What Is a Fake Tooth Called?
Losing a tooth can feel shocking—especially when you’re trying to figure out what a fake tooth is called and what options actually work for chewing, speech, and long-term oral health. In dentistry, the “right” name matters because it often points to the device type, how long it lasts, and what to expect during treatment.
What Is a “Fake Tooth” Called? (Common Names and Dental Terms)
The most common term: “dental prosthesis” (and “false tooth”)
In everyday conversation, people often say fake tooth to mean any replacement for a missing tooth. In dental offices, clinicians more commonly use terms like dental prosthesis, prosthetic tooth, or replacement tooth to describe the specific appliance or restoration.
These terms can sound interchangeable, but they’re not always exact matches. A false tooth is a broad, lay description that may refer to the visible part that replaces the missing tooth (for example, the crown portion of an implant restoration or the “pontic” in a bridge). A prosthetic tooth usually refers to the artificial tooth as part of a larger prosthesis (such as a denture or partial). A replacement tooth is a general phrase that can include both fixed and removable solutions.
Your dentist may also describe the restoration by its function and attachment method. For example, an implant-supported crown is a fixed prosthesis that sits on an abutment, while a flipper is a removable interim prosthesis designed to improve appearance and basic function while waiting for definitive treatment.
- Dental prosthesis: the umbrella term for artificial tooth replacement devices.
- Prosthetic tooth: the artificial tooth component within a prosthesis.
- False tooth: commonly used by patients; may refer to the visible replacement portion.
- Replacement tooth: general wording for any tooth substitute.
Fixed vs removable: how the name changes by device type
One of the biggest reasons the wording varies is that dental professionals categorize replacements by whether they stay in place. Fixed options are designed to remain in the mouth and are not removed by the patient, while removable options can be taken out for cleaning.
Fixed replacements typically include dental implants (with a crown), crowns, and bridges. A bridge is cemented in place, and an implant crown is attached to an abutment that connects to the implant placed in the jawbone. Because these options are stable, they usually support more natural chewing and a more seamless feel.
Removable replacements include flippers, partial dentures, complete dentures, and certain retainers that incorporate a “fake tooth.” These devices often rely on gums and/or clasps for support, which can make them less stable than fixed solutions. Many removable options are intended for interim use or for patients who prefer a non-surgical pathway.
- Fixed: implant crowns, traditional bridges, resin-bonded bridges (stays in place).
- Removable: flippers, partial dentures, dentures, Essix-style retainers (comes out for cleaning).
Temporary vs permanent: why the wording matters
Another key naming difference is whether the prosthesis is intended to be temporary or long-term. When a dentist says “temporary,” the expectation is that the device supports you while healing occurs or while a final restoration is being fabricated.
Temporary options can include flippers and immediate temporary crowns placed right after extraction. These are often designed to restore appearance quickly and help with basic function, but they may not be ideal for heavy chewing. Long-term options include implant crowns, bridges, and dentures, which are selected based on your bite, remaining teeth, bone levels, and long-term goals.
Because timelines affect comfort and expectations, it helps to ask what category your replacement falls into. For example, a temporary crown may be replaced within weeks to a few months, while a definitive implant crown is typically planned for many years of service with proper care.
- Temporary: flipper or immediate temporary crown; supports appearance/function during healing.
- Permanent (definitive): implant crown, bridge, or denture; designed for long-term replacement.
Why People Need a Fake Tooth (Common Causes of Tooth Loss)
Missing teeth from decay, injury, or extraction
Tooth loss is often the result of problems that weaken or damage the tooth beyond what restorative materials can fix. Common causes include cavities (tooth decay), trauma (sports injuries, falls), and periodontal disease, which can loosen teeth over time.
In many cases, the missing tooth is not just one isolated issue. Your dentist may explain that tooth loss can be single-tooth or multiple-tooth, and the replacement plan often depends on how many teeth are missing and what remains around the gap.
When a tooth is extracted, the body begins to change in the area where the tooth used to be. Over months and years, the jawbone can lose some of its volume without stimulation from a tooth root, which is one reason timely replacement is often recommended.
- Decay: cavities that reach deep layers may require extraction.
- Injury: fractures can make the tooth non-restorable.
- Periodontal disease: bone loss can lead to mobility and eventual tooth loss.
Damaged teeth that can’t be restored
Sometimes a tooth is damaged in a way that makes fillings or even crowns unlikely to succeed. If the tooth is too broken, too weak, or has extensive structural loss, dental professionals may recommend extraction to protect surrounding tissues and prevent ongoing pain or infection.
