What a Hole Wisdom Tooth Means for Your Oral Health
If you’ve noticed a hole in wisdom tooth—whether it looks like a dark spot in the tooth, a gap in the gum behind your last molar, or an opening where the tooth was removed—this can be unsettling. The good news is that “holes” can have different causes, and many are treatable once the source is identified. Understanding what you’re seeing helps you know what’s normal, what needs urgent attention, and what your dentist may recommend next.
What “hole in wisdom tooth” usually means (tooth cavity vs extraction socket)
Two common scenarios: cavity in the tooth vs a healing socket in the gum
People often describe a “hole in wisdom tooth” when they can see an opening that looks deeper than expected. In reality, the same-looking “hole” can come from two very different situations: a cavity inside the tooth or a healing space after extraction.
If the wisdom tooth is still present, a “hole” is more likely to be decay—a breakdown of enamel and dentin that can form a visible pit, dark spot, or crumbling edge. If the wisdom tooth was removed recently, the “hole” is usually the extraction socket, where the roots used to be and where tissue gradually seals over time.
Because both scenarios can appear as a dark or open area, the key difference is timing and location. A cavity is on the tooth structure itself, while a socket is in the gum/bone area after removal. Your dentist may confirm the cause with an exam and an X-ray, especially if the tooth is partially erupted or impacted.
- Cavity: hole/pit on the tooth, often with sensitivity or discoloration.
- Extraction socket: opening in the gum area after surgery, typically shrinking as healing progresses.
Quick self-check: is the wisdom tooth still present?
A practical first step is determining whether the wisdom tooth is still in your mouth. If the tooth was extracted, the “hole” is almost certainly related to healing. If the tooth was not removed, the “hole” may be decay, a gum flap area, or part of the tooth’s eruption process.
Decision cues can help narrow it down. If the “hole” appeared right after a recent procedure (often within the first 1–3 days), it commonly corresponds to a socket. If the area has been developing gradually while the tooth is still erupting or partially covered by gum, it may reflect eruption-related tissue changes or a cavity forming in the tooth.
Even with a careful self-check, confirmation usually requires professional evaluation. Dental professionals rely on visual inspection plus imaging to determine whether the “hole” is decay, a trapped-gum pocket, or an empty socket.
- Recent surgery: likely extraction socket.
- Tooth still erupting/partially erupted: possible gum “hole” or decay.
- Only X-ray can confirm: whether the tooth is impacted, partially erupted, or whether decay has penetrated deeper.
Causes of a hole in a wisdom tooth (and why wisdom teeth are prone)
Why wisdom teeth develop cavities
Wisdom teeth are among the most cavity-prone teeth, largely because they sit at the very back of the mouth. Their position makes them harder to reach with a toothbrush and floss, so plaque and food particles can remain longer than they do on other teeth.
Over time, trapped bacteria produce acids that weaken enamel. As enamel breaks down, a cavity can form—a literal “hole” in the tooth structure. For many people, the first signs are subtle: a small dark spot, a rough patch, or a pit that catches the tongue.
Wisdom teeth also often erupt at an angle or partially erupt, creating tight spaces where plaque can accumulate. Studies and clinical experience consistently show that cavities are more likely when cleaning is difficult and when food debris is repeatedly trapped around the gumline.
- Hard-to-clean location: back-of-mouth access challenges.
- Food trapping: plaque builds up in grooves and around gum tissue.
- Enamel breakdown: leads to pits, discoloration, and sensitivity.
How eruption patterns create gum “holes” (operculum/flap and trapped debris)
Another common reason for a “hole in wisdom tooth” is not decay in the tooth at all, but a gum pocket created during eruption. When a wisdom tooth is partially erupted, a flap of gum tissue—often called the operculum—can cover part of the tooth crown.
This flap can trap bacteria, saliva, and food debris, creating a dark-looking area behind the last molar. The gum may look swollen or irritated, and the area can develop a bad taste or odor because the trapped space becomes a breeding ground for bacteria.
