How Long It Takes for a Loose Tooth to Naturally Fall Out in Adults
Discovering a loose tooth adult can feel alarming—especially because permanent teeth are expected to last for life. Unlike the natural looseness of childhood, adult tooth mobility usually signals that something is affecting the gums, ligaments, or bone that hold the tooth in place. The most important takeaway is that timing matters: early evaluation can greatly improve the odds of saving the tooth.
What “loose tooth adult” means (and why it’s different from baby teeth)
In adults, a “loose tooth” typically means the tooth has increased movement beyond what’s considered normal. Teeth are held in place by a combination of the periodontal ligament, gum tissue, and surrounding jawbone, and any disruption to these supports can make a tooth wobble. For most people, even slight mobility is a sign that your mouth is telling you something needs attention.
Baby teeth loosen because their roots are designed to resorb as the permanent teeth develop underneath. Adult teeth, however, are not meant to loosen on their own as part of normal growth. When an adult tooth becomes mobile, it generally reflects an underlying issue—most commonly gum disease, trauma, or pressure-related damage.
How adult tooth mobility is measured (what “loose” can look like)
Dental professionals evaluate mobility by gently assessing how much the tooth moves and how the movement behaves. This helps your dentist estimate whether the tooth is still supported well enough to stabilize, or whether deeper damage may be present. Mobility is not just “feels wiggly”—it’s a measurable change in how the tooth responds to gentle force.
- Slight wobble: the tooth may move a little when touched or during biting, often with minimal discomfort.
- Moderate mobility: the tooth shifts more noticeably and may feel unstable when chewing or cleaning.
- Advanced mobility: the tooth can move significantly, sometimes with pain, gum swelling, or signs of infection.
It’s also important to know that adult teeth should not loosen naturally without an underlying cause. Even if the tooth doesn’t hurt, mobility can reflect early gum or bone changes that are still treatable.
Why a loose adult tooth can’t be ignored
Tooth looseness is often a visible sign of damage that may be happening beneath the gumline. The periodontal ligament and supporting bone can be weakened by inflammation, infection, or repeated stress, and once support is lost, the tooth can become harder to save. Your dentist may be able to stop progression, but delaying care can allow the problem to advance.
In many cases, early treatment improves the odds of stabilizing the tooth and preventing further bone loss. For example, gum disease can often be managed more effectively when caught before significant structural damage occurs. When a tooth is already mobile, it’s a strong signal that the supporting tissues deserve prompt attention.
- Mobility links to support damage: gums, ligaments, and bone work together to hold teeth firmly.
- Early care helps: addressing the cause sooner can reduce the chance of eventual extraction.
- Ignoring it increases risk: untreated inflammation can worsen over weeks or months.
The “no tooth fairy” reality: can it tighten back up?
Some adult teeth may stabilize if the underlying cause is treated quickly and effectively. For instance, if mobility is related to early gum inflammation, professional cleaning and improved home care may allow the tissues to calm down and the tooth to feel less loose. Studies and clinical experience generally suggest that earlier intervention offers better outcomes.
That said, persistent looseness usually means the tooth’s support has already been compromised. If bone loss or ligament damage is advanced, the tooth may not “tighten” on its own, even with good brushing. In those situations, dental professionals may recommend stabilization (such as splinting), deep cleaning, and sometimes surgical options.
The key is that “tightening back up” depends on the cause and how far the problem has progressed. Your dentist can’t reliably predict the outcome without an exam and imaging, but prompt evaluation is the best way to maximize the chance of saving the tooth.
Common causes of a loose tooth in adults
Adult tooth mobility has a short list of common causes, and most are treatable when addressed promptly. The right treatment depends on the cause—so identifying what’s driving the looseness is just as important as treating the symptoms. Below are the most frequent reasons a loose tooth adult situation develops.
Gum disease (periodontal disease) — the leading cause
Gum disease is the most common reason adults develop loose teeth. Plaque and tartar buildup can trigger chronic inflammation, which may gradually damage the gums and the bone that supports teeth. Over time, the tooth may begin to wobble as the periodontal ligament loses its firm attachment.
