilization). Because each stage depends on bone density, gum thickness, and available space, timelines vary widely from person to person.
Another reason timelines differ: some wisdom teeth never fully erupt due to impaction or insufficient room. In these cases, the tooth may remain partially covered by gum tissue or become stuck against the second molar, which can cause ongoing irritation and infection risk even without “full eruption.”
- Pressure stage: the tooth moves slowly under bone; discomfort may come and go.
- Eruption through gum: a gum flap or swelling may appear as the crown approaches the surface.
- Partial eruption: the tooth may stop progressing and become harder to clean.
- Full positioning: the tooth aligns with the bite and is less likely to trap bacteria.
Quick age expectations (when people usually notice it)
Most people notice wisdom teeth eruption in the late teens through the mid-20s. Many dental professionals cite an approximate window of 17 to 25 years for initial eruption, but individual timing can shift earlier or later.
Some people don’t notice anything until their early 30s, while others may never erupt at all. It’s also possible for a wisdom tooth to be present in the jaw but remain fully impacted, meaning it never breaks through the gum line.
Age can influence how long it takes once eruption begins. As people get older, the jaw and surrounding tissues may become less flexible, and bone density can make movement slower—so a tooth that starts erupting in the late 20s or 30s may take longer to reach full position or may stall.
- Typical notice period: late teens to mid-20s
- Possible later eruption: sometimes early 30s
- Possible no eruption: some teeth remain impacted
Wisdom Teeth 101: What They Are and Why They Erupt Late
What is a wisdom tooth (third molar) and where it is
Wisdom teeth are the third molars, the last set of adult teeth to develop and erupt. They are located at the very back of the mouth—two on the upper jaw and two on the lower jaw in most people.
Not everyone has the full set. Some people have fewer than four wisdom teeth due to natural variation in tooth development, which can affect both symptoms and the “timeline” of what you notice.
Because they sit at the back, wisdom teeth are often harder to clean during eruption. That matters because partially erupted teeth can create a gum flap where food and bacteria can become trapped, increasing inflammation and discomfort.
Why they’re called “wisdom teeth” and why they appear later
They’re called “wisdom teeth” because they typically erupt later than other adult teeth, often in the late teens or early adulthood. The name is traditional rather than scientific, but the timing is consistent enough that the label stuck.
Evolutionary theories often explain the late timing by pointing to changes in jaw size and chewing needs over time. Many discussions suggest that as human diets shifted toward softer foods, the jaw may have less room for additional molars—making eruption more difficult for some people.
Even when wisdom teeth are present, the body may not “schedule” their eruption until later in adolescence. That delay is why discomfort often shows up when other adult teeth have already finished erupting and routine dental care has become more established.
Do all wisdom teeth need to erupt to cause problems?
No. Even if a wisdom tooth never fully emerges, it can still cause issues. Impacted or partially erupted teeth can press on nearby structures, contribute to crowding, or create an environment where bacteria thrive.
Dental professionals frequently see problems associated with partial eruption. A tooth that breaks through just enough to form a gum flap can trap debris, leading to inflammation around the crown and sometimes infection.
So, “not coming in” doesn’t always mean “no risk.” If symptoms occur—pain, swelling, recurrent bad taste, or gum irritation—an exam and X-rays can clarify whether a wisdom tooth is involved.
Why It Takes So Long: Causes That Affect Eruption Speed
Jaw size, available space, and crowding
Space is one of the biggest factors affecting how long it takes for a wisdom tooth to come in once it starts. If there isn’t enough room at the back of the jaw, the tooth may erupt slowly, partially erupt, or become fully impacted.