In some cases, people describe a “hole in gum where wisdom tooth is growing.” That appearance can be normal during eruption, but it can also become inflamed (sometimes called pericoronitis) if debris repeatedly collects under the flap. Whether the tooth is likely to erupt normally or remain impacted affects the long-term plan.
- Partially erupted/angled wisdom teeth: flap traps debris.
- Gum “hole” behind last molar: may look black/gray or appear as an opening.
- Inflammation risk: trapped food can lead to swelling, tenderness, and odor.
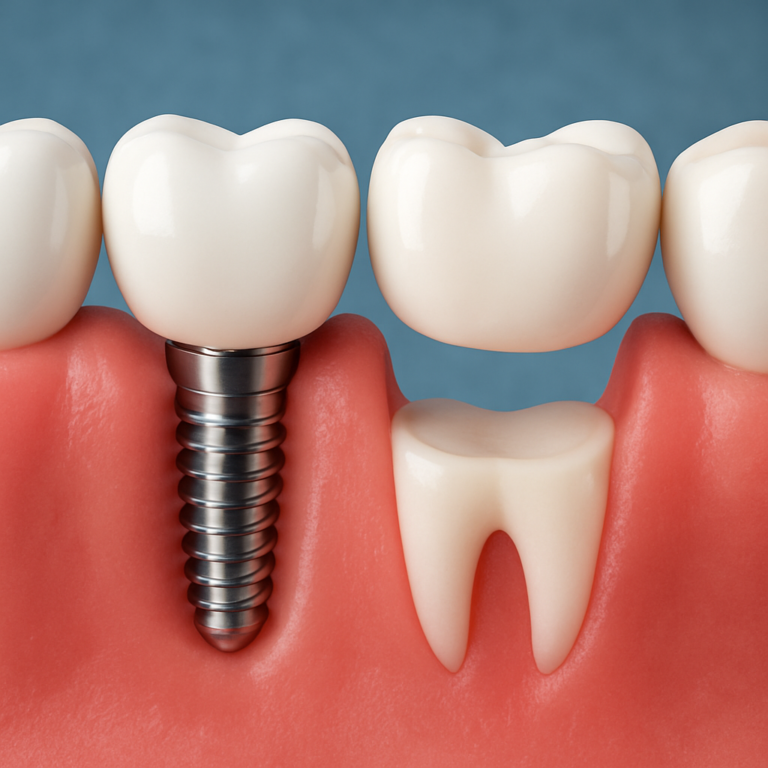
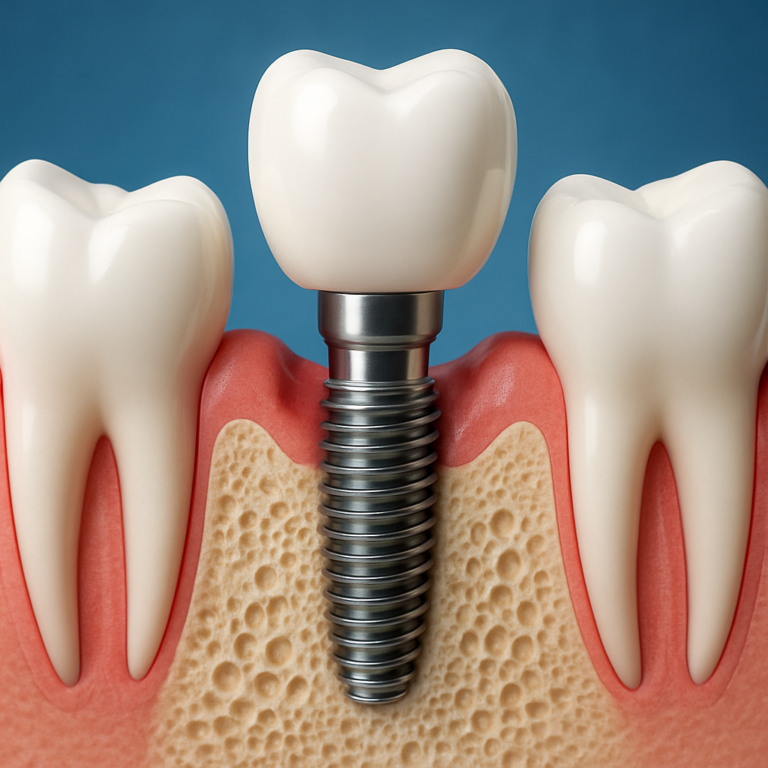
Extraction-related “hole”: what the socket is
After wisdom tooth extraction, the “hole” is typically the socket left behind in the gum and bone. Tooth roots anchor in bone, and when the tooth is removed, the body must rebuild tissue to fill the space.