Clinically, gum disease often progresses in stages. Many people start with gingivitis (gum inflammation that may cause bleeding), and if it’s not treated, it can advance into periodontitis, where deeper tissues and supporting bone are affected. Once bone loss occurs, mobility becomes more likely.
- Gingivitis: gums may bleed during brushing; tenderness or redness can appear.
- Periodontitis: inflammation extends deeper, leading to attachment and bone loss.
- Mobility: as support weakens, the tooth may shift during chewing.
Because gum disease can be painless early on, some people notice mobility only after the condition has progressed. That’s why regular dental visits and professional cleanings are so important.
Trauma and injury (sports, falls, contact)
Trauma is another major cause of adult tooth looseness. A blow to the mouth—such as from a fall, sports contact, or an accident—can damage the periodontal ligament even if the tooth doesn’t crack. The tooth may feel loose immediately or become more mobile over the next days as swelling and tissue healing evolve.
Immediate evaluation matters because ligament injuries and root-related damage may not be obvious at first. Dental professionals may need to assess whether the tooth’s position changed, whether the root is affected, and whether stabilization is required. Sudden onset after an impact is a red flag that should not be ignored.
- Sudden looseness after impact: often indicates ligament injury.
- Chewing pain: can suggest deeper support damage.
- Delayed symptoms: sometimes appear days later, so monitoring is important.
If trauma is involved, your dentist may recommend prompt imaging and a stabilization plan to protect the tooth while tissues heal.
Bone and pressure-related causes (osteoporosis, bruxism, other health factors)
Some causes of adult tooth looseness are related to bone health and repeated mechanical stress. Osteoporosis can reduce bone density, including in the jaw, which may weaken the support around teeth. While osteoporosis doesn’t automatically cause loose teeth, it can increase vulnerability—especially when combined with gum disease.
Bruxism (clenching or grinding) is another common contributor. Over time, excessive forces can strain the periodontal ligament, worsen inflammation, and accelerate mobility. People may not realize they grind, but signs such as worn tooth surfaces, jaw soreness, or headaches can provide clues.
- Osteoporosis: reduced jawbone density may affect tooth stability.
- Bruxism: grinding increases stress and can loosen teeth over time.
- Other accelerators: hormonal changes, pregnancy-related gum sensitivity, and certain medications may contribute indirectly.
Other health factors can also play a role, including uncontrolled diabetes and immune-related conditions that affect healing. Your dentist may coordinate with your physician if systemic factors are suspected.
Age range and risk factors: when adults start noticing loose teeth
While any adult can experience tooth mobility, risk often increases with age due to cumulative gum inflammation and bone changes. Many people notice their first loose tooth adult issue in midlife, but younger adults can still develop mobility from trauma, aggressive gum disease, or untreated decay.
Typical age window (e.g., 40–60) and why risk increases
Many cases become more common between ages 40 and 60 as periodontal disease progresses over years. Gum disease is often slow-moving, and the effects of inflammation and bone loss can accumulate gradually. By midlife, some people have had enough exposure to plaque and tartar buildup for the supporting tissues to weaken.
That said, age is not destiny. A younger adult can have a loose tooth due to a sports injury, a sudden infection, or rapidly progressing gum disease. Conversely, older adults may have stable teeth if periodontal health has been well maintained.
- Midlife risk increases: cumulative periodontal progression and bone changes.
- Variability is normal: trauma and aggressive gum disease can occur at any age.
- Individual factors matter: genetics, hygiene habits, and health conditions influence outcomes.
Personal risk factors that raise the odds
Several risk factors make tooth mobility more likely. Smoking is strongly associated with periodontal disease and slower healing, which can worsen gum inflammation and bone loss. Poor oral hygiene and irregular dental visits can allow plaque to build up, increasing the chance of advanced gum damage.
Existing periodontal history is another major predictor. If you’ve had deep pockets, previous gum treatment, or known attachment loss, the risk of future mobility is higher—especially if maintenance care has been inconsistent. Chronic grinding can also increase stress on teeth, making them more susceptible to loosening.
- Smoking: increases periodontal inflammation and reduces healing capacity.