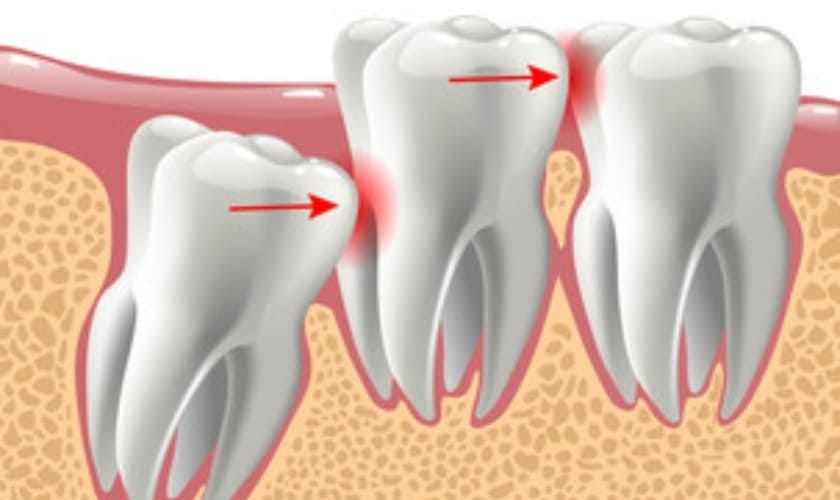
Limited space can also change the eruption path. Instead of moving straight upward, the tooth may angle toward the second molar, which can stall progress and increase pressure on adjacent teeth and gums.
Some people ask whether modern jaw size changes play a role. While the exact cause is complex, it’s commonly discussed that changes in diet and chewing patterns over generations may contribute to smaller jaws in some populations—meaning less room for third molars.
- Enough space: eruption may be faster and more complete
- Borderline space: partial eruption and longer timelines are more common
- Not enough space: impaction and non-eruption become more likely
Tooth position and eruption angle (vertical vs angled vs horizontal)
Even when a wisdom tooth begins to erupt, its angle can determine whether it progresses smoothly. A tooth that is positioned vertically is more likely to follow a typical eruption path, while an angled tooth may take longer or stop entirely.
Angulation can also lead to mesial or distal impaction, meaning the tooth is stuck leaning toward or away from the second molar. In more severe cases, the tooth may be oriented horizontally, which often prevents normal eruption.
When a tooth is “stuck under gum/bone,” it may still move slightly over time, which can explain why symptoms come and go. However, without enough room and the correct path, the tooth may never reach full alignment.
- Vertical: more likely to erupt fully (still variable)
- Angled: slower eruption, higher chance of partial eruption
- Horizontal: often impacted and less likely to erupt on its own
Genetics and missing wisdom teeth
Genetics can influence whether wisdom teeth develop at all, how many you have, and how they erupt. Some families see similar patterns—such as missing one or more wisdom teeth or having wisdom teeth that tend to be impacted.
Even among people with the same number of wisdom teeth, eruption timing can differ. That’s because genetic factors contribute to jaw size, tooth angulation, and the shape of the dental arch, all of which affect eruption speed.
Missing wisdom teeth can also change what “eruption timeline” means for you. If a tooth never develops or never exists, there is no eruption process—so symptoms may come from other causes like gum inflammation, cavities, or issues with the second molar.
Signs and Symptoms: How to Tell If Your Wisdom Tooth Is Coming In
Early warning signs before you see the tooth
Wisdom tooth discomfort often starts before any tooth is visible. A common early sign is a dull ache or pressure at the back of the jaw, sometimes felt near the angle of the jaw or even toward the ear.
Tenderness may develop near the second molar, and some people notice jaw tightness when chewing. These symptoms can be intermittent, which can make them easy to dismiss as general soreness.
Because other dental issues can mimic early wisdom tooth symptoms, it’s wise to pay attention to patterns. If discomfort keeps returning in the same spot over weeks, a dental exam can help determine whether a wisdom tooth is involved.
- Dull ache/pressure at the back of the jaw
- Tenderness near the second molar
- Jaw tightness or mild soreness when chewing
Eruption-phase symptoms (when it starts to poke through)
When a wisdom tooth begins to break through the gum line, the tissue at the back may become swollen or red. Soreness can increase when food gets into the area, and bleeding can occur if the gum flap is irritated.
Many people notice a small white nub or a gum flap (often called an operculum) that partially covers the tooth. This stage can be uncomfortable because the area is difficult to keep clean and bacteria can accumulate under the flap.
Bad taste or odor is another clue. Trapped food and bacteria under the gum flap can lead to a persistent “off” taste, especially after meals.