In other situations, a tooth may be salvageable initially but still requires removal if the prognosis is poor. Your dentist may evaluate the tooth’s remaining structure, the health of the gums, and the presence of infection before recommending a replacement tooth plan.
In many cases, the replacement process begins after the extraction site is evaluated. Depending on the timeline and your goals, your dentist may offer a temporary solution first and then move to a definitive option such as an implant crown or bridge.
- When the tooth is too fractured for a predictable restoration, extraction may be necessary.
- Replacement planning may start immediately with a temporary “fake tooth” while healing occurs.
- Definitive options depend on bone and adjacent tooth health.
Cosmetic concerns after tooth loss
Tooth loss affects more than chewing—it can change how your smile looks and how confident you feel. Many people notice gaps when talking or laughing, and some feel self-conscious about “showing” missing teeth.
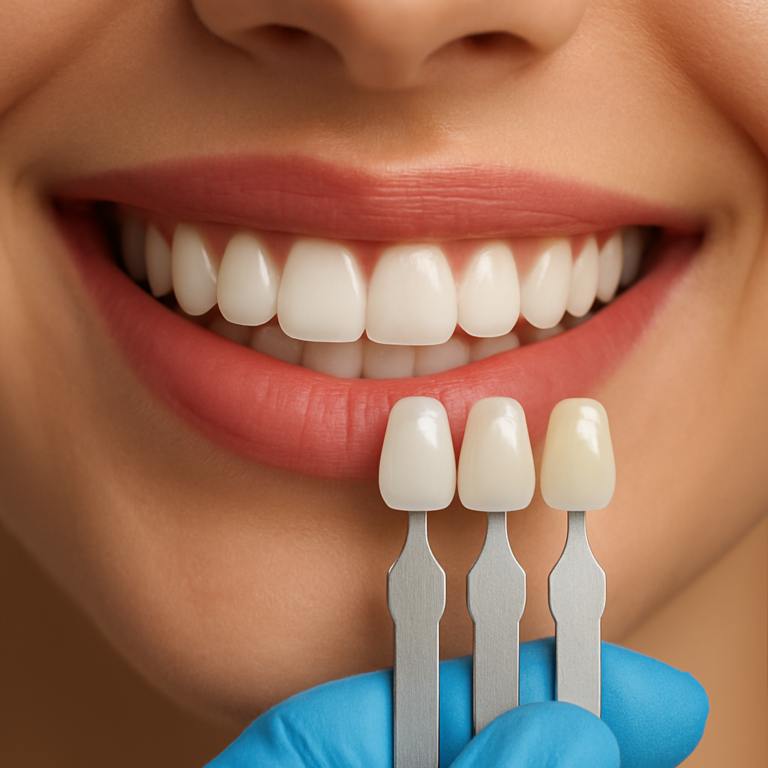
Cosmetic concerns can be especially noticeable when the missing tooth is in the front. In these cases, the goal is often to match the color, shape, and contour of surrounding teeth while also supporting proper bite mechanics.
It’s also important to balance appearance with function. A replacement can be designed to look natural, but your dentist may still emphasize that long-term oral health depends on choosing an option that fits your bite and helps reduce shifting and bone loss.
- Appearance impact: gaps can be visible during speech and smiling.
- Confidence: many patients report reduced social comfort after tooth loss.
- Functional expectations: “show tooth” solutions may not provide full chewing strength.
Signs You May Need a Replacement Tooth (Symptoms and Impacts)
Functional changes: chewing and speech
When a tooth is missing, chewing efficiency often drops. Even if the gap is small, your bite may shift slightly, causing you to chew on one side or avoid certain foods.
Speech can also change, particularly when the missing tooth is near the front. Some people notice altered pronunciation of certain sounds, or they may feel tongue movement changes when talking.
These functional changes can become more noticeable over time. If the missing tooth is in a high-impact area of your bite, your dentist may recommend replacement sooner to help prevent compensatory habits that strain other teeth.
- Chewing: reduced efficiency and altered bite mechanics.
- Speech: pronunciation changes, especially with front teeth.
- Compensation: chewing patterns may shift, affecting comfort elsewhere.
Oral health effects: shifting, bite changes, and bone loss
Tooth loss can set off a chain reaction in the mouth. Adjacent teeth may drift toward the gap, and opposing teeth may over-erupt into the empty space, which can complicate future bite alignment.
Bone loss is another major factor. Without stimulation from a tooth root, the jawbone can resorb over time—studies suggest that bone volume can decrease noticeably within the first year after extraction. This matters for implant planning because implants rely on sufficient bone to support the artificial root.