- Poor plaque control: missed brushing/flossing allows tartar buildup.
- Irregular dental visits: delays detection and treatment of early gum disease.
- Chronic grinding: adds repeated force to already stressed tissues.
When to suspect something more than “normal wear”
Most people associate tooth problems with pain, but mobility can be a warning sign even without discomfort. It’s especially important to suspect something more serious if mobility is sudden, affects multiple teeth, or comes with gum changes such as swelling or bleeding. These patterns can suggest active periodontal disease, infection, or trauma-related ligament injury.
Systemic risk factors also raise concern. For example, if osteoporosis is present or suspected, a loose tooth may reflect reduced jawbone support in addition to gum inflammation. In these cases, dental professionals may recommend a coordinated approach to address both oral and overall health.
- Sudden mobility: especially after an injury or without a clear reason.
- Multiple teeth loosening: may indicate more widespread periodontal or bone issues.
- Systemic symptoms: fever, significant swelling, or feeling unwell can suggest infection.
If any of these apply, prompt dental and, when appropriate, medical evaluation is the safest path.
Symptoms and warning signs of tooth mobility (what to watch for)
Tooth mobility rarely appears without other clues. Even when the tooth feels loose, the gums and surrounding tissues often show early signs of inflammation or damage. Paying attention to these signals can help you seek care before the situation worsens.
Early signs of mobility (subtle wobble and gum changes)
Early mobility can be subtle. Some people notice a slight shift during brushing, flossing, or when biting down on food. Others feel the tooth move when they press it gently with their tongue, even if it doesn’t hurt.
Gum changes often accompany early mobility. Redness, swelling, and bleeding during brushing can indicate inflammation that may be progressing. In some cases, gum recession is visible, which can expose more of the tooth root and increase sensitivity.
- Slight movement felt during cleaning or biting
- Bleeding gums when brushing or flossing
- Redness or swelling around the tooth
Because early gum disease can be painless, these signs may be the first “alarm bell” that something is wrong beneath the surface.
Serious symptoms that suggest infection or advanced damage
Some symptoms indicate the problem may be more advanced or involve infection. Pain when chewing, a bad taste, or pus near the gumline can suggest an abscess or active infection. Fever or feeling generally unwell can also be a sign that the body is responding to infection.
Advanced damage may come with a sudden increase in mobility. If the tooth becomes noticeably more loose over a short period, that can reflect worsening inflammation, ligament damage, or progression of bone loss. Visible discharge or swelling of the gum tissue are also concerning signs.
- Pain with chewing or throbbing discomfort
- Pus/bad taste near the gums
- Fever or significant swelling
- Sudden worsening in movement
When infection is suspected, delaying care can increase the risk of complications and make tooth preservation less likely.
How to tell if it’s “just loose” vs an urgent dental emergency
Not every loose tooth is an emergency, but any loose tooth adult should be evaluated promptly because the cause can vary. A decision framework can help: consider the combination of mobility severity and accompanying symptoms. If mobility is new and unexplained, it’s wise to arrange urgent evaluation even if pain is minimal.
Urgency increases when symptoms suggest infection or trauma. For example, pus, fever, severe pain, or sudden swelling are strong reasons to seek urgent care right away. If the tooth loosened after an impact, same-day or next-day assessment is often recommended.
- Urgent (same day/within 24 hours): pus, fever, severe pain, visible swelling, sudden worsening, or trauma-related looseness.
- Prompt appointment (soon): new mobility without clear cause, bleeding gums, or moderate looseness that affects chewing.
- Do not wait: even “mild” looseness can reflect underlying support damage.
When in doubt, contacting an emergency dental service is safer than waiting for the problem to “settle.”
How long it takes for a loose tooth to fall out naturally in adults
Many people ask how long a loose tooth will take to fall out, but the honest answer is that there is no single timeline. A loose tooth adult may worsen over weeks, remain mobile for months, or stabilize if the cause is treated early. “Natural loss” is not guaranteed, but the risk of eventual tooth loss increases when supporting tissues continue to deteriorate.