- Swollen/red gums at the back
- Soreness and occasional bleeding
- Bad taste/odor from trapped food under a gum flap
Red flags that suggest complications
Some symptoms suggest the wisdom tooth is not erupting normally and may be causing infection or significant inflammation. Difficulty opening the mouth (trismus), worsening pain, and swelling are important warning signs.
Fever or feeling unwell can also indicate infection. In these situations, waiting it out is not recommended—prompt evaluation helps prevent complications from spreading.
Bad breath or a foul taste that worsens alongside increasing gum inflammation can point to pericoronitis, an infection around a partially erupted wisdom tooth. Dental professionals typically recommend urgent assessment when red flags appear.
- Severe or worsening pain
- Swelling, fever, or feeling sick
- Trouble swallowing or opening the mouth
- Foul taste/odor with increasing inflammation
The Eruption Stages Explained (From Pressure to Full Position)
Stage 1 — Pressure and movement inside the jaw
Before a wisdom tooth is visible, it may be moving inside the jaw for months or even years. During this pressure stage, the tooth can press against bone and nearby structures, which may cause a dull ache or intermittent discomfort.
Because the sensation can fluctuate, some people experience “good weeks” followed by flare-ups. That pattern can happen when inflammation changes around the area or when chewing triggers pressure on the tissue.
In many cases, this stage is when people first suspect something is happening, even though no tooth is visible. If discomfort persists, dental professionals often recommend an exam and X-rays to confirm whether a wisdom tooth is erupting and how it’s positioned.
- Typical sensations: dull ache, pressure, intermittent discomfort
- Tooth may be moving internally long before visibility
- Symptoms may come and go based on inflammation
Stage 2 — Breaking through the gum line
Once the crown approaches the surface, the gum may become swollen and tender. People may notice a small white nub, a gum flap, or a localized red area at the back of the mouth.
This stage can be the most uncomfortable for many individuals. The gum flap can trap food and bacteria, and the area may be irritated each time you chew.
Even if the tooth appears to be “coming in,” it may still take time to progress beyond this stage. Some teeth break through and then stall, which is why ongoing symptoms should be evaluated rather than assumed to be temporary.
- Small nub or gum flap may appear
- Swelling/redness and soreness are common
- Food trapping under the flap can worsen discomfort
Stage 3 — Partial eruption vs full eruption (and what happens next)
In partial eruption, the tooth breaks through but stops progressing. This can happen if the tooth hits resistance from bone, lacks space, or is angled in a way that prevents it from reaching its final bite position.
Partial eruption often makes cleaning harder. Food and bacteria can accumulate around the gum flap, increasing the risk of repeated inflammation episodes and sometimes cavities or gum disease in nearby teeth.
In full eruption, the tooth continues until it aligns with the other molars (when space allows). At that point, symptoms may improve because the gum flap is less likely to trap debris and the tooth becomes easier to brush and floss.
- Partial eruption: tooth stops; harder to clean; more inflammation risk
- Full eruption: progresses into bite position; often less gum irritation
- Next step: monitoring or treatment depending on symptoms and X-ray findings
Impacted or Partially Erupted Wisdom Teeth: What It Means for Timing
Definitions: impacted vs partially erupted vs fully erupted
An impacted wisdom tooth is stuck under gum and/or bone and cannot erupt normally. A partially erupted tooth is partly visible but may not continue to progress, often because it is blocked or angled.
A fully erupted wisdom tooth has reached its expected position in the mouth. It may still be difficult to clean depending on how far back it sits, but it is generally less likely to create a persistent gum flap environment.
It’s also helpful to remember that “not coming in” doesn’t always mean “not present.” Many impacted teeth remain in the jaw for years and can still cause symptoms when they press on surrounding tissue or create a pathway for bacteria.
- Impacted: stuck under gum/bone
- Partially erupted: partially visible but stalled
- Fully erupted: aligned and stable in the bite
How impaction changes the timeline (and why it can stall for months/years)
Impaction can dramatically change eruption timing. If the wisdom tooth is angled and lacks space, it may halt eruption entirely—meaning it can stall for months, years, or never fully emerge.
Some teeth appear to “almost come in,” then stop. This can happen when the tooth reaches a point where it encounters dense bone or meets resistance from the second molar. The result is often a cycle of irritation: inflammation flares up, then calms down, then flares again.