Replacing a missing tooth can help slow or prevent some of these changes. While bridges and dentures can restore function and appearance, implants are specifically designed to replace the root portion and may offer better support for preserving jawbone volume when conditions allow.
- Shifting: neighboring teeth may move into the gap.
- Bite changes: opposing teeth can shift or over-erupt.
- Bone resorption: jawbone volume can decrease after tooth loss, affecting implant eligibility.
Comfort and daily-life impacts
Removable options can come with day-to-day challenges. Some people find that food traps under removable appliances, especially during meals, which can lead to extra cleaning steps and occasional discomfort.
Comfort and stability vary by device. A flipper or partial may feel bulky at first, and dentures require learning how to seat them properly for better comfort and speech.
Beyond physical comfort, many patients experience embarrassment or social discomfort. If the replacement is temporary, it may be removed during eating, which can feel awkward in public settings.
- Food trapping: more common with removable appliances.
- Speech/comfort: may require adaptation time.
- Social discomfort: some people feel self-conscious about removing a device.
Treatment Options: Top Fake Tooth Choices for Replacing Missing Teeth
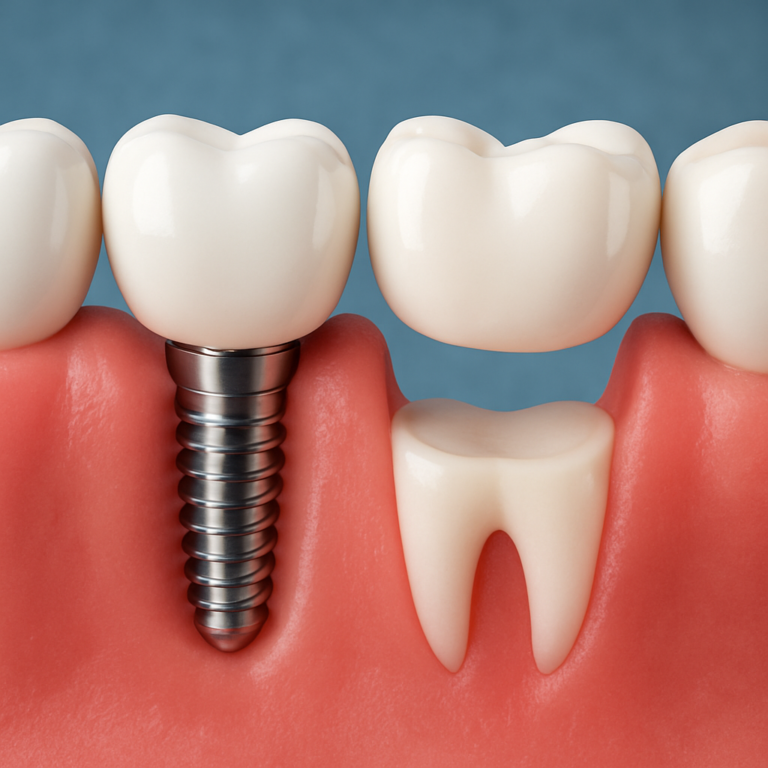
Dental implants (implant post + abutment + crown)
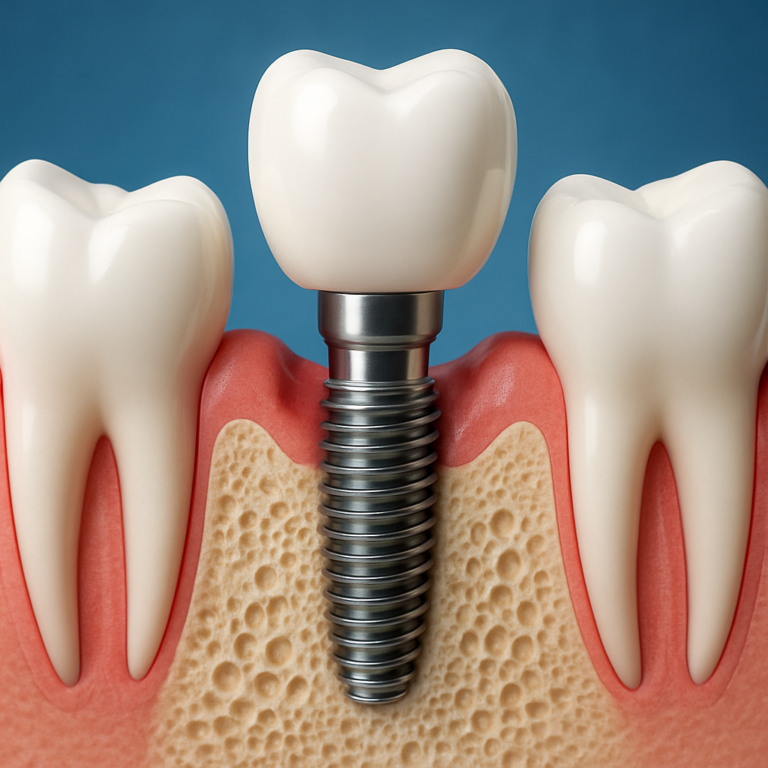
Dental implants are often considered the most “tooth-like” replacement because they replace both the root and the visible crown. The system typically includes an implant post placed into the jawbone, an abutment that connects the post to the crown, and a custom-made crown that looks like a natural tooth.