Why there’s no fixed timeline (what determines progression)
The time it takes for a loose adult tooth to fall out depends on what’s driving the mobility. Gum disease progression, the extent of bone loss, and whether infection is present can all change the pace dramatically. Trauma-related looseness may also follow a different healing pattern depending on ligament and root involvement.
Mobility severity is another major factor. A tooth with slight wobble may be more salvageable than one with advanced movement, and early-stage support damage may be reversible or at least manageable. In contrast, advanced mobility often reflects significant attachment loss, which can lead to eventual extraction if stabilization isn’t possible.
- Cause severity: gum disease vs trauma vs infection can progress at different speeds.
- Degree of mobility: slight movement often has better odds than advanced mobility.
- Supporting tissue status: how much ligament and bone support remains.
Studies and clinical observations generally support that untreated periodontal disease tends to progress gradually, but flare-ups and infections can accelerate the timeline.
Typical progression ranges (weeks to months) and what “natural loss” implies
In many untreated cases, tooth mobility can worsen over weeks to months. Some people notice increasing looseness within a few weeks, especially if inflammation is active or an abscess develops. Others may experience slower progression over several months as bone loss continues.
However, it’s important to clarify what “natural loss” means. A tooth doesn’t always fall out on its own; it may simply become unstable and painful until it’s extracted. Your dentist may recommend extraction if the tooth cannot be stabilized safely, but the goal is often to prevent reaching that point.
- Without treatment: risk of progression increases, and eventual loss becomes more likely.
- With early treatment: stabilization may be possible, and tooth preservation may improve.
- Extraction isn’t the only outcome: some teeth can be saved with deep cleaning, splinting, or other interventions.
Because the timeline varies, the best way to estimate your situation is through an exam and imaging. Your dentist can look at bone levels and the tooth’s root support to provide a more realistic prognosis.
What to do if you’re worried about timing
If you’re concerned about how quickly things are moving, the safest approach is to seek evaluation as soon as possible. In many cases, arranging an appointment within 12–24 hours is reasonable when mobility is new, moderate, or affecting chewing—especially if there’s bleeding or discomfort. Emergency evaluation may be recommended sooner if infection symptoms are present.
During the visit, your dentist will typically perform a mobility assessment and periodontal evaluation. X-rays help determine whether the root is still supported by adequate bone and whether there are signs of infection or structural damage. These findings guide whether the tooth can be stabilized and what treatment plan is most appropriate.
- Exam + imaging: mobility testing and X-rays to assess root/bone support.
- Prognosis estimate: your dentist can explain likelihood of stabilization vs extraction.
- Action plan: deep cleaning, splinting, antibiotics (if indicated), or other options based on cause.
Even if the tooth doesn’t fall out quickly, prompt care can reduce pain, prevent infection spread, and improve the chance of preserving the tooth.
What to do right away if your adult tooth is loose (first aid until you’re seen)
While waiting for dental care, the goal is to avoid making the situation worse. Gentle protection and good hygiene can help reduce irritation and limit bacterial buildup around the tooth. These steps are not a substitute for professional treatment, but they can support your tooth until you’re evaluated.
Immediate do’s and don’ts (avoid worsening the situation)
It’s tempting to test how loose the tooth is, but repeated touching can irritate the gums and increase movement. Dental professionals generally advise against wiggling the tooth with fingers or the tongue. The more you manipulate it, the more likely you are to aggravate the periodontal ligament and surrounding tissues.
Instead, focus on protecting the tooth from stress. If you must eat, avoid chewing directly on the affected side and choose foods that require minimal force. If the tooth is painful, pain-free eating strategies become especially important until your appointment.
- Don’t wiggle or poke the tooth repeatedly.
- Don’t test mobility with the tongue or fingers.
- Do keep chewing pressure off the loose tooth.
- Do plan for urgent dental evaluation.
Safe at-home steps while waiting for an emergency dentist
Soft foods are usually the safest choice. Examples include yogurt, eggs, smoothies, soups (not too hot), mashed potatoes, and well-cooked pasta. Avoid crunchy items, sticky candies, and hard bread that can increase pressure on the tooth.