In many cases, a tooth may never fully erupt on its own. Dental professionals may recommend monitoring or extraction depending on symptoms, the tooth’s position, and the risk to nearby teeth.
- Angled teeth may not have a clear eruption path
- Limited space can halt progress
- Some teeth never fully erupt without treatment
Common complications linked to partial eruption
Partial eruption is a common setup for complications because the gum flap can trap food. This increases the risk of pericoronitis, which is inflammation and sometimes infection around the partially erupted tooth.
Repeated inflammation can lead to swelling, pain, and difficulty chewing. Over time, the area can become more challenging to clean, increasing the risk of cavities or gum disease not only around the wisdom tooth but also on the adjacent second molar.
Impacted or partially erupted wisdom teeth can also contribute to crowding and pressure. While not every case causes noticeable tooth movement, dental professionals often evaluate whether the wisdom tooth is affecting the alignment of neighboring teeth.
- Pericoronitis and gum inflammation
- Food trapping and recurrent bad taste/odor
- Higher cavity/gum disease risk near the second molar
- Potential crowding or pressure effects
Treatment Options: What Dentists Do When Wisdom Teeth Don’t Erupt Normally
When watchful waiting is appropriate
Not every wisdom tooth needs immediate treatment. If a wisdom tooth is healthy, not causing pain, and not creating gum problems, your dentist may recommend watchful waiting with periodic monitoring.
Monitoring typically involves clinical exams and X-rays to track position and eruption changes. This approach can be appropriate when the tooth is unlikely to cause harm and symptoms are absent or minimal.
Even with watchful waiting, good oral hygiene and prompt reporting of new symptoms matter. If discomfort returns or inflammation develops, the plan may change based on updated findings.
- Tooth is asymptomatic and not causing gum issues
- X-rays suggest low risk to nearby teeth
- Regular checkups to reassess eruption progress
When extraction is recommended (and why)
Extraction may be recommended when wisdom teeth cause recurrent pain, infection, or gum inflammation. It may also be advised if the tooth is contributing to crowding, damaging nearby teeth, or creating a high risk of decay and gum disease.
Some dentists recommend removal preventively in certain situations, such as when X-rays show a tooth is positioned in a way that makes future problems likely. Other recommendations are symptom-driven, meaning extraction becomes the best option after repeated episodes of pericoronitis or persistent discomfort.
In general, the decision depends on factors such as the tooth’s angle, depth of impaction, proximity to nerves, and overall oral health. Your dentist may discuss benefits and risks so the plan fits your specific situation.
- Recurrent infection or inflammation
- Persistent pain or difficulty cleaning the area
- Crowding or damage to the second molar
- Concerns seen on imaging (position, cyst risk, etc.)
What to expect from evaluation and imaging
Evaluation usually starts with an exam of the back of the mouth and a review of symptoms. Dental professionals often ask about pain patterns, swelling, bad taste/odor, and whether chewing worsens discomfort.
X-rays are essential for determining whether the tooth is vertical, angled, or impacted, and whether there is enough space for eruption. Imaging also helps assess whether the wisdom tooth is likely to progress, stall, or cause harm to adjacent teeth.
Based on findings, your dentist may recommend continued monitoring, targeted treatment for inflammation, or extraction. The goal is to reduce pain and prevent complications while keeping the plan realistic for your timeline and comfort.
- Clinical exam of gum tissue and bite area
- X-rays to determine position/angle/space
- Plan tailored to eruption likelihood and risk level
Pain Relief and Self-Care While You Wait for Eruption
Safe at-home comfort measures (general guidance)
While waiting for eruption—or while deciding on next steps—comfort measures can help. Warm saltwater rinses are a common option because they may soothe irritated gum tissue and support gentle cleansing around the area.
Gentle oral hygiene is important, especially if a gum flap is present. Brushing normally while being careful around tender tissue can reduce plaque buildup, and flossing may help if it can be done comfortably.
Over-the-counter pain relief may help some people, but it should be used according to the product label and any clinician guidance. If you have medical conditions or take medications, it’s best to confirm safe options with your dentist or pharmacist.