The implant post acts like an artificial root. Over time, the bone integrates with the implant surface in a process called osseointegration. The crown is then fabricated to match your tooth color and shape, helping restore appearance and bite function.
Implants may be a strong option for many patients, but suitability depends on health and bone availability. Your dentist may discuss factors such as gum health, smoking status, and whether a bone graft is needed to create enough support for the implant.
- Pros: natural feel, strong chewing function, and potential support for jawbone preservation.
- Cons: higher upfront cost, surgery and healing time, and possible bone grafting.
Recovery and timeline can vary widely. Many implant pathways involve several months from placement to crown delivery, especially when bone grafting is required or when healing needs to be carefully monitored.
Dental bridges (fixed bridges and resin-bonded/Maryland bridges)
Dental bridges replace one or more missing teeth by anchoring a false tooth (pontic) to crowns on adjacent teeth. In a traditional bridge, the neighboring teeth are prepared and fitted with crowns that hold the pontic in place.
Resin-bonded bridges (often called Maryland bridges) attach the pontic using a conservative bonding approach. These are frequently used for certain front-tooth situations where the bite forces are lower and the neighboring teeth can provide stable support.
Bridges can be a good choice when you want a fixed solution without implant surgery. However, they do require altering the adjacent teeth in most cases, and they do not replace the tooth root—so they may not prevent bone loss at the gap in the same way an implant can.
- Traditional bridges: crowns on adjacent teeth + pontic; fixed and stable.
- Resin-bonded/Maryland: conservative attachment; often used for front teeth.
- Pros: faster than implants for many patients, fixed feel, good esthetics.
- Limitations: may require prep of neighbors; does not preserve bone at the missing site.
Removable “fake tooth” options (flippers, partial dentures, dentures, Essix retainers)
Removable options are commonly used when speed, affordability, or interim support is the priority. These can include flippers (interim partials), removable partial dentures, complete dentures, and certain retainers that incorporate a false tooth, such as an Essix retainer.
A flipper typically replaces a single missing tooth temporarily. It may be designed to be worn continuously for appearance and basic function, but patients are usually advised to avoid heavy chewing with the flipper’s artificial tooth.
Removable partial dentures can replace multiple teeth and may include clasps or metal components for retention. Complete dentures replace all teeth in an arch and require a learning period for comfort, speech, and chewing.
Essix retainers with a false tooth are often used for quick turnaround, sometimes within a day or a few days, depending on the situation. They’re usually intended as a temporary solution and are removed for eating and cleaning.
- Flippers/interim partials: single-tooth temporary replacement; limited chewing strength.
- Removable partial dentures: multiple teeth; may include clasps/metal; bulkier.
- Dentures: full arch replacement; require adaptation and regular maintenance.
- Essix retainer: temporary “retainer with a fake tooth,” often for fast turnaround.
Removable options can be practical, but they come with trade-offs. Stability may be less than fixed restorations, speech may take time to adjust, and food can sometimes get trapped underneath—especially if cleaning routines are inconsistent.
- Pros: affordability and speed.
- Top limitations: less stability, possible speech/comfort issues, maintenance needs, and limited longevity.
Temporary Fake Tooth Solutions (When You Need Something Now)
Flippers and immediate temporary crowns: what to expect
Temporary solutions are designed to bridge the gap between tooth loss and definitive treatment. A flipper is commonly used right after extraction or while waiting for a final crown, bridge, or implant restoration.
Immediate temporary crowns may also be placed in select cases, particularly when a tooth is extracted and a final restoration is planned soon. These temporary teeth help protect the appearance of your smile and can support basic function while healing takes place.