Warm saltwater rinses can help soothe irritated gums and reduce bacterial load. A typical approach is mixing salt into warm water and gently rinsing without force. Continue regular brushing and flossing carefully around the area, but avoid aggressive scrubbing directly on the loose tooth.
- Soft foods only: minimize chewing force on the affected side.
- Warm saltwater rinse: gentle rinsing to support gum comfort.
- OTC pain relief: use only as appropriate for your health needs and label directions.
If the tooth is bleeding or very tender, extra care with hygiene is important, but avoid trauma to the area. If you have severe pain, swelling, or signs of infection, prioritize urgent care over home remedies.
When to treat it as an emergency (timing rules)
Some situations require urgent evaluation immediately. If you notice pus, fever, severe pain, or visible swelling, seek emergency dental care right away. Sudden worsening of mobility—especially after an injury—also warrants prompt attention.
When symptoms are milder but the looseness is new and unexplained, scheduling within 12–24 hours when possible is a good rule of thumb. This timing helps your dentist assess the cause before additional tissue damage occurs. Your dentist may also want to rule out infection or root-related injury.
- Emergency now: pus/discharge, fever, severe pain, significant swelling, or rapid worsening.
- Urgent evaluation: new mobility without clear cause, especially if bleeding is present.
- Don’t delay: any adult tooth looseness deserves prompt assessment.
Even if the tooth doesn’t fall out quickly, early care can prevent complications and improve outcomes.
Dental treatment options for a loose permanent tooth
Dental treatment focuses on two goals: identifying the cause and stabilizing or preserving the tooth when possible. Your dentist’s plan will depend on mobility severity, gum health, bone levels, and whether infection or trauma is involved. Treatment can range from deep cleaning to splinting, and in advanced cases, surgical options or extraction with replacement.
Diagnosis first: what the dentist checks
Your dentist will typically start with a mobility assessment and a periodontal evaluation. This may include checking gum pockets, bleeding on probing, and signs of inflammation around the tooth. The goal is to understand whether the looseness is driven by gum disease, trauma, infection, or other factors.
X-rays are commonly used to evaluate the root and the surrounding bone. Imaging helps your dentist estimate the extent of bone loss and identify potential abscesses or structural issues. In some cases, additional imaging or tests may be recommended depending on symptoms.
- Mobility assessment: how much the tooth moves and how it responds.
- Periodontal evaluation: gum health, pocket depth, bleeding patterns.
- X-rays: bone support and root condition.
Once the cause is identified, your dentist can explain the most realistic prognosis and the treatment options that best match your situation.
Common treatments by cause and severity
For trauma-related looseness, your dentist may recommend stabilization (often called splinting) and monitoring healing. The tooth may need protection while the periodontal ligament recovers, and follow-up visits are important to ensure the tooth remains stable and healthy.
For gum disease or infection, the typical approach includes scaling and root planing (deep cleaning) to remove plaque and tartar below the gumline. If infection is present, antibiotics may be recommended in select cases, along with follow-up to confirm improvement. Treating the underlying inflammation is essential to give the tooth a chance to stabilize.