In the first days, the socket may look deep and open. A blood clot forms inside the socket and acts like a protective bandage. Over time, gum tissue grows over the area, and bone gradually fills in underneath.
Impacted or partially trapped wisdom teeth can create larger sockets. If the tooth required more extensive removal, the opening can be deeper and take longer to smooth out. This is one reason two people can have very different “hole” appearances after similar procedures.
- Socket after removal: normal healing space.
- Impacted teeth: may leave larger openings.
- Healing depends on size: bigger sockets often take longer to fill.
Symptoms that help you tell cavity vs healing socket
Signs of decay in the tooth structure
A cavity in a wisdom tooth often shows up as a visible pit or discoloration on the tooth itself. People commonly notice dark brown, black, or gray spots, rough edges, or a “hole” that feels like a notch when gently touched with a clean finger or dental mirror.
Sensitivity is another clue. Wisdom tooth cavities may cause discomfort with cold drinks, sweets, or chewing, especially as decay progresses toward deeper layers. Some cavities remain painless at first, so a “hole” without pain can still be decay.
Bad taste or bad breath can also occur when bacteria collect in a cavity. If the “hole” seems to trap food and the area repeatedly smells foul, that pattern supports decay rather than normal healing.
- Visual clues: pits, dark spots, crumbling enamel edges.
- Sensitivity: cold/sweets, sometimes lingering pain.
- <strongTaste/odor: bacteria trapped in the cavity.
Signs of normal healing after wisdom tooth removal
Normal healing after extraction can look dramatic at first. In the early days, the socket may appear as a deep opening, sometimes with a whitish or yellowish film that can be part of normal healing tissue. What matters most is the overall trend: the area should gradually become less open and more comfortable.
Food may temporarily collect in the extraction site, especially during the first few days. This can happen even with good aftercare, and it’s usually manageable with gentle rinsing as your dentist advises. The key is that symptoms should improve week by week rather than worsen.
Many people notice that the gum surface looks smoother within about 1–2 weeks. Even after the gums seal, a slight depression can remain while bone fills in, which can take longer than gum healing.
- Trend matters: the hole should shrink over time.
- Early food collection: may occur but should improve.
- Comfort improves: pain typically decreases after the first few days.
Red flags that suggest complications (not normal healing)
While some discomfort is expected after extraction, certain patterns suggest complications. Persistent or worsening pain after the first few days is a major warning sign, especially if pain becomes more intense instead of gradually improving.
Swelling that doesn’t improve, fever, or a foul odor/taste can indicate infection or delayed healing. In these situations, waiting can allow the problem to worsen, so prompt evaluation is important.
Mechanical issues can also be a clue. If food repeatedly gets stuck deeply in the socket or flap area, it may reflect incomplete healing, inflammation, or a need for targeted cleaning. Similarly, if the “hole” doesn’t shrink over months, it’s worth re-checking to rule out ongoing inflammation, retained tissue, or other causes.
- Worsening pain: especially after day 3–4 post-extraction.
- Infection signs: fever, increasing swelling, foul odor/taste.
- No improvement: hole doesn’t shrink over months.
How long does a wisdom tooth “hole” take to close?
Typical timeline for gum healing vs bone healing
Healing after wisdom tooth removal often follows a two-stage pattern: gum surface healing first, then slower bone fill. For many patients, gum tissue begins to cover the opening within the first week, and by around 10–14 days the area often looks smoother.
Bone healing takes longer. Even after the gums seal, the underlying bone may continue filling in for several weeks to a few months. This can leave a small dip or depression that gradually improves as the socket remodels.