It’s important to understand limitations. Temporary teeth are typically not meant for heavy chewing, and they may feel less secure than the final restoration. Your dentist may recommend softer foods and careful bite habits during the interim period.
- Use cases: right after extraction, or while waiting for final restoration.
- Expect: cosmetic and basic functional support, not maximum durability.
- Care: follow instructions closely to avoid irritation and damage.
DIY temporary kits and at-home “snap-in” teeth (Temptooth-style products)
Some products marketed as at-home “snap-in” teeth claim to provide quick cosmetic coverage. These kits may include heat-and-mold materials or removable appliances designed to fit over existing teeth.
While the idea of a fast solution is understandable, the fit and safety can vary significantly. A poor fit can rub gums, cause irritation, or create pressure points that worsen discomfort. More importantly, DIY products may mask underlying issues that a dental exam would catch—such as gum inflammation, infection, or bone loss.
Dental professionals generally recommend avoiding DIY temporary teeth when there is pain, swelling, or signs of infection. If a product doesn’t fit properly, it can lead to sores and may delay proper treatment.
- Quality concerns: fit may be inconsistent without clinical assessment.
- Health concerns: irritation risk and missed diagnosis of gum/bone issues.
- When to avoid: if there is pain, bleeding, swelling, or recent extraction complications.
How long temporary options last and what happens next
Temporary options are typically measured in weeks to a few months, depending on the definitive plan. For example, a flipper may be used until a final bridge is ready, while an immediate temporary crown may be worn during healing before the definitive restoration is placed.
In implant cases, the timeline often includes multiple stages. Healing and osseointegration can take weeks to months, and the final crown is usually placed after the implant is stable and the gums have healed appropriately.
Temporary teeth do not replace definitive treatment for long-term outcomes. Even if they look good, they may not provide the same bite stability, durability, or long-term oral health benefits as a properly planned implant crown, bridge, or denture.
- Temporary-to-final: often weeks to months, based on healing and lab fabrication.
- Why it matters: temporary devices support you now, but definitive treatment protects long-term function.
The Dental Implant Process (Step-by-Step, From Exam to Crown)
Consultation, imaging, and eligibility checks
The implant process usually begins with a thorough evaluation. Your dentist will review medical history and perform an oral exam to assess gum health, remaining teeth, and the specific area of missing tooth.
Imaging is a key part of planning. X-rays and often 3D imaging help evaluate bone density, bone volume, and the position of important structures. This information guides decisions about implant placement and whether a bone graft is needed.
Eligibility checks also consider lifestyle factors. Smoking and uncontrolled periodontal disease can affect healing, and certain health conditions may require coordination with a physician.
- Exam + imaging: X-rays/3D scans to map bone and anatomy.
- Health checks: gum status, smoking, and medical conditions.
- Plan discussion: timeline, comfort expectations, and whether grafting is recommended.
Surgery and healing: osseointegration explained
Implant surgery places the implant post into the jawbone. The procedure is typically performed with local anesthesia, and many patients also receive sedation depending on complexity and comfort needs.
After placement, the implant must integrate with the bone through osseointegration. This healing phase can take several weeks to months, and the exact duration depends on bone quality, whether a bone graft was performed, and how well healing progresses.
During recovery, mild soreness is common. Many patients find that discomfort peaks within the first 24–72 hours and then gradually improves; however, your dentist may recommend specific pain management and aftercare steps.
- Placement: implant post into jawbone.
- Healing: osseointegration over weeks to months.
- Possible grafting: if bone volume is insufficient.
Abutment and crown placement (final “fake tooth”)
Once the implant has healed and is stable, an abutment is attached. The abutment connects the implant post to the crown and helps shape the final emergence profile of the tooth.
The crown is then custom-made to match your smile. Your dentist may take digital scans or impressions so the lab can fabricate a crown that fits properly and matches color and shape. This is where the “natural-looking” goal becomes very real—especially for visible front teeth.
After placement, your dentist will check bite alignment and may adjust the crown to ensure comfortable chewing. With good home care and regular cleanings, implant crowns can last many years.
- Abutment: connector between implant and crown.
- Custom crown: color/shape matching for a natural appearance.
- Aftercare: hygiene and follow-up visits to protect long-term success.
How to Choose the Best Fake Tooth Option (Decision Framework)
Match the option to your situation (single tooth vs multiple teeth vs full arch)
The best choice depends heavily on how many teeth are missing and where the gap is located. A single missing tooth may be treated with an implant crown, a bridge, or an interim removable option like a flipper or Essix retainer.