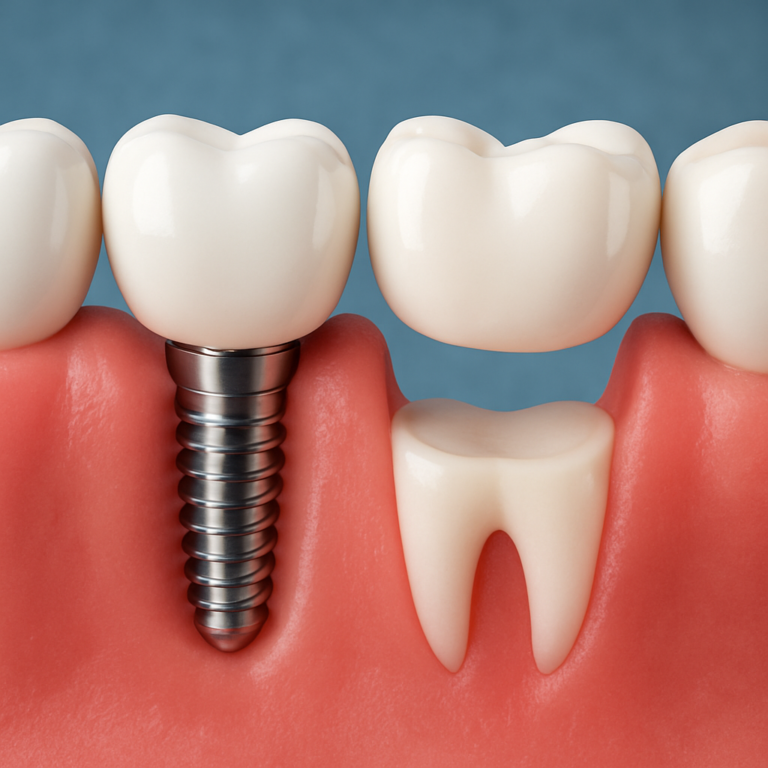
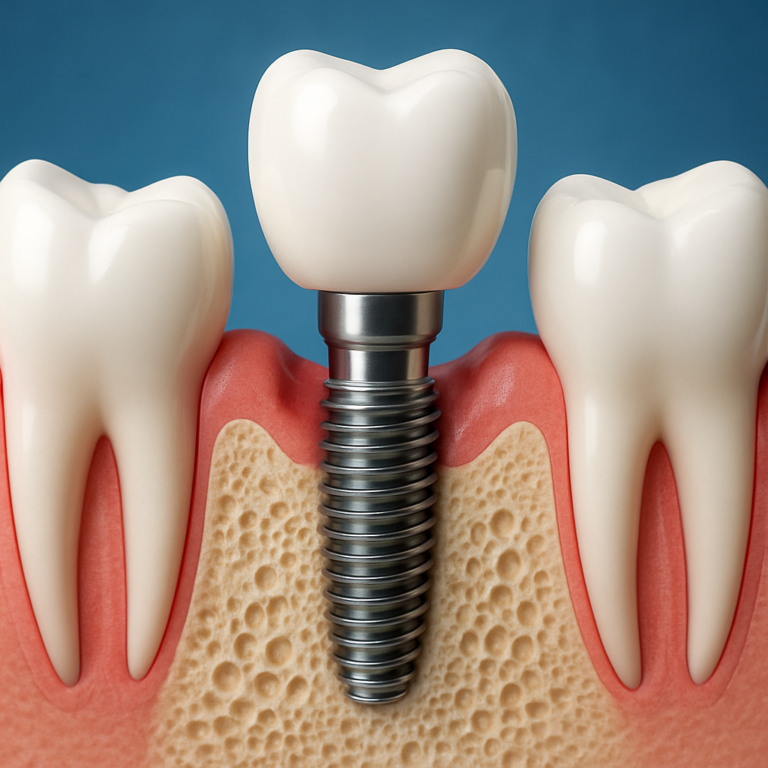
Advanced cases may require gum or bone grafting to restore support, or extraction if the tooth cannot be stabilized safely. Replacement options may include implants or bridges, depending on your overall oral health and bone availability.
- Trauma: stabilization/splinting and monitoring healing.
- Gum disease/infection: deep cleaning (scaling/root planing), possible antibiotics, follow-ups.
- Advanced support loss: grafting or extraction with replacement options.
Stabilization and supportive care (how dentists help the tooth stay)
Splinting is often used to reduce movement and allow the supporting tissues to recover. By limiting the tooth’s mobility, splints may help reduce stress on the periodontal ligament. Your dentist will determine whether splinting is appropriate based on mobility level and the underlying cause.
If bruxism is contributing, a mouthguard may be recommended. A custom or properly fitted guard can reduce grinding forces and protect both the loose tooth and the rest of your dentition. Addressing the habit is important because even successful gum treatment can be undermined by ongoing excessive pressure.
Supportive care also includes a maintenance plan. This may involve more frequent cleanings, periodontal re-evaluations, and careful home care instructions tailored to your needs. Many dentists emphasize that long-term success depends on preventing recurrence.
- Splinting: aims to limit movement and support healing.