Because tooth position and extraction difficulty vary widely, timelines are averages rather than guarantees. Impacted teeth, larger sockets, and more complex surgical techniques can extend the process.
- Gum healing: often ~1–2 weeks for surface smoothing.
- Bone fill: often several weeks to 3+ months.
- What to watch: gradual shrinkage and improving comfort.
Why a hole may seem to “never close”
Sometimes the “hole” looks like it never closes because it’s larger to begin with. Impacted wisdom teeth, especially those that are partially trapped under gum tissue, can require more removal and may leave bigger sockets that take longer to fill.
Patient health can also affect healing speed. Conditions such as diabetes, anemia, or nutritional deficiencies can slow tissue repair. Smoking and vaping can reduce blood flow to healing tissues, increasing the risk of delayed healing.
In addition, some people notice a persistent opening because they’re checking too frequently or because the site is still remodeling under the surface. A follow-up exam can clarify whether the socket is healing normally or whether additional care is needed.
- Larger/impacted extractions: longer bone fill time.
- Slower healing factors: diabetes, anemia, poor nutrition.
- Smoking/vaping: can delay closure and increase complications.
Dry socket and other reasons healing stalls
Dry socket is a common complication after extraction where the protective blood clot is lost too soon. Without the clot, bone and nerve endings can become exposed, leading to significant pain that often starts a couple of days after surgery and may worsen rather than improve.
Dry socket can also make the socket appear more open than expected. It’s not just about appearance—pain pattern is the main clue. If pain becomes severe on days 2–5 post-extraction, dental professionals may suspect dry socket and provide specific treatment to relieve discomfort.
Infection can also delay healing. If bacteria enter the socket, the body may spend more time fighting inflammation, which can prolong the “hole” appearance and contribute to foul odor/taste. Prompt evaluation helps prevent complications from progressing.
- Dry socket: protective clot loss; pain often worsens after day 2–3.
- Infection: swelling, fever, foul taste/odor, delayed improvement.
- Delayed closure: may require additional cleaning or medication.
Treatment options (what your dentist/oral surgeon may recommend)
If the hole is a cavity in the wisdom tooth
Treatment depends on how deep the decay is and whether the tooth is positioned in a way that allows reliable cleaning and restoration. When decay is minimal and the tooth is accessible, your dentist may discuss options such as a filling or a crown to restore function and protect the tooth.
However, wisdom teeth often present challenges for long-term restoration. Limited access, angled or partially erupted positions, and the difficulty of keeping the area clean can increase the chance that decay returns. Many dental professionals recommend extraction when the risk of recurrence or complications is high.
Your dentist may also consider whether the cavity has affected deeper structures. If decay is close to the nerve or causing persistent symptoms, extraction may be the safer route. The goal is to prevent spread of infection and avoid future emergency pain.
- Possible restorations: filling or crown in select cases (minimal decay, favorable position).
- Extraction more likely: high risk of recurrence, poor access, or deeper decay.
- Decision is individualized: exam + X-ray guide the plan.
If the hole is a gum socket after extraction
When the “hole” is an extraction socket, the main treatment is aftercare that protects the blood clot and supports normal healing. Your dentist may recommend gentle salt-water rinses (often starting after the first 24 hours, depending on instructions), careful oral hygiene around the area, and avoiding actions that dislodge the clot.
If healing is progressing normally, no additional treatment may be needed beyond monitoring. If symptoms suggest dry socket or infection, your dentist may provide targeted interventions such as medicated dressings, prescription medication, or additional cleaning of the site.
In select cases—especially when sockets are large or when bone defects are present—your dentist may discuss advanced options like grafting. These decisions are based on clinical findings and imaging, and not every patient requires them.
- Standard aftercare: protect clot, gentle rinsing, soft foods.
- Additional care: may include cleaning/medication if infection or dry socket is suspected.
- Selective procedures: grafting may be considered in certain cases.
If the hole is from a wisdom tooth trying to erupt (gum “hole”)
A gum “hole” behind the last molar can indicate a wisdom tooth is erupting through the gingiva. Sometimes the opening looks dark or even white depending on whether enamel is visible or whether the area is covered by a flap of gum tissue.