- Warm saltwater rinses to reduce irritation
- Gentle brushing and careful cleaning around the back molars
- OTC pain relief as directed by label/clinician advice
What to avoid during eruption
Some well-meaning habits can make eruption discomfort worse. Avoid poking the gum flap or trying to “lift” tissue with tools, since this can increase inflammation and delay healing.
Aggressive cleaning can also irritate the area. If brushing causes sharp pain or bleeding, it may be better to use gentle technique and focus on consistent, careful hygiene rather than vigorous scrubbing.
Most importantly, avoid delaying care when symptoms worsen. Wisdom tooth pain that escalates, swelling that spreads, or signs of infection should be evaluated promptly rather than managed indefinitely at home.
- Avoid poking or manipulating the gum flap
- Avoid aggressive scrubbing that increases irritation
- Don’t wait too long if pain, swelling, or infection signs worsen
When home care isn’t enough (seek urgent dental evaluation)
Home care is not a substitute for professional evaluation when red flags appear. Seek urgent dental assessment if pain becomes severe or rapidly worsening, especially if it’s accompanied by swelling.
Fever, trouble swallowing, or difficulty opening the mouth are also reasons to seek prompt care. These symptoms can indicate infection that may require treatment beyond rinses and OTC pain relief.
Increasing foul taste or odor along with worsening gum inflammation can be consistent with pericoronitis. In these situations, dental professionals may recommend prescription medication, irrigation, or other interventions depending on severity.
- Severe or worsening pain
- Swelling, fever, or feeling unwell
- Trouble swallowing or opening the mouth
- Foul taste/odor with increasing inflammation
Prevention and Long-Term Management (Before Problems Start)
How regular dental visits help catch issues early
Regular dental visits help identify wisdom tooth risk before it becomes a crisis. Dental professionals can monitor eruption status, check for gum irritation, and evaluate whether a tooth is likely to become impacted or cause crowding.
Early identification can reduce complications and make treatment easier. For example, if X-rays show a tooth is angled and likely to cause recurrent inflammation, planning can happen before repeated infections occur.
Even if a wisdom tooth is not bothering you yet, routine exams provide the baseline needed to compare future changes. That makes it easier to decide whether watchful waiting remains appropriate.
- Monitor eruption progress and gum health
- Detect impaction risk with X-rays
- Reduce complexity by planning early when needed
Keeping the area clean if a gum flap forms
If a gum flap (operculum) forms over a partially erupted tooth, hygiene becomes more important. Food and bacteria can collect under the flap, so consistent cleaning can reduce inflammation episodes.
Practical cleaning often includes gentle brushing along the gum line and careful rinsing after meals. Some people benefit from a dentist-recommended technique for cleaning around partially erupted areas, especially if flossing is difficult.
Because inflamed tissue can bleed, it’s normal to feel some sensitivity at first. The key is to keep the area clean without causing trauma—gentle, consistent care tends to work better than aggressive scrubbing.
- Brush gently along the back molars and gum line
- Rinse after meals to reduce trapped debris
- Ask your dentist about techniques if flossing is painful
Timing considerations for extraction (if needed)
When extraction becomes necessary, timing can influence ease of removal and recovery. In many cases, earlier intervention can be simpler because roots may not be fully developed and the surrounding tissues may be more adaptable.
Complexity and recovery can increase with age and with the severity of impaction. While individual experiences vary, dental professionals often discuss expected recovery ranges, which commonly include several days of soreness and swelling, followed by gradual improvement over about 1–2 weeks.
Your dentist can explain what timing makes sense based on X-ray findings, your symptoms, and your overall health. The goal is to prevent repeated infections and protect nearby teeth while minimizing downtime.
- Earlier removal may be easier in some cases
- More severe impaction can increase complexity
- Recovery varies, but many people improve noticeably within 1–2 weeks
Frequently Asked Questions
Once it starts, how long does it take a wisdom tooth to come in?
Once a wisdom tooth begins breaking through the gum, it often takes weeks to several months to fully erupt. In some cases, it can take up to a year or more, especially if space is limited or the tooth is angled or partially impacted.
Some wisdom teeth partially erupt and then stall for months, while others may never fully settle into their final position without dental treatment.
Can a wisdom tooth take years to come in after it starts?