- Mouthguard: helps reduce grinding stress when bruxism is present.
- Maintenance plan: follow-ups and hygiene routines to prevent relapse.
Prevention: how to reduce the risk of adult tooth loosening
Preventing adult tooth loosening is largely about protecting gum health and minimizing harmful forces on teeth. While some risk factors can’t be changed (like genetics or age), many common contributors are modifiable. Consistent daily habits and regular professional care are the foundation.
Daily habits that protect gums and bone
Good plaque control is the most effective way to reduce the risk of periodontal disease. Brushing twice daily with fluoride toothpaste and flossing (or using interdental cleaners) helps remove plaque where toothbrush bristles can’t reach. When plaque is controlled, inflammation is less likely to progress to deeper tissue damage.
Diet also matters. A balanced diet supports overall oral health, and adequate intake of nutrients supports tissue repair. Reducing frequent sugary snacks and acidic drinks can help protect teeth and reduce the risk of decay that can contribute to structural weakening.
- Brush twice daily: focus on the gumline.
- Floss daily: remove plaque between teeth.
- Support gum health: balanced nutrition and hydration.
If you notice bleeding when brushing, treat it as a sign to improve technique and schedule a professional evaluation rather than ignoring it.
Professional care and early intervention
Regular dental check-ups and cleanings help catch gum disease early, before mobility develops. Professional cleanings remove tartar that can’t be removed with brushing alone. Early detection also allows your dentist to monitor gum pocket depth and bone levels over time.
Prompt treatment of tooth decay is also important. Deep cavities can weaken tooth structure and increase the risk of infection, which can affect the tissues around the tooth. Treating problems early reduces the chance that inflammation spreads or that the tooth becomes unstable.
- Routine visits: catch periodontal disease before it advances.
- Deep cleaning when needed: scaling/root planing can reduce inflammation.
- Decay treatment: prevents structural weakening and infection.
For people with a history of periodontal disease, maintenance visits may be more frequent and tailored to individual risk.
Protect against trauma and grinding
Trauma prevention is especially relevant for active adults. Contact sports and high-risk activities increase the chance of impacts that can injure the periodontal ligament. Using protective gear can reduce the likelihood of tooth loosening after a hit.
For bruxism, a mouthguard can be a game-changer. If grinding is suspected, your dentist may recommend a guard to reduce tooth wear and protect supporting tissues from repeated stress. Addressing jaw tension and stress management strategies can also support long-term improvement.
- Mouthguard for bruxism: reduces grinding forces.
- Protective gear for sports: lowers trauma risk.
- Immediate evaluation after impacts: don’t wait if a tooth feels loose after a hit.
Prevention is not only about avoiding problems—it’s also about catching them early so they don’t progress to tooth loss.
Comparison: what causes loose teeth and what treatment usually follows
Because the cause of mobility determines the best treatment, it helps to understand how common triggers map to typical dental approaches. Below is a practical comparison of causes and what your dentist may recommend.
Quick cause → likely dental approach mapping
| Cause | What’s happening | Typical dental interventions |
|---|---|---|
| Gum disease (periodontitis) | Inflammation damages gums and supporting bone | Scaling & root planing (deep cleaning), periodontal maintenance; possible antibiotics if infection is present |
| Trauma (sports/falls/contact) | Ligament injury and possible root damage | Stabilization/splinting, monitoring healing; follow-up imaging |
| Bruxism (clenching/grinding) | Repeated stress increases mobility risk | Mouthguard, bite assessment, periodontal stabilization as needed |
| Osteoporosis / bone density changes | Reduced jawbone support can worsen stability | Periodontal treatment, stabilization if needed; coordination with medical care |
| Untreated decay/infection | Infection can spread to supporting tissues | Drainage or infection control (if needed), deep cleaning, antibiotics when indicated; possible endodontic or restorative care |
Prognosis factors that affect whether the tooth can be saved
Whether a tooth can be saved depends on multiple factors, not just how loose it feels. Early-stage mobility with limited bone loss generally has a better prognosis than advanced mobility with significant attachment loss. Infection presence can also reduce the chance of stabilization if it isn’t controlled quickly.