Because eruption patterns vary, an exam and X-ray are essential to determine whether the tooth is likely to erupt normally or remain impacted. Your dentist may look at the tooth’s angle, proximity to nearby teeth, and whether there is enough space in the jaw.
Typical treatment directions include monitoring if the tooth is not impacted and symptoms are minimal. If the tooth is partially impacted, inflamed gum pockets often trap debris and can recur, so removal is more commonly recommended to prevent repeated episodes of pain and infection.
- Need for imaging: X-rays determine orientation/impaction.
- Monitoring possible: if eruption is likely and symptoms are mild.
- Removal more likely: for partially impacted teeth with recurrent flap inflammation.
When to see a dentist urgently
Pain and infection warning signs
Seek urgent dental care if pain becomes severe or worsens after the initial healing period. After wisdom tooth extraction, many people experience discomfort that gradually improves; a sudden increase in pain can signal dry socket or infection.
Fever, increasing swelling, and persistent foul odor or taste are also red flags. These symptoms suggest bacterial involvement and may require medication or procedural treatment.
Even if the “hole” looks like it’s healing, symptoms can provide the more reliable signal. If the body is fighting infection, the site may not look dramatically different at first.
- Severe/worsening pain: especially after day 3–4 post-extraction.
- Fever or increasing swelling: possible infection.
- Foul odor/taste: persistent bacterial activity.
Mechanical/functional warning signs
Mechanical problems can also indicate that something is not healing as expected. If food regularly gets stuck deeply in the socket or under the gum flap, the area may remain inflamed and harder to keep clean.
Difficulty opening the mouth (trismus) or worsening discomfort with chewing can suggest inflammation spreading beyond the immediate gum tissue. These symptoms deserve a timely evaluation to prevent complications.
In some cases, a partially erupted wisdom tooth creates a recurring “trap” that keeps re-irritating the gum. Your dentist may recommend specific cleaning strategies or removal depending on the tooth’s position.
- Food repeatedly stuck: suggests ongoing inflammation or debris trapping.
- Worsening chewing pain: may indicate spreading irritation.
- Limited mouth opening: needs prompt assessment.
“Not shrinking” timeline thresholds
Healing should show a general downward trend in symptoms and a gradual change in appearance. If the “hole” doesn’t appear to shrink over several months—or if it remains open with persistent symptoms—an evaluation is recommended even if early healing seemed normal.
For many patients, gum surface smoothing occurs within about 1–2 weeks, and bone fill continues longer. If the area remains deeply open beyond expected timelines, retained tissue, delayed bone healing, or ongoing inflammation may be factors.
Persistent symptoms should never be ignored. A re-check can include an updated exam and X-ray to confirm whether the cause is a cavity, a socket that needs additional care, or an erupting tooth that requires a different plan.
- Evaluate if no shrinkage: after several months with ongoing symptoms.
- Re-check even if early healing looked okay: complications can evolve.
- Imaging helps: confirms whether the issue is tooth-related or socket-related.
What you can do at home to support healing (and what to avoid)
Habits that can worsen a wisdom tooth hole (especially post-extraction)
Home care can make a meaningful difference, particularly after extraction. Certain habits can disturb the blood clot, irritate the area, or increase the risk of dry socket and delayed healing.
Common “avoid” items include smoking or vaping, using a straw, and vigorous rinsing or spitting. Hard or crunchy foods can also traumatize the area, especially in the first week when tissue is still fragile.
Brushing directly on the extraction site is another mistake people sometimes make. While good overall hygiene matters, your dentist’s instructions for cleaning around the site should be followed closely.
- Avoid: smoking/vaping, straw use, vigorous rinsing/spitting.
- Avoid: crunchy/hard foods and very hot/alcoholic/sugary drinks early on.
- Avoid: brushing directly on the extraction site (follow guidance).
Supportive recovery steps
Supportive recovery focuses on protecting the healing area and maintaining comfort. Warm salt-water rinses are commonly recommended, but timing and frequency should follow your dentist’s directions to avoid disrupting healing tissue.
Soft foods and hydration help reduce trauma and support tissue repair. Many patients do best with options like yogurt, soups (not too hot), mashed potatoes, eggs, and smoothies for the first few days.