When multiple teeth are missing, the plan may shift toward implant-supported bridges, implant-supported dentures, or removable partial dentures. The goal is to restore function while balancing stability, cost, and the health of remaining teeth.
For full-arch tooth loss, options may include conventional dentures or implant-supported solutions. Implant-supported approaches can improve stability for many patients, but the right plan depends on bone availability and overall health.
- Single tooth: flipper/Essix (temporary), bridge (fixed), or implant crown (long-term).
- Multiple teeth: implant-supported bridges/dentures or removable partials.
- Full arch: conventional dentures or implant-supported overdentures.
Compare based on bone, adjacent teeth, and bite requirements
Bone availability is a major factor for implant candidacy. If bone volume is limited, your dentist may recommend a bone graft before or during implant placement to support the artificial root.
Bridges depend on the health of adjacent teeth. If neighboring teeth are weak or have extensive decay, a bridge may not be ideal. Your dentist may also consider whether the bite forces in that area are suitable for a bridge design.
Bite requirements vary by location. Back teeth experience higher chewing forces, so your dentist may recommend stronger, more durable solutions for molar gaps compared with some front-tooth scenarios.
- Implants: need enough bone or may require grafting.
- Bridges: require healthy neighboring teeth for support.
- Bite forces: back teeth often need more robust restoration planning.
Compare based on cost, timeline, and maintenance
Cost and timeline often drive decision-making, but maintenance requirements are just as important. Removable options are usually less expensive upfront, while implants typically have the highest initial cost due to surgery and multi-stage treatment.
Timeline can also differ. Some bridges and removable options can be completed in a matter of weeks, while implant pathways may take several months depending on healing and whether grafting is needed.
Maintenance varies by option. Removable devices may need relines or replacement as gums and bone change, while fixed restorations require consistent oral hygiene and professional cleanings to protect the supporting teeth or implant.
- Upfront cost: removable usually lowest; bridges mid-range; implants highest.
- Timeline: quick cosmetic fixes vs multi-month implant pathway.
- Maintenance: cleaning routines, possible adjustments, and replacement likelihood.
Costs, Insurance, and Financing for Fake Tooth Replacement
Typical cost ranges by option (high-level, non-numeric or “relative”)
Costs vary widely based on location, complexity, and the number of teeth involved. As a general rule, removable options tend to be the least expensive upfront, while bridges are often mid-range, and implants are usually the highest upfront investment.
These differences reflect materials, lab work, and the complexity of treatment. Implant treatment includes surgical placement and staged healing, while bridges require dental lab fabrication and preparation of supporting teeth.
Your dentist can provide a personalized estimate after evaluation. It’s also helpful to ask what’s included in the quote, such as imaging, temporary solutions, and follow-up visits.
- Removable: usually lowest upfront cost.
- Bridges: mid-range cost for fixed replacement.
- Implants: highest upfront cost due to surgery and multi-stage care.
Insurance coverage patterns and what to ask
Insurance coverage can be unpredictable. Some plans cover portions of bridges or dentures more readily than implants, while others may have annual maximums or coverage limitations that affect your out-of-pocket cost.
To avoid surprises, ask your dental team to break down the total cost and explain which parts are likely covered. Coverage may differ for diagnostic imaging, temporary restorations, lab fees, and follow-up appointments.
Important questions include whether bone grafting is covered if needed, and whether temporary-to-final costs are included in the estimate. Your dentist’s office can often help coordinate benefits and provide documentation.
- Ask what’s covered for bridges/dentures vs implants under your plan.
- Request a total estimate including follow-ups, lab fees, and any grafting.
- Clarify whether temporary solutions are included in the overall cost.
Payment plans and affordability strategies
Many dental practices offer payment options to make treatment more manageable. In-office financing or third-party plans can spread costs over time, which may help when definitive replacement is needed but budget is tight.
Affordability strategies often involve prioritizing the most urgent steps. For example, if appearance is a concern immediately after extraction, a temporary flipper or immediate temporary crown may be used while definitive planning continues.
Your dentist can also help sequence treatment to match your timeline and financial comfort. In some cases, addressing gum health first can improve long-term outcomes and reduce the likelihood of complications.
- Financing: in-office plans or third-party financing options.
- Sequencing: temporary solutions first if urgency requires it.
- Long-term value: consider durability and maintenance costs, not just the initial price.
Risks, Downsides, and Complications (What to Know Before You Choose)
Common downsides by category
Every replacement option has trade-offs. Understanding the potential downsides helps you make a decision that fits your health, lifestyle, and expectations.