Your personal risk factors matter too. Smoking, uncontrolled diabetes, and inconsistent periodontal maintenance can worsen outcomes. Conversely, people who follow treatment and attend follow-up visits often have better long-term stability.
- Early vs advanced mobility: slight movement often responds better to treatment.
- Bone loss extent: imaging helps determine support levels.
- Infection presence: controlling infection improves stability chances.
- Patient risk factors: smoking and hygiene consistency influence healing.
Your dentist can provide a more individualized prognosis after evaluating mobility, gum health, and X-ray findings.
Cost/time expectations (high-level, non-numeric)
Timelines vary by cause and severity, but emergency stabilization may be faster than surgical options. If the tooth can be stabilized and the underlying inflammation can be controlled, treatment may involve a shorter sequence of visits. In contrast, advanced cases may require multiple appointments, healing time, and longer-term maintenance.
Follow-up visits are usually part of the overall timeline. Your dentist may re-check mobility, gum health, and symptoms after initial treatment, then adjust the plan. Ongoing maintenance is often essential to prevent recurrence and protect the rest of your teeth.
- Emergency stabilization can be quicker than grafting or complex reconstruction.
- Follow-ups are common to monitor healing and adjust treatment.
- Maintenance helps prevent the problem from returning.
Exact timing and cost depend on your diagnosis, but the best way to plan is to schedule an evaluation and ask for a clear treatment pathway.
Frequently Asked Questions
Can a loose adult tooth tighten back up on its own?
Sometimes early looseness may stabilize if the underlying cause is addressed quickly, such as treating early gum inflammation or protecting the tooth after minor trauma. However, persistent mobility usually indicates damage to supporting tissues that won’t reliably resolve without professional treatment. If an adult tooth is loose, prompt evaluation is the safest approach.
What are the most common causes of a loose tooth in adults?
The most common causes include gum disease (periodontal disease), trauma or injury, bruxism (clenching/grinding), osteoporosis or other bone-related changes, and untreated decay or infection. In many cases, more than one factor contributes, such as gum disease plus grinding. Your dentist can determine the primary driver through an exam and X-rays.
Is a loose tooth always serious in adults?
Yes—an adult loose tooth should be evaluated promptly because it often signals damage beneath the surface. While severity varies, mobility can indicate weakening of the periodontal ligament and supporting bone. Early care can reduce the risk of progression and improve the chance of saving the tooth.
What should I do if my tooth feels loose after an injury?
Avoid wiggling the tooth and stick to soft foods to minimize stress. Contact an emergency dentist as soon as possible for stabilization and assessment, especially if the looseness appeared suddenly after a hit. Immediate evaluation helps your dentist check for ligament injury or root-related damage.
How long can I wait before seeing a dentist for a loose permanent tooth?
It’s best to seek urgent evaluation within 12–24 hours when possible, especially if the looseness is new, moderate, or affecting chewing. If pain, swelling, pus, fever, or sudden worsening is present, treat it as an emergency and seek care immediately. Waiting longer increases the risk that supporting tissues will deteriorate.
What symptoms mean I might have an infection or abscess?
Infection signs can include pus or discharge, a bad taste, gum swelling or bleeding, fever, and significant pain. Some people also notice a pimple-like bump on the gum or a tooth that feels more mobile over time. These symptoms warrant immediate dental care.
Will my dentist use X-rays to evaluate a loose tooth?
Typically, yes. X-rays help your dentist assess root condition and the amount of bone support around the tooth, which is essential for determining whether stabilization is possible. Imaging also helps identify infection or other hidden causes of mobility.
Can bruxism cause adult teeth to become loose?
Yes. Chronic grinding and clenching can increase stress on teeth and supporting structures, gradually contributing to mobility—especially when combined with gum disease. A dentist may recommend a mouthguard and a plan to reduce harmful forces while treating any underlying gum inflammation.
If a loose tooth adult situation is happening now, don’t wait for it to “work itself out.” Schedule a dental consultation as soon as possible so your dentist can diagnose the cause, protect the tooth, and discuss the most appropriate next steps for your specific timeline and symptoms.