Rest and balanced nutrition also matter. Healing requires energy and building blocks such as protein, vitamins, and minerals, so a steady intake can support recovery.
- Rinses: warm salt water as recommended.
- Diet: soft foods + plenty of water.
- Recovery: rest and balanced nutrition for tissue repair.
If you suspect decay while the tooth is still present
If the wisdom tooth is still in place and a “hole in wisdom tooth” appears to be decay, waiting is usually not the best strategy. Cavities can progress from enamel into deeper layers, increasing the risk of pain, infection, and more complex treatment.
Prompt dental evaluation helps determine whether a filling/crown is possible or whether extraction is safer. In the meantime, gentle hygiene around the area can reduce bacterial load without irritating the gum.
Temporary symptom management may help until the appointment, but it should not replace care. Persistent bad taste, increasing sensitivity, or visible pits are strong reasons to schedule an exam.
- Don’t wait it out: cavities can worsen.
- Gentle cleaning: keep the area clean without aggressive scraping.
- Schedule an exam: especially if pain, odor, or discoloration is present.
Prevention: how to reduce the chance of a hole in a wisdom tooth
Cleaning strategies for back-of-mouth teeth
Prevention starts with reaching the back molars effectively. Brush with attention to the last few teeth, using gentle pressure and small circular motions along the gumline where plaque tends to collect.
Interdental cleaning can also help. Flossing may be difficult for some people, but interdental brushes or a water flosser (if recommended) can improve access around the wisdom tooth area.
If a gum flap is present over a partially erupted wisdom tooth, cleaning becomes even more important. Your dentist may recommend specific techniques to reduce trapped debris under the operculum.
- Brush technique: focus on the gumline and last molars.
- Interdental tools: floss, interdental brushes, or water flosser if advised.
- Consistency: daily cleaning reduces plaque buildup over time.
Diet and lifestyle factors that increase cavity risk
Diet influences cavity risk because frequent sugar exposure feeds cavity-causing bacteria. Reducing frequent snacking and limiting sugary or acidic drinks can lower the number of acid attacks on enamel.
Dry mouth increases risk as well. Saliva helps neutralize acids and wash away food particles, so managing dry mouth—through hydration, addressing medications with your clinician, and avoiding tobacco—is beneficial.
Tobacco and heavy alcohol use are linked to worse oral health outcomes, including higher inflammation and delayed healing. Lifestyle changes can support both cavity prevention and recovery if a wisdom tooth issue has already started.
- Reduce snacking: fewer sugar/acid exposures.
- Manage dry mouth: hydration and clinician guidance if needed.
- Avoid tobacco: supports healthier gums and healing.
Monitoring eruption and getting X-rays early
If a gum “hole” appears behind the last molar, early evaluation can prevent repeated flare-ups. A small gum opening can be part of normal eruption, but it can also signal a partially impacted tooth that traps debris.
X-rays determine tooth orientation and whether the wisdom tooth is impacted, partially impacted, or likely to erupt normally. Without imaging, it’s difficult to predict whether the gum flap will keep causing problems.
Early monitoring also helps dentists plan preventive care. Depending on findings, your dentist may recommend cleaning strategies, periodic checks, or removal to prevent cavities and gum inflammation.
- Evaluate new gum holes: especially if they appear behind the last molar.
- Use X-rays: confirms impaction and guides next steps.
- Plan early: monitoring vs removal depends on risk.
Comparison: cavity vs extraction socket vs erupting wisdom tooth gum hole
Side-by-side differences (appearance, timing, typical symptoms)
Because a “hole in wisdom tooth” can look similar at first glance, comparing key features can help. The biggest differentiators are whether the tooth is still present, whether the area appeared after extraction, and whether symptoms match decay or healing.