For implants, the main downsides include surgery, healing time, and the possibility of bone grafting if bone volume is insufficient. While implant success rates are generally high in appropriate candidates, your dentist may still discuss risks such as infection or delayed healing.
For bridges, a common limitation is that adjacent teeth may need preparation. Bridges also do not replace the root, so they may not prevent bone loss at the gap. Over time, bridges may require replacement as supporting teeth change.
For removable options, stability and comfort can be challenges. Removable devices may affect speech, trap food, and require relines or replacement as your mouth changes.
- Implants: surgery risk, healing time, possible bone grafting.
- Bridges: may require altering neighbors; no root replacement; potential future complications.
- Removables: less stable, food trapping, speech/comfort issues, repeated replacement.
When DIY or temporary “snap-in” teeth may be a bad idea
DIY temporary kits can seem convenient, but they may create more problems than they solve. A poor fit can irritate gums and make it harder to detect inflammation or infection.
Another risk is that DIY products can delay proper diagnosis. If the missing tooth area has underlying gum disease, bone loss, or an infection, a snap-in appliance may hide symptoms rather than address the cause.
If pain, swelling, or bleeding is present, professional evaluation is important. Dental professionals can determine whether the issue is simply cosmetic or whether urgent treatment is needed.
- Poor fit: irritation and pressure sores can develop.
- Masked problems: underlying gum/bone issues may be missed.
- Clinical assessment: needed to confirm healing and plan definitive care.
How to reduce risk with proper dental care
Risk reduction starts with consistent oral hygiene and follow-up visits. Your dentist may recommend specific cleaning techniques based on your option, such as flossing strategies for bridges or careful cleaning around implant-supported crowns.
For long-term success, lifestyle factors matter. Smoking can impair healing and worsen gum health, which can affect both implants and the health of supporting teeth for bridges.
Regular checkups also allow early detection of issues like loosening, gum inflammation, or bite changes. Addressing small problems early can prevent bigger complications later.
- Follow-ups: attend scheduled visits for monitoring and adjustments.
- Hygiene: brush and clean around the restoration as instructed.
- Periodontal management: keep gum disease under control for better outcomes.
Prevention and Long-Term Care (Make Your Replacement Tooth Last)
Daily care routines for each option
Long-term success depends on daily maintenance. For implant crowns and fixed restorations, brushing twice daily and cleaning between teeth are essential to protect gum health and prevent inflammation around the restoration.
Bridges require careful cleaning under the pontic. Flossing or using interdental brushes can help remove plaque from areas that are harder to reach, which reduces the risk of gum irritation and supporting tooth decay.
Removable devices require a different routine. Flippers, partial dentures, and dentures should be removed for cleaning and stored properly when not in use. Many dentists recommend soaking and brushing with products designed for dentures to reduce odor and buildup.
- Implants/crowns: brush around the implant area; floss carefully; schedule professional cleanings.
- Bridges: clean under the pontic; use floss/threaders or interdental tools as advised.
- Removables: remove daily; clean and soak as instructed; rinse after meals.
Lifestyle factors that affect longevity
Some habits can shorten the life of restorations. Smoking is a major risk factor because it can reduce blood flow to gums and impair healing, which may affect both implants and the health of supporting teeth.
Diet also plays a role. Hard foods can increase the risk of chipping or loosening, especially for temporary or less stable devices. Grinding or clenching can add stress to crowns and bridges, leading to wear or fracture over time.
Your dentist may recommend a night guard if bruxism (teeth grinding) is present. Protecting your bite can extend the lifespan of your replacement tooth and reduce discomfort.
- Smoking: harms gum health and healing.
- Hard foods: increase risk of damage.
- Grinding/clenching: may require a night guard to protect restorations.
Regular checkups and “replacement planning”
Even durable restorations need monitoring. Your dentist may recommend checkups every 3–6 months initially after treatment, then typically every 6–12 months once stable, depending on your oral health.
Checkups help track gum health, bite alignment, and the condition of the restoration. For removable appliances, periodic adjustments or relines may be needed as tissues change.
Replacement planning means knowing what signs to watch for. Looseness, persistent discomfort, changes in fit, or increased food trapping can indicate it’s time for an adjustment or replacement.
- How often: follow your dentist’s schedule for monitoring.
- What to watch: looseness, discomfort, fit changes, and gum irritation.
- Relines/repairs: may be needed for removable options as your mouth changes.
Frequently Asked Questions
What is a fake tooth called in dentistry?