Yes. Eruption can be slow, and some teeth partially emerge and then stall for months or even years. In other situations, the tooth may never fully erupt due to impaction or lack of space.
Symptoms may also fluctuate during that time, which can make the process feel unpredictable.
What are the first signs that my wisdom tooth is coming in?
Common early signs include a dull ache or pressure at the back of the jaw and tenderness near the second molar. Some people also notice mild jaw tightness or discomfort when chewing.
When the tooth is closer to the surface, a gum flap or small white nub may become visible.
Why does my wisdom tooth hurt even if it’s not fully out?
Pain can happen even when a wisdom tooth isn’t fully erupted because partial eruption often creates a gum flap that traps food and bacteria. That can lead to inflammation and sometimes pericoronitis.
Additionally, an impacted or angled tooth can press on surrounding tissue, causing pressure-related discomfort.
How do I know if my wisdom tooth is impacted?
Symptoms alone can’t confirm impaction, but they can raise suspicion—especially if pain persists in the same back area. An X-ray is the main way dental professionals determine whether the tooth is stuck under gum or bone or angled in a way that prevents normal eruption.
Your dentist can interpret the tooth’s position and explain whether it’s likely to erupt or stall.
When should I see a dentist about wisdom tooth pain?
Schedule a dental visit promptly if pain is severe, worsening, or accompanied by swelling. It’s also important to be seen if there is fever, bad taste/odor that’s increasing, or trouble opening your mouth.
Early evaluation helps prevent complications and can reduce the chance of repeated infections.
Do all wisdom teeth need to be removed?
No. Some wisdom teeth erupt normally and never cause problems, so they may be monitored instead of removed.
However, others are removed due to impaction, recurrent pain or infection, crowding, decay risk, or concerns seen on imaging.
Comparison: Typical Eruption vs Partial Eruption vs Impacted Wisdom Teeth
Timeline and visibility differences
Wisdom teeth can look very different depending on how far along they are and whether they have enough space. Typical eruption often progresses steadily, while partial eruption may show visible progress that then stalls.
Impacted teeth may never become visible at all, or they may only show a small portion while the rest remains trapped under gum or bone. This difference is one reason the question how long does it take a wisdom tooth to come in once it starts can have such varied answers.
| Condition | Visibility | Typical timeline after “starting” | What often happens next |
|---|---|---|---|
| Typical eruption | Gradual emergence above gum line | Weeks to several months | Often reaches stable bite position |
| Partial eruption | Tooth breaks through but stops | May stall for months; sometimes longer | Higher risk of gum flap inflammation |
| Impacted | May be submerged or only minimally visible | May never fully erupt | May require monitoring or extraction |
Symptom patterns
Typical eruption often causes mild, intermittent pressure that improves as the tooth becomes more fully exposed. Partial eruption tends to create a more consistent pattern of soreness, especially after meals, due to trapped debris under the gum flap.
Impacted wisdom teeth may cause deeper, persistent pain or pressure, sometimes with swelling episodes. Red flags—such as fever, significant swelling, or trouble opening the mouth—suggest complications and warrant prompt evaluation.
- Mild pressure/tenderness: more consistent with early or typical eruption
- Recurrent inflammation/pericoronitis: common with partial eruption
- Severe pain/swelling/red flags: suggests infection or significant impaction
Likely dental recommendations
Dental recommendations depend on symptoms and imaging. With typical eruption and minimal symptoms, watchful waiting and good hygiene may be enough.
For partial eruption, dentists often focus on reducing inflammation and improving cleaning access. If infections keep recurring or the tooth threatens nearby teeth, extraction may be recommended.
For impacted teeth, the plan often depends on position and risk. Some impacted teeth can be monitored, while others are removed to prevent ongoing pain, infection, crowding, or damage to adjacent teeth.
- Watchful waiting: typical eruption, low risk, no symptoms
- Hygiene-focused management: partial eruption with manageable inflammation
- Extraction evaluation: recurrent infection, significant impaction, or risk to nearby teeth
If wisdom tooth discomfort is starting—or if symptoms have been lingering—scheduling a consultation with your dentist is the best next step. An exam and X-rays can clarify whether a tooth is erupting normally, partially erupting, or impacted, and can help create a plan that prioritizes comfort and long-term oral health.