The table below summarizes common differences. Individual cases vary, so the safest approach is still an exam and X-ray when the cause is unclear.
| Scenario | Where the “hole” is | Typical timing | Common symptoms |
|---|---|---|---|
| Cavity | On the tooth structure (pit/pocket) | Develops over time | Sensitivity, dark spot, persistent bad taste/breath |
| Extraction socket | In gum/bone where tooth was removed | Immediately after surgery | Pain that improves, gradual shrinkage; clot protection early |
| Erupting tooth gum hole | Behind last molar; may involve flap/operculum | As tooth erupts (can be gradual) | Swelling/tenderness, food trapping under flap, odor if inflamed |
Matching the scenario to likely next steps
Once the likely cause is identified, the next steps become clearer. A cavity typically requires an exam to determine whether restoration is feasible or whether extraction is safer due to access and recurrence risk.
A socket after extraction usually follows a predictable healing timeline. The focus is aftercare and monitoring for red flags like dry socket or infection, especially if pain worsens after the first few days.
A gum “hole” from eruption often requires imaging to determine impaction. If the tooth is partially impacted and repeatedly traps debris, removal may be recommended to prevent ongoing inflammation and discomfort.
- Cavity → exam for filling/crown vs extraction decision.
- Socket → aftercare + watch for dry socket/infection signs.
- Eruption gum hole → X-ray to determine impacted vs not impacted; monitor vs remove.
Frequently Asked Questions
Is it normal to have a hole where my wisdom tooth was removed?
Yes. An extraction socket can look deep at first, and the body typically seals the area with gum tissue over the following weeks. Gum healing often improves within about 1–2 weeks, while bone fill can take longer.
If pain worsens after the first few days, swelling increases, or there is persistent foul odor/taste, contact your dentist promptly to rule out dry socket or infection.
How long does it take for a wisdom tooth hole to close?
Gum surface smoothing often occurs within roughly 1–2 weeks. Bone healing can take several weeks to a few months even after the gums appear to have covered the area.
Healing speed varies based on extraction difficulty, socket size, and health factors like diabetes control and smoking status.
What does a hole in the gum where a wisdom tooth is growing mean?
A hole in the gum where a wisdom tooth is growing often means the tooth is erupting through the gingiva. It can also reflect a flap (operculum) that traps debris, especially if the wisdom tooth is partially impacted.
An exam and X-ray help determine whether monitoring is appropriate or whether removal is needed to prevent recurring inflammation.
Can a wisdom tooth cavity be filled instead of extracted?
Sometimes, a wisdom tooth cavity can be treated with a filling or crown if decay is limited and the tooth is favorably positioned. Many cases still require extraction because wisdom teeth are difficult to clean and restorations may not hold up well long-term.
Your dentist can recommend the safest option based on the depth of decay, access, and risk of recurrence.
What are the signs of dry socket?
Dry socket often causes significant pain that commonly worsens after the first few days rather than improving. The socket may look more open than expected, and discomfort can be intense enough to affect sleep and eating.
Dry socket is treatable, so dental professionals recommend contacting your dentist if pain follows this pattern.
Why does my wisdom tooth hole smell bad or taste foul?
Bad smell or foul taste can occur when bacteria accumulate in a cavity, an inflamed gum flap, or an extraction socket. In extraction sites, infection or dry socket can also contribute to persistent odor.
If the odor/taste persists or is accompanied by worsening pain or swelling, schedule an evaluation.
When should I call my dentist about a wisdom tooth hole?
Call your dentist if pain worsens after the first few days, if swelling increases, or if fever occurs. Also contact your dentist if foul odor/taste persists, food repeatedly gets stuck deeply, or the hole doesn’t appear to shrink over several months.
Early assessment can prevent minor issues from becoming more complicated.
Will a decayed wisdom tooth eventually fall out on its own?
A decayed wisdom tooth may loosen over time, but waiting is generally not recommended. Decay can spread, leading to infection, fracture, and complications involving surrounding gum and bone.
Dental professionals typically recommend evaluation and treatment to protect overall oral health.
If a hole in wisdom tooth is present—or if a gum opening behind the last molar is new—scheduling a consultation is the most reliable next step. A dentist can examine the area, take an X-ray if needed, and recommend the safest plan for healing, cavity control, or wisdom tooth management. Our team at Smile Avenue Family Dentistry can help you sort out what you’re seeing and move forward with confidence.