In dentistry, a fake tooth is commonly referred to as a prosthetic tooth or dental prosthesis. The exact term depends on the device, such as an implant crown, bridge, denture, flipper, or an Essix retainer with a false tooth.
Can a fake tooth look natural?
Yes—well-made implant crowns and bridges can match color and shape closely, often looking very natural. Removable options can also look good from a distance, but they may be less seamless up close due to design and retention features.
What’s the difference between a flipper and a dental implant?
A flipper is a removable, temporary appliance used to improve appearance and basic function while you wait. A dental implant is a surgically placed artificial root that supports a permanent crown.
How long does an implant crown last?
With good oral hygiene and regular dental care, implant crowns can last many years and often decades. Longevity depends on bite forces, gum health, and whether maintenance visits are kept on schedule.
Will getting a fake tooth hurt?
Most procedures use local anesthesia, so discomfort during treatment is usually minimized. Soreness can occur after treatment, but modern techniques and proper aftercare often keep discomfort manageable.
Do I need bone grafting for an implant?
Sometimes—if bone volume is insufficient, your dentist may recommend bone grafting before or during implant placement. Imaging helps determine whether grafting is needed to support the implant safely.
What’s the fastest way to get a tooth back?
The fastest options are usually temporary solutions like a flipper or immediate temporary crown, depending on the case. Definitive options like bridges or implants take longer because they require planning, fabrication, and healing.
Are DIY temporary tooth kits safe?
DIY temporary tooth kits may provide short-term cosmetic coverage, but they can’t replace clinical assessment. Poor fit can irritate gums, and underlying gum or bone issues may go unnoticed—especially if pain or irritation occurs.
Fake Tooth Options Comparison (Quick Side-by-Side Table)
Compare by permanence, stability, and best use cases
| Option | Permanence | Stability | Surgery required | Bone preservation at gap | Typical timeline | Maintenance level | Best for |
|---|---|---|---|---|---|---|---|
| Implant (post + abutment + crown) | Permanent | High | Yes | Often supportive when conditions allow | Weeks to months | Moderate (daily hygiene + checkups) | Single to multiple teeth; long-term goals |
| Dental bridge (traditional) | Permanent (fixed) | High | No | Limited (does not replace root) | Often a few weeks | Moderate (cleaning under pontic) | Gaps where adjacent teeth are healthy |
| Resin-bonded/Maryland bridge | Permanent (fixed) | Moderate to high | No | Limited | Often faster than traditional bridges | Moderate (careful cleaning) | Selected front-tooth cases |
| Flipper / Essix retainer with a false tooth | Temporary | Low to moderate | No | Not applicable | Days to weeks | High (removal/cleaning; limited durability) | Interim appearance and basic function |
| Removable partial denture | Temporary to long-term (varies) | Moderate | No | Not root replacement | Weeks | High (daily cleaning; possible relines) | Multiple missing teeth; budget-friendly needs |
| Complete denture | Long-term (with adjustments) | Moderate | No | Not root replacement | Weeks | High (adjustments; daily cleaning) | Full arch tooth loss |
| DIY temporary snap-in kit | Temporary | Unpredictable | No | Not applicable | Immediate | High (fit checks; irritation risk) | Generally not recommended without evaluation |
Compare pros/cons in one glance
| Option | Top pros | Top limitations | Questions to ask your dentist |
|---|---|---|---|
| Implant crown | Natural feel, strong chewing, long-term potential | Surgery and healing time; higher upfront cost | Is bone volume sufficient? Will grafting be needed? What is the full timeline? |
| Traditional bridge | Fixed and stable; often faster than implants | Alters adjacent teeth; does not replace root | Which teeth will be prepared? How long is the expected lifespan? |
| Resin-bonded/Maryland bridge | Conservative approach; good for select cases | May debond; not ideal for heavy bite areas | Is this bridge type appropriate for this tooth location and bite? |
| Flipper / Essix retainer | Quick interim coverage; often affordable | Limited chewing strength; less stable | How long will it be used? What foods should be avoided? |
| Partial denture | Can replace multiple teeth; non-surgical | Bulkier; may affect speech; food trapping | Will clasps affect nearby teeth? How often are relines needed? |
| DIY temporary kit | Immediate cosmetic coverage | Fit/irritation risk; misses clinical evaluation | Is there a safer interim option for this specific situation? |
If a missing tooth is affecting your comfort, confidence, or daily routine, the next step is a personalized exam and treatment plan. Scheduling a consultation with your dentist can clarify what your “fake tooth” options are called in your case, which approach fits your bite and bone health, and what timeline is realistic for getting you back to eating and smiling with confidence.